Cellulitis is an infection of the dermal and subcutaneous skin layers that gives rise to red, swollen, hot, and painful skin.
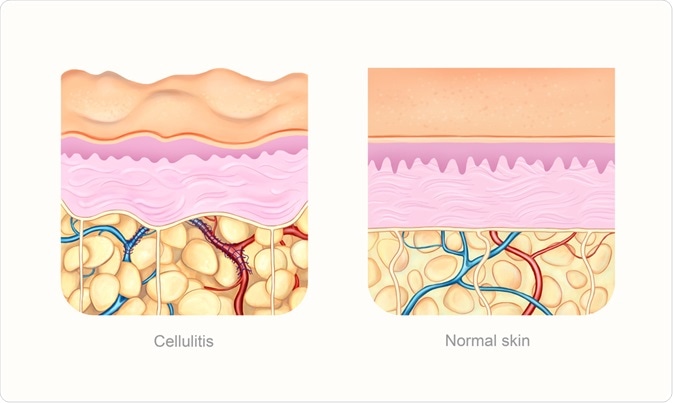
Image Credit: oliavolha / Shutterstock.com
Affected areas
Cellulitis sometimes develops on areas of broken skin due to an ulcer or surgical wound, for example, although this condition can also occur anywhere on the body or face where the skin remains intact.
The most commonly affected area is the lower leg, particularly where the tibia is located and in the foot. The next most frequently affected area is the arm, followed by the head and neck. Certain forms of cellulitis are sometimes named according to the body region affected such as buccal cellulitis, which affects the cheeks, or periorbital cellulitis, which affects the eye socket area.
Cellulitis can be dangerous if it is not treated promptly as it may spread and even lead to septicemia, which is a severe infection of the blood. Recurrent cellulitis infection can also eventually impair lymphatic drainage and cause chronic swelling in the affected area.
This condition is relatively common and affects individuals of all ages and races, although it is more common among middle-aged and elderly people.
Symptoms
The symptoms of cellulitis are inflammatory signs such as swelling, pain, tenderness, redness, and warmth. These symptoms may be accompanied by a fever, sometimes with sweats, chills, and swollen lymph nodes. Eventually, the red areas expand in size, and small red spots or small blisters may start to appear.
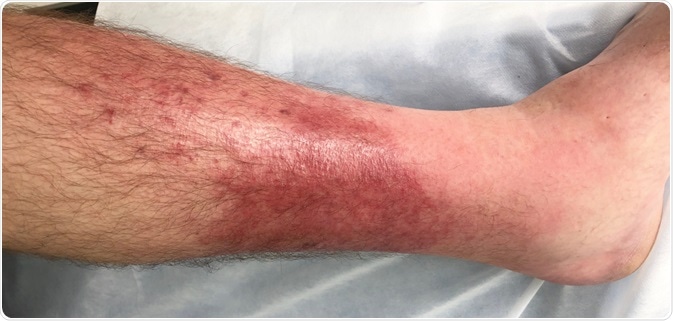
Image Credit: TisforThan / Shutterstock.com
Pathology of cellulitis
The skin is the largest organ in the body and is comprised of three layers which include the epidermis, dermis, and subcutis. Whereas the epidermis is the outermost layer of the skin, the dermis, or the middle layer of the skin, is where sweat glands, hair follicles, and blood vessels are contained. Thirdly, the subcutis or bottom skin layer contains fat and collagen, which provides protection and regulates body temperature.
Cellulitis develops when bacteria and sometimes fungi enter the skin surface through abrasions such as a cut or bruise. More specifically, the most common bacteria to cause this condition are beta-hemolytic streptococci.
Staphylococcus aureas, including the strains that are resistant to methicillin (MRSA), is another type of bacteria that commonly causes cellulitis. When MRSA has caused the infection, cellulitis can be difficult to treat due to the bacteria’s resistance to antibiotics.
Cellulitis can also be caused by many other types of bacteria such as Pasteurella multocida, which can be caught from a dog or cat scratch or bite. In children aged under 6 years, infection with Hemophilus influenza (H. flu) can also cause the condition. When H. flu is the cause, the arms, face, and upper torso are usually affected. Another example of a bacteria that can lead to cellulitis is Pseudomonas aeruginosa, which is a tough bacterial strain that survives in a range of environments and is often found in soil and stagnant water.
Risk factors
Several factors can increase the risk of cellulitis developing and these include:
- Injury – A cut, burn, fracture, or even scrape of the skin can increase the risk of infection because broken skin provides an entry point for bacteria.
- Weakened immune system – Conditions that lead to a weakened immune system increase the risk of infection. Some examples include chronic leukemia, human immunodeficiency virus (HIV) or acquired immunodeficiency syndrome (AIDS), diabetes, kidney disease, and circulatory disorders. Certain medications, such as corticosteroids, can also weaken the immune system.
- Obesity – Obese individuals are more likely to develop cellulitis, as these people are more likely to have reduced circulation of the blood and lymphatic fluid.
- Skin conditions – Some skin disorders that lead to breaks in the skin surface such as eczema, chicken pox, or athlete’s foot can increase the risk of cellulitis developing.
- Previous cellulitis infection – People with a history of cellulitis infection are more likely to suffer a future or recurrent infection, particularly if the area affected was the lower leg.
- Chronic swelling in the leg or arm – Swollen tissue is more likely to crack and expose the skin to infection with bacteria.
Treatment of cellulitis
Since cellulitis is usually caused by an infective bacteria, it is treated using antibiotics that are suitable for killing the organism. For fungal infections, antifungal agents are used.
In some cases, the antibiotic needs to be administered intravenously because oral administration does not always provide adequate penetration of the inflamed tissues. In all cases of cellulitis, doctors base their treatment choice on a combination of factors including general health status, the specific strain of bacteria, and the degree of infection.
References
Further Reading
Last Updated: Feb 23, 2023