A hernia refers to when an internal body part pushes through a weak area of muscle or the surrounding tissue wall. Hernias often do not cause any symptoms, although swelling may appear in the abdomen or groin.
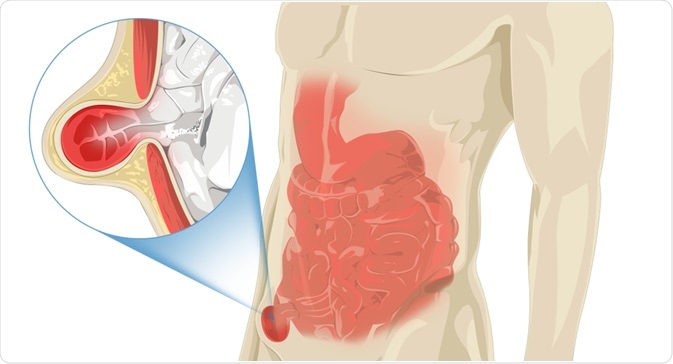 An inguinal hernia. Image Credit: Akora Illustration/Shutterstock.com
An inguinal hernia. Image Credit: Akora Illustration/Shutterstock.com
Although a hernia can develop anywhere in the body, they usually occur somewhere between the chest and hips, with abdominal hernia being the most common form. A weakness in the abdominal wall leads to a hole forming and abdominal organs or adipose tissue then push through the hole, creating a bulge. Hernias can also occur in other parts of the body such as the spine when the intervertebral discs protrude outwards and press on nearby nerves.
Most hernias are reducible, which means the herniated contents can be manipulated back into the abdominal cavity. Irreducible hernias, on the other hand, cannot be pushed back to their original location. This can lead to strangulation, which refers to when pressure placed on the hernial contents may compromise the blood supply to the tissue, leading to ischemia, cell death and even gangrene. Obstruction may also occur if part of the gut herniates and the bowel contents can no longer move through the herniated area. This can lead to cramps, absence of defecation and vomiting.
What happens in a hernia?
The pathophysiology of some of the most common types of hernias is described below.
Inguinal hernia
This is the most common form of hernia and refers to when bowel or fatty tissue protrudes into the groin. This type of hernia mainly occurs in men. A painful dragging sensation may be felt, as well as pain and swelling in the scrotum and testicles.
In cases of inguinal hernia, a loop of the intestine protrudes through a hole in the abdominal wall into the inguinal canal, which contains the spermatic cord. While a male fetus is in the womb, the testes are formed in the abdomen and before birth, they descend into the scrotum via the inguinal canal. The weakness that occurs in the abdominal wall may be present at birth or may develop later on in life.
An indirect inguinal hernia is one that occurs as a congenital lesion. It occurs as a result of the deep inguinal ring failing to close during embryogenesis after a testicle has moved through it. Once bowel or other abdominal tissue moves into and enlarges the empty space, a visible bulge forms and the hernia becomes clinically evident.
Direct hernias are acquired rather than congenital and usually occur in people aged 25 or older. This hernia occurs due to degeneration and fatty changes in the inguinal floor or posterior wall in an area called the Hesselbach triangle.
The majority of direct hernias do not have a true peritoneal lining and do not contain the intestine; they mainly contain preperitoneal fat and occasionally bladder. A long-standing direct hernia that has become large may extend into the scrotum and may also contain abdominal content or intestine.
Femoral hernia
These hernias also occur when part of the bowel or fatty tissue protrudes into the groin, although these are much less common than inguinal hernias and account for only 3% of all hernias. The fatty tissue or part of the intestine pushes through the wall of the femoral canal which houses the femoral artery, nerves and small veins. The femoral canal is found just under the inguinal ligament in the groin. Although femoral hernias can develop in men or women, they are more common among women due to the wider bone structure of the pelvis in females.
The different types of femoral hernia are described below:
- A reducible femoral hernia describes a femoral hernia that can be pushed back into the abdominal cavity. This may occur spontaneously or through manipulation. However, most cases occur spontaneously and the hernia is often painless.
- An irreducible femoral hernia is one that becomes stuck in the femoral canal and causes pain.
- An obstructed femoral hernia refers to when a bowel part becomes tangled up with the hernia and causes obstruction in the intestine. The obstruction can increase in size and become very painful. It may also cause vomiting.
- A strangulated femoral hernia occurs when the hernia blocks the supply of blood to part of the intestine. Strangulation of the intestine can lead to tissue death and gangrene and is a life-threatening condition that requires immediate surgical intervention.
Umbilical hernia
An umbilical hernia forms when part of the intestine or fatty tissue protrudes through an opening in the abdominal muscles near to the navel, causing the belly button to swell. This type of hernia may develop in babies if the opening that the umbilical cord passes through does not close properly after birth. This hernia can also affect adults, possibly due to repeated abdominal strain.
In children, umbilical hernia rarely causes complications, although complications can occur if protruding abdominal tissue becomes trapped and is not possible to push back into the abdominal cavity. This “incarcerated” tissue receives a reduced supply of blood which can lead to tissue damage and umbilical pain.
If the trapped tissue receives no blood supply at all (strangulation) gangrene may occur and infection may spread throughout the abdomen, which can be life-threatening. Incarceration or obstruction of the intestine is more likely to occur in adults and these individuals must receive emergency surgical intervention immediately.
Hiatus hernia
Hiatus hernia refers to when a part of the stomach protrudes into the chest via an opening in the diaphragm. The diaphragm has a small opening (hiatus) that the esophagus passes through to connect to the stomach. If the stomach pushes up through this opening, the result is a hiatus hernia.
A hiatus hernia may not present with any obvious symptoms. However, a large hiatus hernia can enable reflux of food and acid the esophagus, which can cause heartburn and lead to symptoms of gastroesophageal reflux disease (GERD).
The cause of this type of hernia is not completely clear, but it is thought that hiatus hernia may occur as a result of the diaphragm weakening due to pressure on the abdomen or aging.
What Is a Hernia and How Is One Repaired?
Who gets hernias?
Some of the factors that may lead to hernia are described below:
- Mechanical causes such as not lifting heavy weights correctly, hard coughing, incorrect posture or blows to the abdomen.
- Conditions that increase pressure in the abdominal cavity such as obesity, constipation, chronic lung disease and fluid build-up in the abdomen (ascites).
- Muscle weakness due to overexertion, poor nutrition or smoking, for example.
References
Last Updated: Dec 22, 2022