Pneumonia is a common infection of the lungs that affects millions of people worldwide. There are over 30 microorganisms that cause pneumonia, including several types of bacteria, viruses, and fungi.
These causative agents induce pneumonia by triggering an inflammatory response that results in the filling of the alveolar sacs with fluid or pus, thus limiting oxygen exchange.
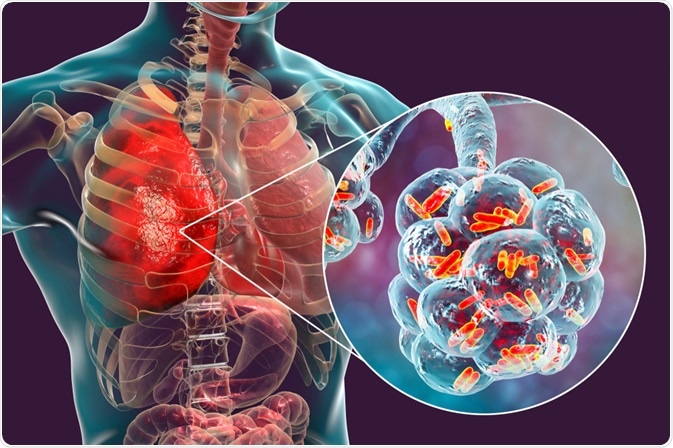
Image Credit: Kateryna Kon / Shutterstock.com
Although pneumonia is highly treatable in most patients, it can be a serious medical condition requiring hospitalization in patients who are under the age of 2, or those who are over the age of 65, have a weakened immune system, or who have a pre-existing chronic disease, such as heart or lung disease. In extreme cases, pneumonia can be life-threatening.
A pneumonia infection is classified based on how it is acquired and can be categorized into community-acquired, hospital-acquired, healthcare-acquired, or aspiration pneumonia.
Community-acquired pneumonia
Community-acquired pneumonia is an infection that is acquired outside of the healthcare system, including hospitals, nursing homes, outpatient clinics, or any other healthcare facility.
Community-acquired pneumonia is the most common type of pneumonia and generally presents as an acute infection, with symptoms appearing over the course of hours or days.
Streptococcus pneumonia is the leading cause of community-acquired pneumonia and is responsible for 20% to 60% of all cases. Haemophilus influenza, Staphylococcus aureus, Legionella pneumophila, Mycoplasma pneumonia, and several viruses are also leading causes of community-acquired pneumonia.
Up to 50% of patients with pneumonia have an unknown causative agent. Infection typically occurs through direct inhalation of the airborne microorganism, but it can also occur when a person accidentally inhales food or liquid from the mouth into the lungs.
This can deliver nasal or oral cavity-based bacteria into the lungs and is called aspiration pneumonia.
Hospital-acquired pneumonia
Hospital-acquired pneumonia is a lung infection that is obtained during a hospital stay. This form of pneumonia can be serious because oftentimes the patient, by nature of being in the hospital in the first place, is in an immune-weakened state due to illness or traumatic injury. As a result, the patient is often more susceptible to infection.
The bacteria responsible for this type of pneumonia are often resistant to first-line antibiotics, which can further complicate treatment regimens.
These infections can occur through inhalation of airborne organisms or contact with contaminated healthcare workers. Hospital-acquired pneumonia is also prevalent in patients who require a ventilator for breathing assistance. Ventilator tubes or other tubes that open a patient’s throat provide a direct point of access for airborne bacteria and viruses to enter the lungs.
The risk of ventilator-acquired pneumonia can be reduced by fastidious hand washing for all healthcare workers and family members who are exposed to the patient, frequent cleaning of the patient’s mouth, and thorough cleaning or replacing of equipment in between patients.
Types of Pneumonia (Medical Classification)
Healthcare-acquired pneumonia
Similarly, healthcare-acquired pneumonia is an infection obtained during a visit to an outpatient clinic, nursing home, or long-term care facility. This type of pneumonia commonly occurs in patients with chronic kidney disease.
Patients with chronic kidney disease often have weakened immune systems and are more susceptible to bacterial infection. In addition, patients must often undergo kidney dialysis, which requires frequent contact with the healthcare system.
Patients and their caregivers must practice exceptional hygiene and thoroughly clean all medical equipment. Given these precautions, dialysis patients are still at increased risk for infection just by the nature of the procedure and the potential for direct exposure to pathogens.
Pneumonia is the leading cause of death in dialysis patients. It is strongly recommended that patients with chronic kidney disease receive a pneumonia vaccine and a yearly influenza vaccine.
References
Further Reading
Last Updated: May 22, 2021