Refractory acute myeloid leukemia (AML) is a very challenging complication in the management of AML. In this condition, the disease is refractory or resistant and patients fail to achieve complete remission following initial treatment.
Most AML patients experience an absence of symptoms post initial treatment with multiple drugs. However, about 10% and 40% of AML patients do not respond to initial therapy and are thus categorized as refractory or resistant to treatment.
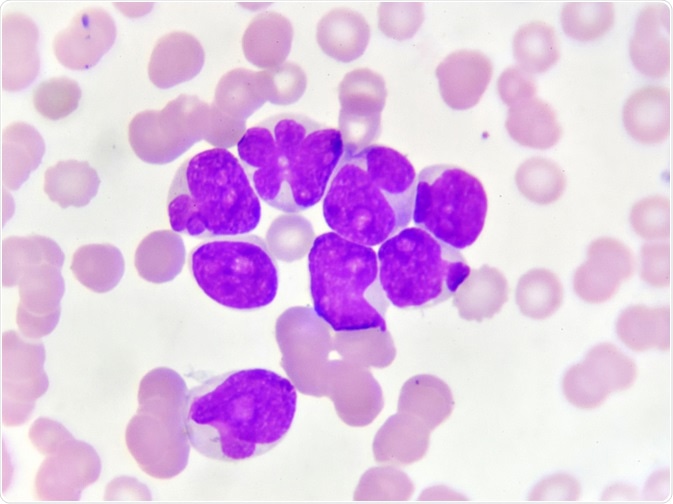 Microscope of acute myeloid leukemia (AML). Image Credit: Jarun Ontakrai / Shutterstock.com
Microscope of acute myeloid leukemia (AML). Image Credit: Jarun Ontakrai / Shutterstock.com
Management of refractory AML
It is very stressful for patients to be diagnosed with refractory leukemia. The health care team consisting of physicians, nurses, and social workers needs to provide support to the patients and their families and encourage them to have open discussions.
Talking to other patients diagnosed with the resistant form of the condition or joining local support groups may also help. It is important to discuss a fresh treatment plan with doctors who have experience dealing with this particular form of AML. Taking part in clinical trials is an option for some patients. Patients are also advised to get a second opinion from another doctor before starting any new treatment.
The new treatment plan may involve new types of drugs that were not used during primary therapy and other drugs that are undergoing tests in clinical trials. Palliative care is crucial to help manage symptoms and side effects of treatment and thus optimize the quality of life of the patient.
New treatment plans must be carefully devised after taking into account several factors, such as the patient’s age, preference, cytogenetic findings, response to drugs, molecular profile. Therapy needs to be customized for each patient depending on their specific disease details. Some of them may not be fit for intensive chemotherapy.
Dr. Ravandi on Relapse/Refractory AML
Allogeneic stem cell transplantation
Allogeneic stem cell transplantation is a treatment option for people diagnosed with refractory AML.
This involves the transfer of stem cells from a healthy donor to the patient’s body after intensive radiation or chemotherapy. This procedure is used to treat high-risk AML patients who do not fully respond to initial treatment or patients in whom a relapse of the disease is found post previous successful treatment. It can be a risky procedure due to the high-intensity chemotherapy or radiation given prior to stem cell transplantation. Intensive radiation and chemotherapy cause severe side effects and also impair the ability to produce one’s own stem cells.
The main objective of this intensive therapy is to deactivate the immune system, thus preparing it to receive new stem cells. It reduces the possibility of graft rejection, kills the remaining cancer cells so as to prevent a recurrence of cancer, and enables an overall successful transplant.
Stem cells to be transplanted can be gathered from blood, bone marrow, or blood from the placenta or the umbilical cord. Finding a bone marrow donor is an important step in allogeneic stem cell transplantation. Siblings, if any, are usually a potential match as they share the same genes. If this is not an option, volunteer donors will need to be found using search registries. Potential donors need to undergo comprehensive blood tests and physical examination before stem cell collection to rule out any serious infectious diseases.
Adverse effects of stem cell transplant
Since the immune system of the donor is also transferred during stem cell transplant, adverse immune reactions caused by the donor cells against the patient’s body tissues are possible. This is minimized by pharmacotherapy post-transplant.
Allogeneic stem cell transplant is not advised for patients whose overall health condition is poor or older patients, because they might not be able to tolerate the intensive therapy given prior to transplant. In some older patients, the use of a low-intensity stem cell transplant may be appropriate.
References
Further Reading
Last Updated: Jan 27, 2021