Some patients with scoliosis will need surgery to correct particularly severe spinal curvature associated with the condition, or to foster healthy growth of the spine for younger patients.
There are many possible reasons that surgery may be recommended for an individual with scoliosis. These include:
- Curve affects the ability to breathe normally
- Curve interferes with the care of patients with spina bifida or cerebral palsy
- High likelihood of progression
- The individual may find the spinal curve cosmetically distressing
Surgery is usually able to correct the curvature of the spine significantly, but it is rare for the spine to become completely straight as a result of the surgery.
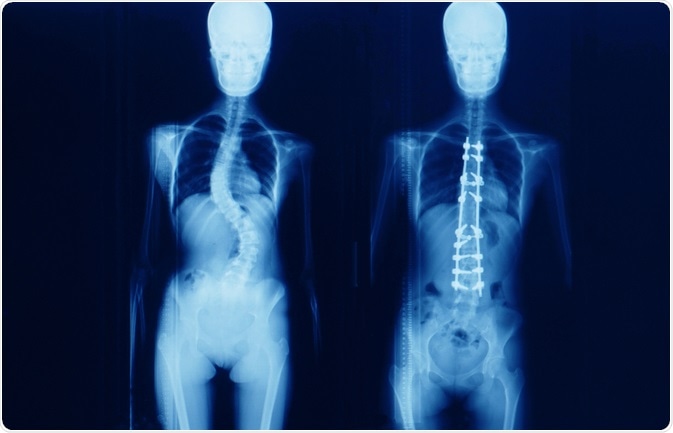 Image Credit: Yok_onepiece / Shutterstock.com
Image Credit: Yok_onepiece / Shutterstock.com
Surgery for scoliosis in young children
For children less than ten years of age - before they have reached the growth spurt prior to puberty - surgery involving the insertion of growing rods may be beneficial. These rods are designed to control the growth of the spine and correct future growth to minimize curvature. The initial procedure is usually conducted in a day or overnight surgery, and the rods are inserted by way of a small incision.
A specialist will be then required to monitor the growth of the child two to three times a year and lengthen the rods as needed to support the child’s growing spine. The lengthening process can be very simple, especially if magnets are used to extend the rods, without the need for internal procedures.
It is usually recommended that children with growth rods wear a brace to help protect the rods and provide further support to their spine. When the child stops growing at approximately 16-17 years of age, the rods can be removed entirely. In some cases, growth rods are sufficient as the sole surgery to support spinal growth but other patients will require corrective spinal fusion therapy.
Ch. 4 - What is Scoliosis Surgery?
Spinal fusion in scoliosis
Spinal fusion is the most common surgery for patients with scoliosis that have finished growing and involves a graft of bone onto the spinal vertebrae that eventually heal together to form a solid, rigid mass of bone. Although this process may restrict the movement of the spine, it prevents the curvature from becoming worse and may correct severe cases.
There are two main techniques that may be used: anterior fusion provides access to the spine via an incision on the side of the chest wall, and posterior fusion utilizes an incision on the back and metal instruments for the curve correction. The bone graft can be attached to the spine with a combination of metal rods, screws, hooks and wires, which are left in place permanently.
This is a major surgery that can take several hours and usually requires intensive care in the recovery period. It can take several weeks for patients to return to acceptable physical standards to go back to school. Non-contact sports can be recommenced approximately eight weeks after the surgery and contact sports should be avoided for up to a year.
There are several risks that are associated with spinal fusion therapy, which include:
- Bleeding - patients may require a blood transfusion
- Infection - patients may require antibiotic treatment
- Movement of the implant - patients may require correctional surgery
- Failure of the graft to fuse - patients may require correctional surgery
- Spinal nerve damage - patients may experience permanent nervous symptoms including incontinence and numbness or paralysis of the legs
As with any treatment option, it is critical to consider the specific risks and benefits for each individual patient in order to guide the decision of whether to undertake surgery for scoliosis.
References
Further Reading
Last Updated: Mar 31, 2023