A vasectomy represents a surgical procedure for male sterilization and is considered to be the most reliable form of male contraception. During this procedure, the vas deferens tubes that connect the testes with the urethra are divided and subsequently occluded in order to prevent spermatozoa from entering into the semen.
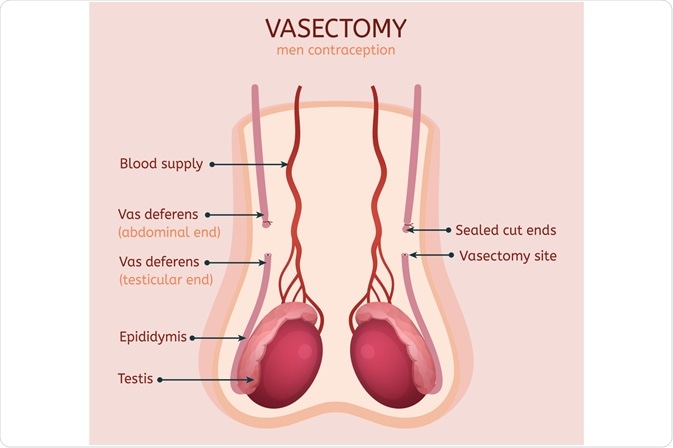
Image Credit: Double Brain / Shutterstock.com
A brief history
xIn one form or another, this procedure has been performed for over 100 years; however, the main advance in male sterilization was seen in 1974 in China with the rise of non-scalpel vasectomy. Following its success, this technique was eventually introduced in 1985 in the United States, and in 1995 in the United Kingdom.
Unlike other areas of minor surgery where proper patient care includes clinical appraisal, presumptive diagnosis, and surgery, a vasectomy instead involves the patient undertaking his own assessment and diagnosis. Therefore, it is pivotal that the specialist offering this service provides comprehensive counseling to fully inform the patient.
Indications, contraindications and practical considerations
Motivations for having a vasectomy differ for each individual; therefore, the decision has to be made in a situation without any compulsion or stress. In general, a vasectomy is indicated for any fully informed man who does not want to father any children and who desires an inexpensive outpatient method of voluntary permanent surgical sterilization. It must be stressed that respect for the patient’s personal decision is essential.
Naturally, there are no absolute contraindications; however, men of a younger age of less than 30 years, as well as those who do not currently have children nor are in a relationship, the presence of certain severe illnesses and scrotal pain can be considered as relative contraindications. Specific anatomic abnormalities, large varicoceles, and hydroceles, as well as acute skin infections, are also considered contraindications for this procedure.
Extreme consideration has to be taken with patients who are on anticoagulant or antiplatelet medications. Moreover, alternative methods of birth control, possible surgical complications, and failure rates should be thoroughly discussed. Needless to say that emotional instability and equivocal feelings about permanent sterilization must be addressed, and written informed consent is recommended.
Vasectomy methods
In general, this procedure can be performed as an open vasectomy or as a non-scalpel vasectomy using fine sharp instruments to puncture the skin and deliver the vas for ligature. This later form of a vasectomy involves the physician excising a segment of vas and repositioning the ends of the vas either with or without ligation, with the latter known as open-ended vasectomy.
A vasectomy can be done in an outpatient setting using local anesthesia, while general anesthesia is required for specific indications. Certain techniques that can be applied for discontinuation of the deferential ducts are interposition of tissue to prevent recanalization, excision of a piece of vas deferens and its subsequent ligation, as well as cautery of the luminal side.
Mutual comparison of different methods has not shown convincing superiority of one particular approach in terms of preventing pregnancy. Still, post-vasectomy semen analysis has shown that the occlusion failure is the highest in methods with simple excision and ligation with sutures or clips, whereas techniques combining fascial interposition and cautery have the lowest failure rate.
Following a short recovery period, more than 80% of patients return to normal activities within one week. An indispensable part of the follow-up is a semen analysis, which is ideally performed three months after the procedure in a certified laboratory. Men can be given clearance if no spermatozoa are observed in the ejaculate.
References
- http://www.aafp.org/afp/1999/0701/p137.html
- http://www.aafp.org/afp/2006/1215/p2069.html
- http://www.vasectomie.net/Sokal_Labrecque_%20vasectomyocclusiontechnique_2009.pdf
- https://uroweb.org/
- Kabir A. Vasectomy: No Scalpel Method. In: Salam MA, editor. Principles and Practice of Urology, Second Edition, Volume One. Jaypee Brothers Medical Publishers (P) LTD, 2013; pp. 705-708.
- Spooner L, Feltbower T. Vasectomy: knowledge. In: Botting J, Schofield J, editors. Brown's Skin and Minor Surgery: A Text and Colour Atlas, Fifth Edition. CRC Press, Taylor & Francis Group, LLC, 2015; pp. 161-168.
Further Reading
Last Updated: Mar 11, 2023