Asthma is a disease that affects your lungs. It is the most common long-term disease of children, but adults can have it too. Asthma causes repeated episodes of wheezing, breathlessness, chest tightness, and nighttime or early morning coughing; these episodes are also known as exacerbations or attacks.
The severity of exacerbations can range from mild to life-threatening. Both the frequency and severity of asthma symptoms can be reduced by the use of medications and by reducing exposure to the environmental triggers of asthma attacks.
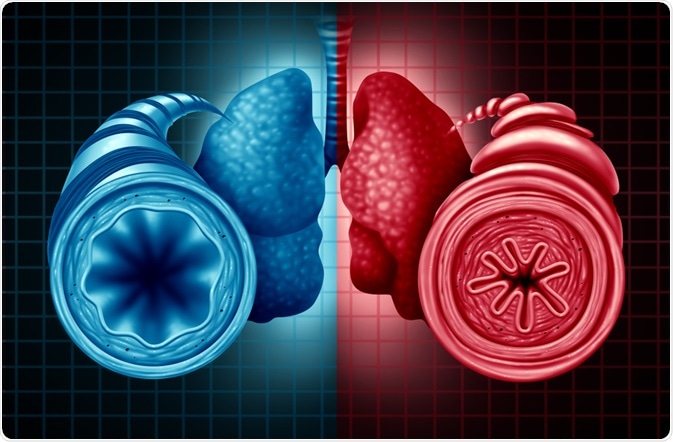 A healthy bronchial tube (left) and an unhealthy bronchial tube (right) with a breathing issue caused by respiratory muscle tightening. Image Credit: Lightspring / Shutterstock.com
A healthy bronchial tube (left) and an unhealthy bronchial tube (right) with a breathing issue caused by respiratory muscle tightening. Image Credit: Lightspring / Shutterstock.com
Epidemiology of asthma
About 20 million Americans have asthma and approximately 300 million people suffer from it worldwide. Nearly 7 million of these are children, although many children outgrow asthma in their teen years. Each year, 5,000 people die from asthma and it tends to run in families.
Asthma is one of the leading chronic childhood diseases, a major cause of childhood disability, and places a huge burden on affected children and their families, limiting the child’s ability to learn, play and even sleep. Collectively, children miss about 13 million school days each year because of asthma.
Black people are diagnosed with asthma at a 28 percent greater rate than the rate in white people. Black children are hospitalized for asthma at 250 percent of the rate, and die at 500 percent of the rate, of white children.
Pathophysiology of asthma
Inflammation of the lining of the airways is a major factor in asthma. This inflammation is produced by your immune system.
How does asthma work? - Christopher E. Gaw
The immune system's job is to defend your body against things that it sees as foreign and harmful, for example, bacteria, viruses, dust and chemicals. It does this by sending special cells to the organs that are being affected by these things. These cells release chemicals that produce inflammation, or swelling, around the foreign substance or substances to isolate and destroy them.
Although inflammation is a defense mechanism for our bodies, it can be harmful if it occurs at the wrong time or stays around after it is no longer needed.
Because our lungs are used to breathing in air with irritants, such as bacteria, viruses, pollens, and dusts, all day every day, they have developed ways of dealing with these things, and normally, an inflammatory response does not occur.
But the airways in the lungs of people with asthma are more sensitive to many of these things, and the immune system in these people overreacts by releasing many different kinds of cells and other chemicals to the airways.
These cells cause the following changes in your airways:
- The inner linings of your airways become swollen or inflamed (inflammation), leaving less room in the airways for the air to move through.
- The muscles surrounding the airways tighten up, which narrows the airways even more. (This is called bronchospasm.)
- The mucus glands in the airways may produce lots of thick mucus, which further blocks the airways.
These changes make it harder for you to breathe. They also make you cough and wheeze and feel short of breath.
People with asthma can develop ongoing inflammation that makes the airways super sensitive. As a result, if the inflammation is not treated, each time your airways are exposed to your asthma triggers, the inflammation increases, and you are likely to have symptoms. (This is called bronchial hyperresponsiveness.)
Because inflammation plays such an important role in asthma, treatment for most people with asthma includes taking medicine every day for a long time to reduce and control it.
Asthma is a chronic disease, like diabetes and high blood pressure. This means that once you develop asthma, you are likely to have it for a lifetime. It cannot be cured. Even when it is not causing symptoms, even when you are feeling just fine, the asthma is still there and can flare up at any time.
Asthma sufferers have trouble breathing because of the narrowing of the airways from their bronchioles, the open airways of the lung, an example of which is shown in the upper left. In chronic asthma (lower left), repeated cycles of inflammation, damage and repair lead to airway remodeling and fibrosis, the buildup of collagen and other materials surrounding the bronchioles.
A chronic condition like asthma requires daily attention. Depending on how severe your asthma is, that may include monitoring your breathing and taking medicine every day, even when you do not have symptoms. Taking care of your asthma must become a routine part of your life, just like monitoring and taking diabetes or blood pressure medicines are for people with those chronic conditions.
Doctors still do not know what causes some people to develop asthma. They think that many different genetic and environmental factors play a role.
Researchers are working hard to identify the responsible genes. They have also made progress in identifying other factors that seem to either lead to the development of asthma or can possibly protect people against developing asthma.
Asthma triggers
The most important factor in the development of asthma is probably atopy. This is the inherited tendency to be allergic. So if other people in your family have allergies, you may have inherited a tendency to be allergic, and your chances of developing asthma are greater than average.
Researchers also are beginning to see that exposure to certain irritants when you are very young may play a role in the development of asthma. If you have a family history of asthma or allergies and your mother was exposed to certain irritants, such as tobacco smoke, when she was pregnant with you, you may be more likely to develop asthma.
Exposure to certain indoor allergens in early childhood may also play an important role in the development of asthma. In many places, exposure to house dust mites appears to have this effect. Other indoor allergens that may play an important role in the development of asthma include cat dander, cockroach droppings, and mold.
Exposure to irritants, certain chemicals, or substances in your workplace may increase your chances of developing occupational asthma.
Changes in the way we live and work in the United States today may also increase our exposure to these allergens and irritants. For example, we now spend far more time indoors than we used to, and we have reduced ventilation in our homes and workplaces to conserve energy. This may trap allergens and irritants inside.
Researchers have also found a link between asthma and obesity. Some think that being obese may increase your chances of developing asthma, while others argue that people with asthma may not be active enough, and, as a result, they become overweight. This is an issue that is now being studied.
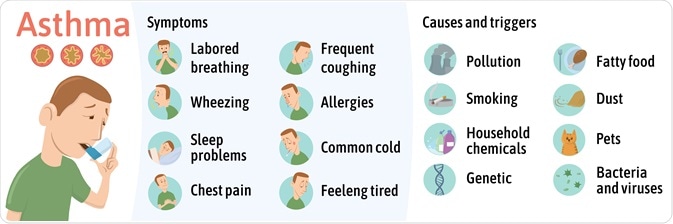 Infographic of the symptoms and triggers of asthma. Image Credit: Good_Stock / Shutterstock.com
Infographic of the symptoms and triggers of asthma. Image Credit: Good_Stock / Shutterstock.com
Protective factors against asthma
On the other side of the coin, medical research has identified factors that seem to help protect us against developing asthma. For example, they think that children who are exposed to certain types of infections and environments during their first year or two of life may be less likely to develop asthma.
As an example, research has shown that many children who grow up on or near farms and are exposed to livestock and poultry are less likely to develop asthma and allergies. The same appears to be true of children who have two or more older siblings or attend daycare during their first 6 months.
This discovery has led to the theory that our western lifestyle- with its emphasis on hygiene and sanitation-has resulted in changes in our living conditions and an overall decline in infections in early childhood. Many young children no longer experience the same types of environmental exposures and infections that they did in years past.
This affects the way their immune systems develop during very early childhood and may increase their chances of developing atopy and asthma. This is especially true of people who have close family members with one or both of these conditions.
This theory is called the "Hygiene Hypothesis." It may help explain why asthma has been on the increase in recent years.
Further Reading
Last Updated: Jan 28, 2021