The type of bariatric surgery that is used to help extremely or morbidly obese individuals lose weight depends on a number of factors, with each type of surgery associated with advantages and disadvantages. Patients and healthcare providers need to discuss the risks and benefits of procedures before deciding on the most suitable type of surgery.
Open and laparoscopic surgery
An open surgery involves cutting open the abdomen and making modifications to the digestive tract. This involves making a single, large incision across the abdomen that may later take time to heal and may also lead to complications such as hernias.
A laparoscopic surgery involves distending the abdomen with an inert gas and making several small half-inch incisions across it to enable insertion of surgical instruments and a small camera that can be used to aid the operating surgeon. Today, most bariatric surgery is laparoscopic because compared to open surgery, it requires smaller incisions that heal faster, are associated with fewer post-operative complications (especially hernias) and allow for early hospital discharge.
However, not all patients are suitable for laparoscopy. Extremely obese individuals, those with complex medical problems such as severe heart and lung disease or those who have previously had abdominal surgery may require the open surgery approach.
Types of bariatric surgery
There are four types of operations that are commonly offered to patients:
- Adjustable gastric banding
- Roux-en-Y gastric bypass
- Biliopancreatic diversion with a duodenal switch
- Vertical sleeve gastrectomy
Factors that are considered when choosing the surgery include:
- Benefits and risks associated with surgery type
- Patient preference and willingness to adhere to the post-surgery dietary recommendations
- Body mass index
- Eating habits
- Health conditions related to obesity
- Previous stomach surgeries
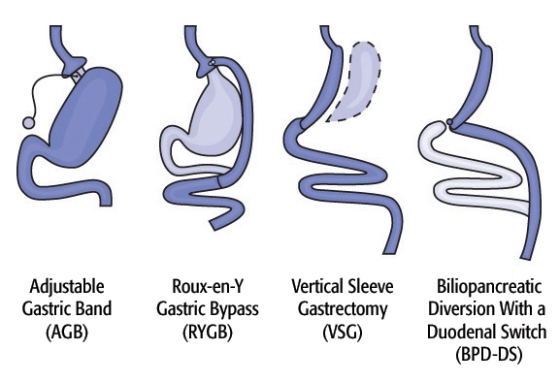
Diagram of Surgical Options. Image credit: Walter Pories, M.D. FACS.
- Adjustable Gastric Banding (AGB)
The basic principle of this type of surgery is to decrease food intake with the use of a small bracelet-like band placed around the top of the stomach. The band restricts the size of the opening from the throat to the stomach, limiting the amount of food a patient can ingest. The size of the opening can be modified using a balloon inside the band that can be inflated or deflated with saline solution according to the needs of the patient.
- Roux-en-Y Gastric Bypass (RYGB)
This method is also used to decrease food intake and involves creating a small pouch that is similar in size to the pouch created with AGB. The food bypasses the rest of the stomach and reaches the small intestine, where it is absorbed to a much lesser degree than if it had passed through the stomach, duodenum, and upper intestine.
- Vertical Sleeve Gastrectomy (VSG)
This procedure involves removal of most of the stomach, which not only restricts food intake and absorption, but lowers levels of the hormone ghrelin that is responsible for appetite.
- Biliopancreatic Diversion with a Duodenal Switch (BPD-DS)
Also called the duodenal switch, this three-stage procedure involves the removal of a large part of the stomach which makes the patient feel full after eating only a small meal, followed by re-routing of the small intestines to prevent food absorption. The third step involves changing how bile and other digestive juices affect the process of digesting and absorbing calories.
Further Reading
Last Updated: Jun 19, 2023