Intracerebral hemorrhage (ICH) is sudden, catastrophic bleeding that occurs in the brain tissue or ventricles. Symptoms may be sudden and severe, such as headache, loss of consciousness, or vomiting, but can also be milder, resembling ischemic stroke.
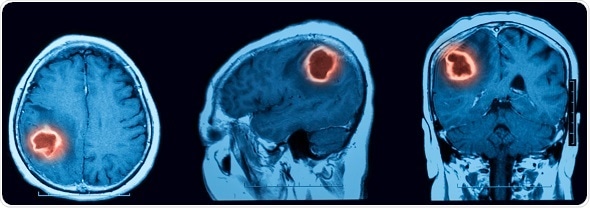
©MRI scan of cerebral hemorrhage - Suttha Burawonk /Shutterstock.com
Primary ICH
A primary ICH is not caused by any type of underlying deformity or coagulation disorder. Eighty percent of primary ICH cases are caused by hypertensive arteriosclerosis and cerebral amyloid angiopathy (CAA). Patients with CAA are often older, with a large hemorrhagic volume.
Conversely, those with ICH caused by hypertension are often younger, with the basal ganglia involved, and with smaller hemorrhagic volumes. Hypertension creates high pressure in the circle of Willis, a circular blood vessel system that supplies blood to the brain. The high pressure leads to smooth cell proliferation, which eventually causes cell death, leading to hemorrhage.
Secondary ICH
Secondary ICH is caused by an underlying problem with the blood vessels. That could be something such as an ischemic stroke that begins to leak, a brain tumor, or a blood-clotting disorder.
The majority of secondary ICH cases are caused by arteriovenous malformations (AVM)--abnormal direct connections between arteries and veins. Another type of malformation, called a cavernous malformation, is created by capillaries that have open pores, increasing their permeability. These are called sinusoidal vessels.
Risk factors
The main risk factors for ICH are age, male sex, high blood pressure, and alcohol intake.
Heavy drinkers are at particular risk of ICH at a young age. A study of people who consumed three or more alcoholic beverages per day showed a significantly increased risk of ICH, and had their strokes at an average age of 60 years, or 14 years earlier than the general population average of 74 years. Drinkers and non-drinkers had similar lengths of hospital stay and similar complications, but heavy drinkers were more likely to die within 2 years.
Hypocholesterolemia (low cholesterol) has been linked to ICH in people under 40 years. One theory explaining this connection is that high blood pressure and low cholesterol levels weaken the endothelium in the arteries.
Pregnancy can increase the risk for some types of stroke, although the overall incidence is low. Hypertension, as in pre-eclampsia and eclampsia, can lead to stroke in pregnant and post-partum women. Rupture of a vascular malformation and cerebral venous thrombosis are other causes of ICH seen in pregnant women.
Sympathomimetic drugs are associated with some risk of ICH, with amphetamine-like agents as the most commonly implicated. The mechanism of this effect is not known.
Recreational drugs can also increase the risk of ICH. In a retrospective study of cocaine-associated ICH, patients had higher blood pressure when admitted to the hospital, more subcortical hemorrhages, and higher rates of intraventricular hemorrhage. They were nearly three times more likely to die during their hospitalization than ICH patients who had not taken cocaine.
ICH in children
Stroke is one of the top ten causes of death in childhood, and roughly half of childhood strokes are hemorrhagic. ICH in children is usually caused by arteriovenous malformation, blood disorder, or a brain tumor. Other possible causes include hemangioma, infection, vasculopathy, vasculitis, and illicit drug use.
Further Reading
Last Updated: Feb 26, 2019