Introduction
Progression of Gingivitis
Symptoms of Gingivitis
Treatment for Gingivitis
References
Gingivitis refers to inflammation and irritation of the gums that surround our teeth. As one of the diseases that can affect the periodontium (which includes the gums, soft tissue, and bone around the teeth), gingivitis is classified as a form of periodontal disease. Gingivitis can cause gums to recede and lead to permanently damaged teeth.
Periodontal diseases are often classified depending on their severity, ranging from a mild case of gingivitis to severe periodontitis and acute necrotizing ulcerative gingivitis, which can be a dangerous and life-threatening condition.

Image Credit: Pixel-Shot/Shutterstock.com
Progression of Gingivitis
Gingivitis usually occurs before periodontitis develops, and not all cases of gingivitis progress to periodontitis. When gingivitis is only in the early stages, bacteria present in plaque cause inflammation of the gums, which may then bleed on brushing. However, even though the gums may be irritated, the teeth they surround remain fixed in their sockets, and no irreversible damage to the gums or other surrounding tissue has occurred at this stage.
If gingivitis is not treated, periodontitis may develop and the inner layer of gum and the surrounding bone loosen around the teeth. This creates pockets of space between the teeth and gums, where debris collects, leading to plaque and infection. Bacteria or toxins produced by the plaque begin to break down the bone and surrounding connective tissue that holds the teeth firmly in their sockets, and as the condition advances, the pockets become deeper and more bone and gum are destroyed. Eventually, the teeth loosen from their sockets, and tooth loss occurs.
It is therefore vital to detect gingivitis in the early stages so that early treatment can be initiated to increase the chance of full recovery and decrease the risk of recurrence.
Symptoms of Gingivitis
Healthy gums should appear pink, firm, and attached to the lower ends of the teeth that they are holding in place. There should be no bleeding when the teeth are brushed normally. In cases of gingivitis, however, the gums become red, swollen, or infected and tend to bleed easily when brushed. A foul odor or taste in the mouth may also develop, as well as plaques or white spots on the gums. It is also possible to develop gingivitis that does not present with any symptoms, so it is vital to regularly attend dental appointments and check the health of the gums and teeth
.
Some examples of gingivitis symptoms are listed below:
- Red and swollen gums
- Painful gums, especially to touch
- Gums that bleed on brushing or flossing
- Gums that have peeled or recessed at the lower ends of the teeth
- A bitter or unpleasant taste in the mouth due to discharge from bacteria within the mouth
- Bad breath caused by gases given off by bacteria
- The presence of hardened plaque called tartar, visible as grey or brown discolorations across the teeth
- If the gingivitis has progressed, the teeth may have become loose due to the gums receding at the lower ends of the teeth. This may cause difficulty eating.
- Excessive salivation
- Difficulty in speaking, eating, or chewing due to pain
- Gum abscesses filled with pus that may be swollen and painful
- Swollen gums and painful ulcers - a condition called "trench mouth"
In acute necrotizing ulcerative gingivitis, symptoms include bleeding, pain, receding gums, ulcers, and difficulty swallowing or chewing. Other disease features include a metallic taste in the mouth and severe bad breath or halitosis.
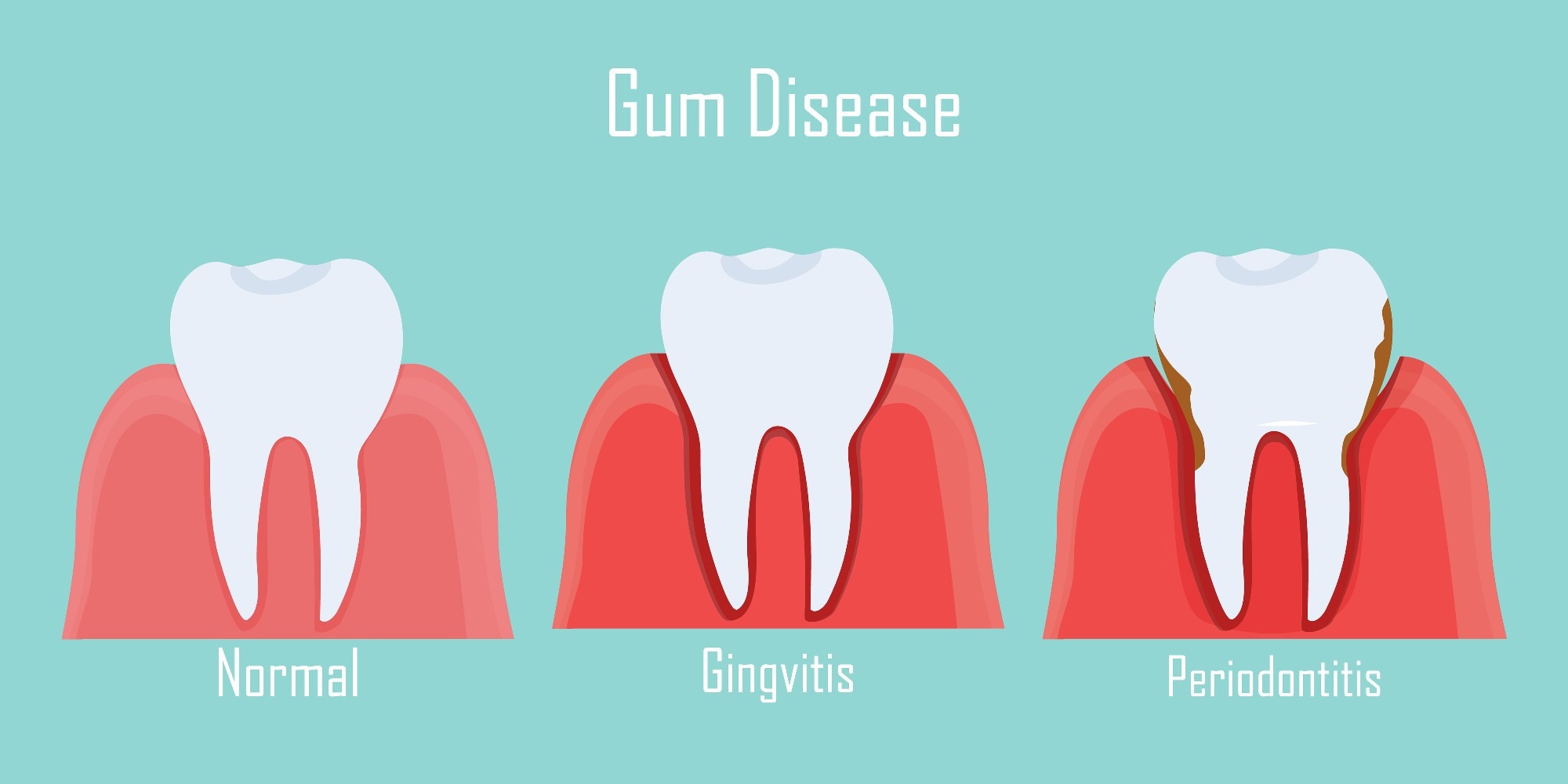
Image Credit: AlyonaZhitnaya/Shutterstock.com
Treatment for Gingivitis
The symptoms of gingivitis are alleviated by removing the source of infection. Regular visits to the dentist are essential to ensure accumulated plaque is removed to combat the condition. Once the plaque has been removed, the teeth should be brushed and flossed regularly to minimize further plaque formation. In cases of advanced gingivitis, antibiotics may be required to combat the infection and reduce plaque.
References:
- Gum disease (2018). Available at: https://www.nhs.uk/conditions/gum-disease/ (Accessed: 4 August 2022).
- (2022) Healthinfotranslations.org. Available at: https://www.healthinfotranslations.org (Accessed: 4 August 2022).
- (2022) Medicinenet.com. Available at: https://www.medicinenet.com/gum_disease/article.htm#what_are_the_signs_and_symptoms_of_gum_disease (Accessed: 4 August 2022).
- An Overview of Gum Disease (2022). Available at: https://www.webmd.com/oral-health/guide/gingivitis-periodontal-disease (Accessed: 4 August 2022).
- What Is Gingivitis? Treatment, Symptoms, Home Remedies & Causes (2022). Available at: https://www.emedicinehealth.com/gingivitis/article_em.htm (Accessed: 4 August 2022).
Further Reading
Last Updated: Mar 9, 2023