Contact dermatitis is a condition in which the skin suffers inflammation, becoming red, itchy, swollen, and perhaps developing rashes, after coming into contact with a specific substance. It is known to be of two major types; irritant or allergic contact dermatitis.
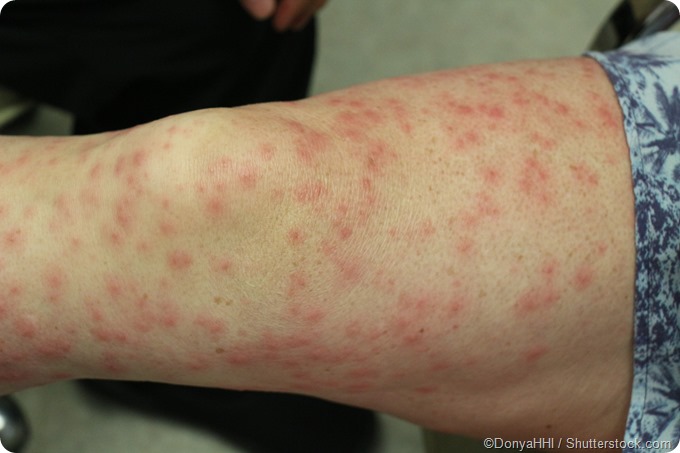
Irritant contact dermatitis
This is quite common - it is more frequently encountered than the allergic type of contact dermatitis. It is a result of irritation and breach of the skin surface by a substance. For this reason, the nature and extent of the rash depend on how much of the irritant was present, and the duration of exposure.
This type of reaction shows no characteristic time lapse between exposure and the onset of dermatitis. Factors which may hasten the reaction or themselves act as irritants include exposure through wet skin, dry skin, and extreme climatic conditions.
Typical irritants include:
- Chemicals such as acids or alkalis which burn the skin, including soaps and detergents
- Fabric treatment chemicals such as fabric softeners, or solvents
- Shampoos
- Cement
- Hair dye
- Wetness as in prolonged use of diapers
- Weedicides or pesticides
- Gloves made from rubber
Cause
The rash or skin reaction is in response to skin irritation induced by the chemical.
Allergic contact dermatitis
This is a delayed or type IV hypersensitivity reaction carried out by T-lymphocytes in the epidermis. These cells come into contact with the antigen which has bound to the cell surface to form a new immunogen.
Sensitizing agents may include:
- Adhesives such as those used for cosmetic aids such as attached wigs
- Certain topical antibiotics
- Certain resins
- Clothing
- Fragrances used in perfumes, soaps, or cosmetics
- Other cosmetics including nail polish, or hair treatment agents
- Nickel, chromium, or other metals
- Poisonous plants such as poison ivy, or poison sumac
- Rubber or latex gloves or shoes
Cause
The contact between skin immune cells and specific antigens on the sensitizer provokes an immune-mediated or allergic reaction.
The reaction takes place in two phases, as is shown below:
- Sensitization – this is when the immune cells react to the hapten in a specific manner. During this phase, non-specific immune cells pick up the hapten-carrier protein complex and migrate to the local lymph nodes. There they activate antigen-specific lymphocytes to produce a proliferative clone of T-cells which enter the circulation and enter the dermis. The sensitization process is now complete, and the new T-cells are ready to respond to the antigen if they encounter it. The whole process takes about 10-14 days.
- Elicitation – this phase follows re-exposure to the antigen. The prepared T-cells mount an immune challenge which produces the allergic reaction. Increasing use can lead to persistent or severe reactions. This phase takes 24-48 hours, on average, the first time the antigen is picked up following sensitization. However, subsequent exposures bring about more rapid reactions, which is called anamnesis.
Photosensitivity reactions
These are a type of skin allergy in which the causative product causes a reaction only if the skin is concurrently exposed to ultraviolet or other forms of radiation present in sunlight. Some culprits include:
- Sunscreen ingredients
- Shaving lotions
- Sulfa-containing ointments
- Coal tar products
- Some natural oils and certain perfumes
Symptoms
Allergic reactions are either acute (within 24-48 hours), or require some days or months to first manifest. Such reactions are typically very pruritic, papular, and ill-defined. The skin is reddened. Vesicular and oozing lesions may occur. Ulceration is rare. However, higher concentrations of some allergenic substances may give rise to irritant reactions as well.
Irritant contact dermatitis is more often associated with burning or stinging as well as, or instead of, itching. The skin may be fissured, as well as rough and dry. Redness, oozing lesions, and inflammation may develop with chronic irritant contact dermatitis. Pain may be present if the skin is cracked and cut, and the area is usually very tender.
Both forms of contact dermatitis are found on the parts of the body that are exposed to the causative agent. The hands, especially the interdigital webs, are thus a typical location. Eczematous lesions with oozing, papules, crusting, or thickening, are often present.
Distinctions between irritant and allergic contact dermatitis
The following table summarizes some primary differences between the two types:
|
Irritant contact dermatitis
|
Allergic contact dermatitis
|
|
Often acute in onset
|
Acute, subacute, or chronic in onset
|
|
Appears after first exposure
|
Sensitization necessary before the reaction occurs
|
|
Decrescendo phenomenon - reaches a rapid peak and starts to resolve
|
Crescendo phenomenon - keeps worsening and resolves more slowly
|
|
Red swollen skin, sometimes ulcerated, in acute form
|
Vesicles are common, but ulceration or skin necrosis is rare in acute cases
|
|
Thickening, erosion, fissuring, or shiny skin following chronic irritation
|
Vesicles may not be found in chronic cases
|
|
Sharply delimited rash in area of contact
|
More ill-defined boundaries but lesions usually found in areas of contact
|
|
Burning or stinging of the area, which is intensely tender
|
Intensely pruritic lesions
|
Diagnosis and treatment
A careful history, with a physical examination, is supplemented with skin testing using the patch test if the reaction recurs frequently or persists for a long time. Treatment may vary from leaving the skin absolutely untreated, or washing it with copious amounts of water and avoiding further exposure to the offending substance, to corticosteroid therapy. Emollients are essential to lock in the skin oils and to keep the skin from scaling, helping the healing process. In most cases, the skin becomes clear within 3 weeks. Soap should not be used on affected areas.
Severe, persistent, or infected lesions may require systemic corticosteroids, antibiotics, or calcineurine inhibitors.
References
- https://medlineplus.gov/ency/article/000869.htm
- https://www.med.umich.edu/intmed/allergy/edu/syllabus/TOPICS/Contact%20Dermatitis/contactderm.htm
- https://www.ncbi.nlm.nih.gov/pubmed/1017189
- http://www.aafp.org/afp/2010/0801/p249.html
Further Reading
Last Updated: Feb 26, 2019