Laser in situ keratomileusis (LASIK) surgery is a safe and effective treatment for refractive errors, the most common of which include myopia, hyperopia, and astigmatism. Both a combination of technological advances and increasing surgical experience have resulted in improved refractive outcomes and reduced complication rates.
Although LASIK surgery is an effective and safe procedure for the right patient, the possibility of developing postoperative complications is always present. Still, a large number of intraoperative complications can potentially be prevented with the appropriate preoperative and intraoperative precautions, as well as the careful maintenance of surgical instruments.
LASIK Surgery and its Risks
Intraoperative complications
Flap-related complications are the most common intraoperative complications following LASIK surgery. An incomplete flap, which is reported in 3% of cases, can occur when the smooth passage of the microkeratome, which is a precise instrument with an oscillating blade, is obstructed within the surgical field. Other significant causes of flap-related complications include the intraoperative loss of suction, electrical failure, accidental release of the vacuum, and damage to the microkeratome.
Thin flaps and buttonholes can result from the application of inadequate suction, irregular corneas, and poor blade quality. Thin flaps are often cumbersome to manipulate, as they are more likely to wrinkle. Comparatively, a buttonhole flap is often detected after the reverse pass of the microkeratome. These complications can be reduced or avoided by proper preventive maintenance of the microkeratome.
Corneal perforation represents a devastating intraoperative complication that can occur during the creation of the flap. A poorly secured blade of microkeratome can perforate the cornea and cause subsequent damage to the underlying lens and iris; however, this type of complication has also been seen during laser ablation. Today, corneal perforation represents a rare event, as modern instruments tend to use fixed depth plates.
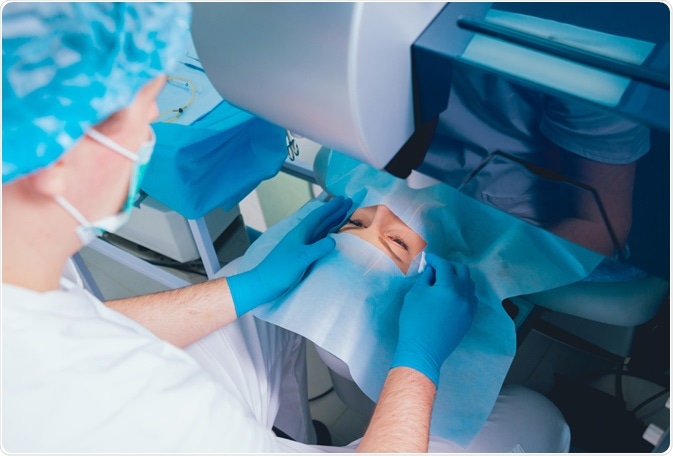
Image Credit: Roman Zaiets / Shutterstock.com
Early postoperative complications
During the first 24 hours after LASIK surgery, flap dislocation can occur as a result of mechanical disruption. Significant pain and severely reduced vision are common signs that this complication has occurred. In the event that flap dislocation has occurred, it should be repositioned as soon as possible in order to prevent the formation of fixed folds and/or epithelial ingrowth.
Flap striae after LASIK surgery can occur in up to 3.5% of patients and is, therefore, more common than full flap dislocations. This complication is a result of the misalignment of the flap and can be classified into macrostriae and microstriae. Gentle flap manipulation is shown to decrease the incidence of striae. additional treatments such as suturing are required for persistent striae.
Epithelial trauma at the time of surgery can lead to the proliferation of epithelial cells into the space between the stromal bed and the flap, which, in turn, may result in epithelial ingrowth. Important risk factors for this condition are peripheral epithelial defects, poor flap adhesion or its perforation, and free cap.
Albeit rare, infections are potentially vision-threatening early postoperative complications of LASIK surgery. Most of these infections are acquired intraoperatively, although some of them are caused by postoperative contamination. The incidence ranges from 0 to 1.5%, and they typically present within 72 hours after surgery. Common symptoms of these infections include increased light sensitivity, redness, pain, and loss of vision.
Late postoperative complications
The coordinated action of the cornea, conjunctiva, and accessory lacrimal glands in normal tear function is vital to the healthy functioning of the eye. Post-LASIK dry eye syndrome represents one of the most common late postoperative complications of this procedure. The main risk factors implicated in this complication are preoperative eye dryness and chronic ocular surface inflammation.
Chronic tear dysfunction is a subset of the post-LASIK dry eye syndrome and can be accompanied by neurotrophic keratopathy or neuropathic pain. This condition can range from asymptomatic or mild to severe and debilitating. Injury of the epithelium during refractive surgery alters the tear film cytokine levels. Moreover, LASIK surgery has also been associated with the loss of goblet cell mucin, which ultimately can lead to tear film instability.
Corneal ectasia is another rare, but serious complication of LASIK surgery which manifests as a progressive corneal thinning in the area of ectasia with unstable topographical steepening. This complication can arise even several years after the surgery and is linked to a reduction of unaided or spectacle-aided visual acuity. Collagen cross-linking is studied as a potential treatment of ectatic disorders and thus far shows significant promise.
Starbursts (glare), ghosting, haloes, and double vision are occasionally reported after LASIK surgery. These complications are often referred to as higher-order visual aberrations. Although these symptoms usually resolve in time, there is a risk that they may permanently affect the quality of vision.
References
Further Reading
Last Updated: Jan 18, 2023