In absolute terms, hypotension or low blood pressure can be defined as blood pressure lower than 80/50 mmHg.
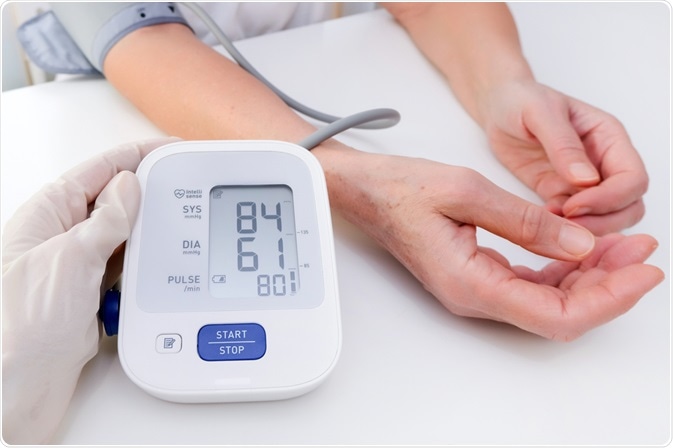
Image Credit: lev.studio / Shutterstock.com
The potential causes of hypotension range from dehydration to serious medical disorders. Moreover, the condition itself becomes clinically important when it is associated with symptoms. The diagnosis of hypotension is based on the medical history, a physical exam, and test results.
Classification of symptoms
Different forms of hypotension can be clinically classified into three groups based on their symptoms. These types of hypotension include asymptomatic chronic hypotension, chronic hypotension with multiple symptoms, and orthostatic dysregulation. In contrast to arterial hypertension, low blood pressure does not lead to cardiovascular damage.
Asymptomatic chronic hypotension is not considered a disease; therefore, treatment is not required. Rather, this form of hypotension is seen as a normal, constitutionally determined variant of circulatory regulation that is often observed in trained high-performance athletes when the resting circulation is in a parasympathetic state.
In chronically or occasionally decreased blood pressure, different subjective complaints can arise as a result of insufficient circulation to the organs, but also due to the unspecific disorders of the general condition. The cardinal symptom of this form of hypotension is dizziness or lightheadedness, which accounts for approximately 5 percent of primary care clinic visits.
Other symptoms include rapid tiring, lack of concentration, irritability, vertigo, nausea, sleep disorders, tinnitus (ringing in the ears), sensitivity to cold, lack of appetite, dyspnea, and painful sensations near the heart. It is often hard to differentiate these symptoms from psychovegetative disorders of a general condition.
In orthostatic hypotension or orthostatic dysregulation, changes in the person's position, particularly, when standing up, can decrease venous blood return to the heart, resulting in a sudden drop in blood pressure. Symptoms of orthostatic hypotension include feelings of vertigo, empty feeling in the head, insecurity in walking, collapse, and syncope. The condition is frequent in older people with disorders of the autonomic nervous system.
Diagnosis of hypotension
A diagnosis of hypotension is made when repeated blood pressure measurements show a decrease in blood pressure associated with symptoms and subjective complaints. The goal of additional diagnostic procedures is to find an underlying cause in order to determine any systemic problems and suggest the correct treatment.
The measurement of blood pressure and heart rate while supine for at least 5 minutes and then again after standing for 1 and 3 minutes is important in establishing a diagnosis of orthostatic hypotension. Measuring both seated and standing blood pressures represents an alternative in everyday clinical practice.
The tilt table test, which is also known as the head upright tilt test or passive head-up tilt test, records blood pressure and heart rate values on a minute-by-minute basis while the table is tilted in a head-up position at different levels. The test is important in the differential diagnosis of unexplained syncope and has proven pivotal in understanding the hemodynamic changes related to dysautonomia.
The Valsalva maneuver is another physical examination that can be used to assess autonomic function in hemodynamics by analyzing heart rate and blood pressure. For this test, parameters are measured after several cycles of deep breathing using a noninvasive blood pressure monitoring system.
Blood tests, which should include complete blood count (CBC), vitamin B12 levels, basic metabolic panel, and morning cortisol, as well as an electrocardiogram (ECG) and echocardiogram can provide additional information and sometimes aid in finding the principal cause of hypotension. Magnetic resonance imaging (MRI) can be employed to assess possible etiologies of neurogenic orthostatic hypotension.
References
Further Reading
Last Updated: Oct 28, 2022