A neurocutaneous syndrome is a general term for disorders that affect the brain, as well as the spine and peripheral nerves. These life-long conditions lead to the growth of tumors in the spinal cord, brain, bones, and skin.
The three most common forms of a neurocutaneous syndrome are neurofibromatosis, tuberous sclerosis, and Sturge-Weber syndrome. While all three of these diseases occur as congenital conditions, neurofibromatosis can also occur sporadically as the result of a gene mutation that develops later in life.
All neurocutaneous syndromes are incurable; therefore, treatment is aimed at prolonging survival and improving quality of life.
Prevalence
Estimates from the National Institute of Neurological Disorders (NINDS) suggest that in the United States, around one in 3,000 to 4,000 individuals are born with neurofibromatosis type 1, whereas around one in 25,000 are born with neurofibromatosis type 2. Tuberous sclerosis affects around 1 in 6,000 individuals and Sturge-Weber syndrome affects about one in 5,000 to 10,000.
Other neurocutaneous syndromes
Some examples of other neurocutaneous syndromes include:
- Ataxia-telangiectasia
- von Hippel-Lindau disease
- Klippel-Trenaunay-Weber Syndrome
- Osler-Weber-Rendu Syndrome
- Wyburn-Mason Syndrome
- Linear Sebacious Nevus Syndrome
- Neurocutaneous Melanosis
- Waardenburg Syndrome Type 1 & 2
- Fabry's Disease
Symptoms
The symptoms that manifest vary significantly between conditions and between individuals. In many cases, the effects are not evident at birth and only become apparent as a child grows and develops. As well as physical complications, there are also educational and social problems associated with these conditions that lead children to require support with throughout their lives.
Neurofibromatosis type 1
The primary symptom of neurofibromatosis type 1 is the presence of light brown patches on the skin, which are referred to as “café-au-lait” spots. Benign tumors referred to as neurofibromas also grow on the nerves and in various organs of the patient’s body, particularly the brain. Very rarely, in less than 1% of cases, affected individuals develop malignant neurofibromas.
Small tumors referred to as Lisch nodules may develop as the patient reaches adolescence; however, these tumors are relatively harmless and rarely cause problems. Other symptoms the person may develop include headaches, hearing loss, facial pain, seizures, numbness, and scoliosis. Intellectual disability, learning difficulties, and hyperactivity are also associated with the illness.
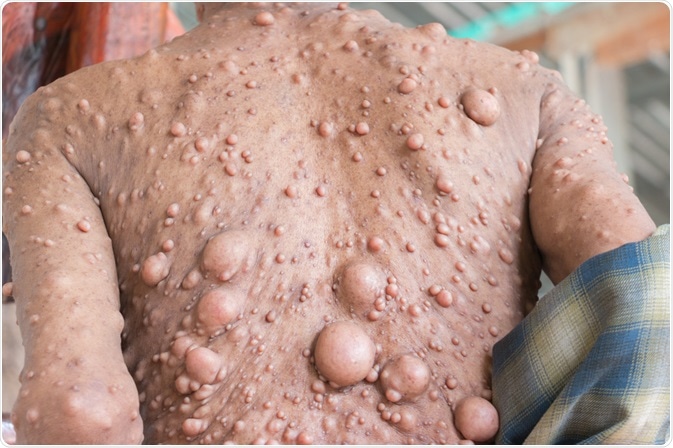
Image Credit: CHIEW / Shutterstock.com
Neurofibromatosis type 2
Also called bilateral acoustic neurofibromatosis, neurofibromatosis type 2 is characterized by tumors that grow on the eighth cranial nerve. The tumors lead to a loss of hearing, difficulty with facial movement, headaches, and problems with balance and mobility. Other signs associated with neurofibromatosis type 2 include neurofibromas, seizures, and café-au-lait spots, although these symptoms are much less common than in type 1 neurofibromatosis.
Tuberous Sclerosis
Tuberous sclerosis is characterized by the presence of growths referred to as tubers which develop inside the brain and the retina. The condition also affects many other parts of the body including the lungs, heart, kidneys, spinal cord, skeletal bones, and skin. Some of the problems associated with this disease include learning disabilities, intellectual disability, seizures, and developmental delays.
Sturge-Weber syndrome
The most common symptom of Sturge-Weber syndrome is a port-wine stain on the face when the child is born. This usually occurs as a flat, red, or purple mark across the forehead and around the eye area. This birthmark arises due to the presence of an excess of small blood vessels underneath the skin.
The child may also be born with glaucoma, a condition that causes pressure to build up in the eye. Sturge-Weber syndrome can cause symptoms such as visual disturbances, intellectual disability, seizures, and weakness in the muscles. Unlike neurofibromatosis and tuberous sclerosis, this condition does not affect other organs in the body.
Management
Neurocutaneous syndromes are lifelong conditions that cannot be cured. Therefore, treatment is aimed at managing symptoms, which often involves input from a multidisciplinary team of professionals.
Some of the health providers involved in managing a patient with a neurocutaneous syndrome include a pediatrician, ophthalmologist, neurologist, neurosurgeon, nurse, and rehabilitation experts such as occupational, physical, and speech therapists.
Management is typically focused on preventing or limiting the development of deformities and helping the patient to achieve independence at home and in the community.
References
Further Reading
Last Updated: Nov 8, 2022