Ocular larva migrans is a rare inflammatory condition of the eye caused by local reactions to the larva of Toxocara species. These are roundworms which infest dogs and cats as their definitive hosts. Toxocara canis (T. cani), which infests dogs, is more commonly implicated than Toxocara cati (T. cati) because dogs deposit their feces in a more indiscriminate manner.
Infestation with ocular larva migrans
Toxocara is a common nematodan parasite. The female worm produces hundreds of thousands of non-infective non-embryonated eggs while in the intestine of the host, where it survives for approximately 4-6 months. These eggs undergo two molts in the soil, where they are passed along with the animal’s feces. This takes 2-5 weeks, during which they mature into embryonated infective third-stage larvae under the right conditions of warmth, moisture and shade. When soil contaminated with these larvae is ingested, whether deliberately, as in children with pica, or accidentally, the eggs are swallowed and hatch in the intestine of the human host.
Accidental consumption of soil may follow the eating of fruits and vegetables that are grown in such soil or if it is used as compost. In addition, soil lodged on the hands may enter the food chain if hand-washing does not occur after working or playing outdoors or with animal hosts of the roundworm.
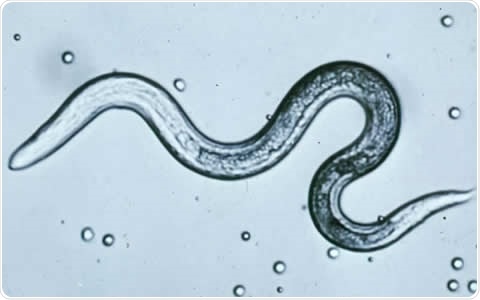 Toxocara canis (T. cani) larva - Image Credit:CDC
Toxocara canis (T. cani) larva - Image Credit:CDC
The hatched eggs produce second-stage larvae which cannot, however, mature in the accidental human host. Instead, they migrate through the intestinal wall to enter the blood capillaries and be carried to different parts of the body. When they reach the eye and settle in it, the condition is called ocular larva migrans. Only a small number of larvae are required to precipitate this eye disorder, and therefore the anti-Toxocara antibody level is lower or indiscernible, in contrast with visceral larva migrans.
Epidemiology
Ocular larva migrans is a disease caused by the final migration of these larvae and affects mostly the young, with an average age group of 3-11 years. Males and females are equally affected. Low socioeconomic groups have a disproportionately high prevalence.
Pathogenesis
In most cases, the larvae migrate into the posterior segment of one eye through the choroidal and retinal blood vessels. All ocular larval migration does not produce inflammation and retinal granulomas. Thus a sight-threatening response to the larvae depends also upon the release of the Toxocara excretory-secretory (TES) antigen and/or the host immune response. In cases where eye inflammation occurs, eventually visual loss occurs.
Other toxocariasis symptoms are typically absent. This leads to the suggestion that the worm load is so low that the body’s immune system does not react to kill the worm. Thus the larva has opportunity to reach the eye, even 10 years after initial infection. Ocular migration is a chance phenomenon.
Diagnosis
An eye examination, in response to the symptoms, most commonly shows the presence of granulomas, vitreous or chorioretinal inflammation, or scarring granulomas.
Blood tests for eosinophilia and an elevated white cell count are usually negative. Toxocara antibodies are negative as well, in some cases. Histopathologic examination of biopsy specimens may show the larvae. However, the diagnosis is purely one of presumed ocular LM in many cases as other tests remain negative.
Treatment
In the presence of ocular larva migrans, treatment is directed towards suppressing intraocular inflammation by glucocorticoid therapy. In addition, antihelminthic drugs such as diethylcarbamazine or albendazole should be given to eradicate the infection completely. Vitrectomy may be performed, if needed, to improve vision and remove granulomas.
References
Further Reading
Last Updated: Feb 27, 2019