Peptic ulcers are open sores along the inner lining of the stomach, duodenum, or esophagus.
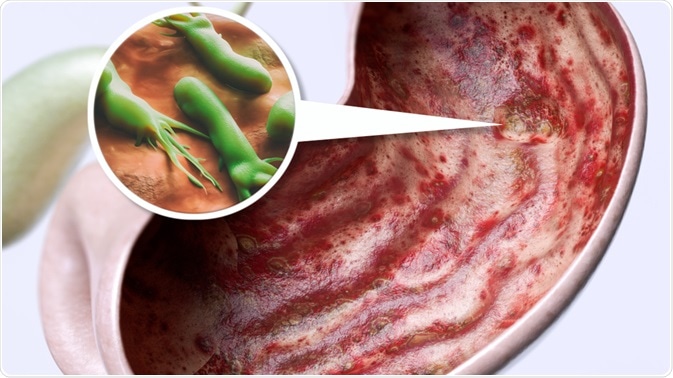
Image Credit: Crevis / Shutterstock.com
Introduction
The two primary causes of peptic ulcers are infection with Helicobacter pylori bacteria and the overuse of non-steroidal anti-inflammatory drugs (NSAIDs).
Most peptic ulcers are highly treatable. The method of treatment will depend on the underlying cause of the ulcer.
A clinician can often deduce the cause of an ulcer after performing a medical history and, if necessary, ordering tests for the presence of H. pylori. The information obtained in the diagnostic period will guide subsequent treatment decisions. Patients can be treated for peptic ulcers using a variety of medications and lifestyle changes.
Treatment for H. pylori ulcers
If the underlying cause of the peptic ulcer is infection with H. pylori, then treatment will focus on the eradication of the bacteria from the gastrointestinal (GI) tract. This can be achieved with a course of antibiotics.
Typically, a combination of two antibiotics is taken together twice a day for seven to fourteen days. The antibiotics commonly prescribed include amoxicillin, clarithromycin, and metronidazole. Unfortunately, many strains of H. pylori are becoming resistant to certain antibiotics, making eradication therapy more challenging.
The course of antibiotics is often combined with a proton pump inhibitor (PPI) medication and, together, this is called triple therapy. PPIs block the action of gastric secretory cells and reduce or eliminate levels of acid in the stomach and small intestine.
A similar line of medication called H2-receptor agonists block the action of histamine and cause a similar reduction in stomach acid. H2-receptor agonists are more often used when the ulcer is located in the duodenum. Both PPIs and H2-receptor agonists suppress gastric acid levels and allow the wound to heal.
Treating ulcers caused by NSAID overuse
If the underlying cause of the ulcer is the overuse of NSAIDs, a clinician will often recommend switching to different pain medication, if possible. Oftentimes, a patient will obtain a similar benefit from acetaminophen, which is not an NSAID and does not irritate the lining of the stomach. In addition, a patient with an NSAID-associated ulcer will also be prescribed a PPI or H2-receptor agonist medication in order to reduce acid levels and allow the ulcer to heal.
In addition, a clinician may also prescribe an over-the-counter antacid to neutralize existing stomach acids or a cytoprotective agent such as bismuth subsalicyclate to protect the lining of the GI tract. These agents generally alleviate patient discomfort but do not promote healing.
In cases of ulcers with severe bleeding, or if bleeding is observed by the clinician during an endoscopic exam, it may be necessary to cauterize the blood vessel or apply medication to stop the flow of blood. In very extreme cases where an ulcer has perforated the stomach or intestinal wall, emergency surgery may be necessary.
Lifestyle changes
There are a number of lifestyle changes a patient can make in order to alleviate symptoms of an ongoing ulcer and reduce the potential risk for future ulcers. These include avoiding behaviors that irritate the lining of the stomach such as smoking, consuming alcohol, or avoiding long-term use or high doses of NSAIDs for pain relief.
Patients should also try to appropriately manage stress in their daily lives, which can aggravate symptoms of an existing ulcer. Eating a healthy diet is also important so that the body can heal faster.
Refractory ulcers
In rare cases, an ulcer may fail to heal with standard therapy and is therefore referred to as a refractory ulcer. This may be because the H. pylori strain is resistant to first-line antibiotics or the sores are due to an infection with bacteria other than H. pylori.
Refractory ulcers can also be attributed to extreme acid production in the GI tract, stomach cancer, or a disease unrelated to ulcers such as Crohn’s disease.
References
Further Reading
Last Updated: Nov 2, 2022