Scleroderma, also sometimes referred to as systemic sclerosis, is a chronic autoimmune disorder that involves a progressive hardening of the skin. An excess of collagen and other connective tissues in the skin leads to a change in cellular structure and vascular of the tissues. Internal organs may also be affected in more severe cases.
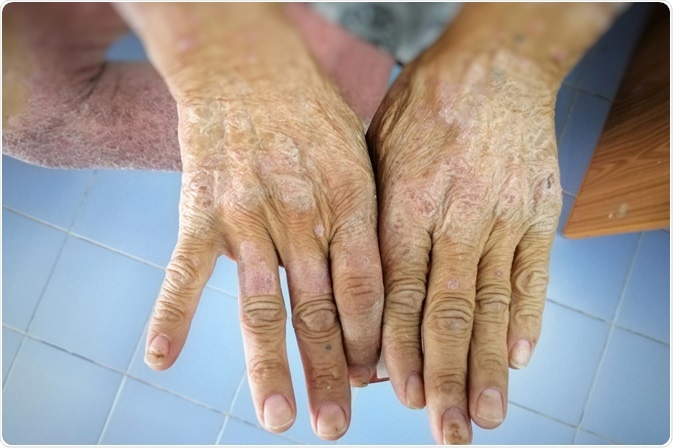
Image Credit: Numstocker / Shutterstock
The term derives from the Greek works skleros, which means hard or indurated, and derma, which means skin. Hippocrates was the first person recorded to reference the condition, describing the symptoms of thickened skin.
It usually presents in adults aged 20-50 years old, although any age group may be affected. Females are more likely to be affected, with four to nine times the risk of suffering from the disease in respect to the male counterpart.
Scleroderma affects populations throughout the world, although the exact incidence and prevalence of the disease varies among different ethnicities. Asian populations, for example, are less likely to have symptoms of scleroderma and it is more common in African America populations.
The incidence of the disease is 19 per million in the United States, and the overall prevalence of the country is 240 per million. In Australia, the incidence is 22.8 per million and the prevalence 233 per million.
Risk Factors and Causes
The cause of sclerosis is not currently known, although it appears there are a range of factors that may affect the likelihood of an individual of suffering from the disease. These include family history, environmental factors and previous medical therapies.
Scleroderma is not thought to be an inherited condition, although a genetic predisposition seems to be evident in some individuals with a family history of the condition.
There are certain environmental triggers that are associated with an increased risk of disease. These include exposure to silica, radiation and solvents such as vinyl chloride, trichloroethylene, epoxy resins, benzene and carbon tetrachloride.
Additionally, invasive treatments for in cancer patients, such as radiotherapy, may trigger scleroderma. Some evidence also indicates that some viral factors may accelerate the progression of disease.
Types
There are two main forms of scleroderma, which are:
- Limited cutaneous sclerosis: affecting the skin only, predominantly the hands, arms and face. Complications may include calcinosis, Raynaud’s phenomenon, esophageal dysfunction, sclerodactyly, telangiectasias and pulmonary hypertension. The prognosis of this type is usually positive, particularly for patients without pulmonary hypertension.
- Diffuse cutaneous sclerosis: widespread skin and the involvement of at least one internal organ (e.g. kidneys, esophagus, heart, lungs). May be considerably disabling and has a poorer prognosis, particularly for males and those that are elderly.
There are also some other types of the disease, such as fulminant sclerosis, which is distinguished by more severe involvement of the skin and other organs.
Diagnosis
If a patient present with symptoms indicative of scleroderma, there are several diagnostic methods that can be used to establish the involvement of the disease.
Initially, a thorough medical and family history should be taken. This is essential because there may be a genetic link in the development of the disease and some previous medical treatment (e.g. radiotherapy) may increase risk of scleroderma.
Additionally, some environmental factors are known to trigger the disease in some patients, such as exposure to silica, radiation and various solvents.
Treatment
There are currently no treatments for scleroderma, but the complications of the involvement of particular organ systems can be managed appropriately.
Particularly more severe forms of the disease with affected organ will require treatment to manage or reduce the risk of complications.
References
Further Reading
Last Updated: Mar 11, 2021