A colorectal polyp is a growth that may present on the lining of the colon or rectum. While these are fairly common and affect between 15-20% of the adult population, they are not usually associated with symptoms. However, large polyps can cause bowel obstructions that may lead to symptoms such as nausea, vomiting, and severe constipation.
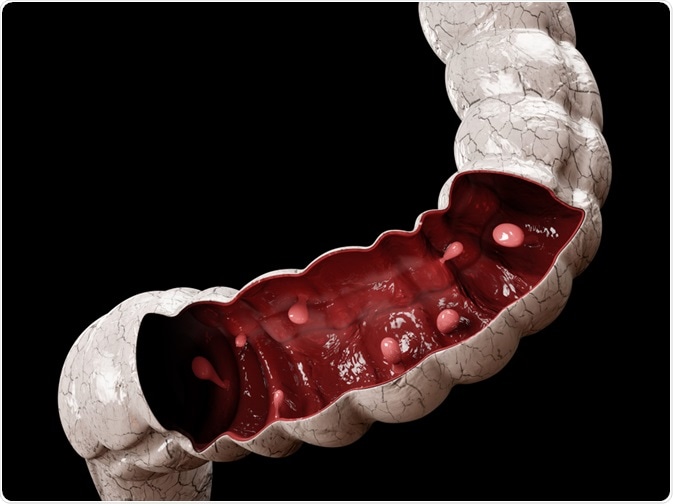
Image Credit: Victor Josan / Shutterstock.com
The best course of action when a polyp is found is dependent upon the number, type, size, and location of the polyp. While bowel polyps are not usually cancerous, they will need to be removed completely and safely as soon as possible, as some polyps have the potential to progress to cancer if left untreated.
Classifying polyps
Polyps can be classified as either pedunculated or sessile. Whereas pedunculated polyps are attached to the intestinal wall by a stalk, sessile polyps grow directly from the wall. In addition to these classifications, polyps can also be separated into three distinct categories:
- Adenomatous (malignant)
- Hamartomatous
- Inflammatory
Colorectal Polyps, Causes, Signs and Symptoms, Diagnosis and Treatment.
Adenomatous (malignant) polyp
Adenomatous (malignant) polyps are of the greatest concern as they have the potential to become cancerous after many years. Such adenomas are histologically classified as tubular, tubulovillous, or villous, each of which exhibit distinct growth patterns. Of these adenomas, the two that are of the greatest concern include tubular and villous adenomas, with a mixture of these growth patterns giving a tubulovillous adenoma.
Generally, most small adenomas (< 1/2 inch) have a tubular growth pattern, whereas the larger ones may have a villous growth pattern and, therefore, an increased likelihood of becoming cancerous.
The likelihood of cancer in an adenomatous polyp at the time of discovery is related to its histologic type, size, and degree of dysplasia. For example, a tubular adenoma that is 1.5 centimeters (cm) in size has a 2% risk of being cancerous compared to a 35% risk in a 3 cm villous adenoma. A somewhat more aggressive type of adenoma known as a serrated adenoma may develop from hyperplastic polyps.
Following the removal of an adenoma, patients will require a follow-up examination, as new polyps may develop over time that will also need to be removed.
Hamartomatous polyp
A hamartoma is defined as a tumor-like malformation that presents due to an error in the development at numerous sites where growth occurs. These lesions are benign and may not cause any problems, usually identified incidentally, as they tend to grow at the normal and non-pathological rate of the host tissue, rarely causing problems such as compression.
Despite these characteristics, hamartomas are not harmless. Morbidity can arise by means of a variety of mechanisms such as obstruction, infection, infarction, hemorrhage, and iron deficiency anemia amongst others.
While hamartomas may resemble a neoplasm, this type of tumor does not usually show a tendency to evolve into one. With this being said, the occurrences of neoplastic evolution have been reported in patients suffering from von Recklinghausen disease. Interestingly, an association has also been established between neoplasms and hamartomas which can be seen in some patients with Peutz-Jeghers syndrome. While the polyps themselves carry a small potential for malignancy, there is still a 15% chance of colonic malignancy because of potential coexisting adenomas.
Inflammatory polyp
Inflammatory polyps are associated with inflammatory conditions such as Crohn’s disease and ulcerative colitis (UC). Although the polyps themselves are not a particularly significant threat, suffering from these two colon disorders increases the overall risk of colon cancer.
Risk factors for colorectal cancer
It is possible for anyone to get colorectal cancer; however, this type of cancer is most commonly reported in people over age 50.
Risk factors for colorectal cancer include:
- A history (personal or family) of colorectal cancer or polyps
- Unhealthy diet (abundant in red and processed meats)
- Inflammatory bowel disease (such as Crohn's disease or UC)
- Inherited conditions (including hereditary non-polyposis colon cancer and familial adenomatous polyposis)
- Obesity
- Smoking
- Sedentary lifestyle
- Alcohol abuse
- Type 2 diabetes
References
Further Reading
Last Updated: May 9, 2021