Dysphagia is the term used to describe difficulty swallowing. The term can be broken down into two parts, where “dys” meaning difficulty and “phag” meaning eating.
For some people affected by the condition, the difficulty swallowing may be restricted to food only, while others may also have difficulty with liquids and some people are unable to swallow altogether.
Typical symptoms of this condition include coughing or choking when eating or drinking, a sensation of food being lodged in the throat or chest, and a tendency to regurgitate food. Dysphagia often makes eating challenging, meaning the affected individual has difficulty taking in sufficient calories and nutrients. Eventually, dysphagia may lead to weight loss, recurring chest infections, and other serious complications.
Causes
Although dysphagia can affect anyone, it is more likely to affect babies, older adults, or people with a brain or nervous system disorder. The condition usually arises due to a problem in the throat, which is referred to as oropharyngeal dysphagia, or esophagus, otherwise known as esophageal dysphagia.
In cases of oropharyngeal dysphagia, material from the oropharynx is not properly emptied into the esophagus. These patients report difficulty swallowing, nasal regurgitation, and breathing in food, which causes coughing. This form of dysphagia usually occurs in people who have a nervous system disorder or a condition that affects the skeletal muscles.
Esophageal dysphagia describes the difficulty in moving food down the esophagus, usually due to an obstruction of some type or a motility disorder.
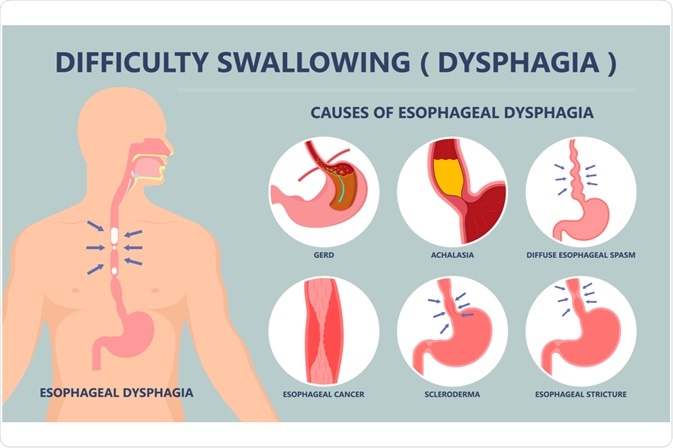
Image Credit: rumruay / Shutterstock.com
Additional examples of conditions that can prevent the muscles and nerves from working well enough to pass food through the throat and esophagus include:
- Stroke
- Brain or spine injury
- Nervous system disorders
- Multiple sclerosis
- Post-polio syndrome
- Parkinson’s disease
- Muscular dystrophy
- Inflammation disorders
- Polymyositis
- Dermatomyositis
- Scleroderma, which causes the tissue of the esophagus to harden and narrow
- Esophageal spasm, which is a sudden squeezing of the muscles in the esophagus that prevents food from passing through to the stomach
Examples of conditions that may cause an obstruction in the esophagus include:
- Gastroesophageal reflux disease (GERD), where stomach acid moves up into the esophagus causing ulcers to form and eventually scar tissue that narrows the structure.
- Esophagitis refers to inflammation in the esophagus that can be caused by infection, allergic reactions, or GERD.
- Esophageal tumors, which may be benign or malignant.
- Diverticula, which are small sacs that form in the wall of the throat or esophagus.
- Masses may form outside of the esophagus that press on the structure and narrow it.
Diagnosis
Dysphagia is diagnosed based on symptoms and physical examinations. A doctor may also want to check the patient’s muscle strength, speech, and reflexes. The patient may then be referred to another specialist, which can include:
- An otolaryngologist who deals with problems occurring in the ear, nose, and throat
- A neurologist who manages problems with the brain, spine, and nervous system
- A gastroenterologist who is an expert in the digestive system
- A speech-language therapist
In order to establish the exact cause of a patient’s dysphagia, a consultant may arrange for one or more of the following tests:
- X-ray to generate images of the chest and neck
- Barium swallow test, which is an examination of the throat and esophagus. The patient swallows barium, which is a chalky liquid that coats the inside of the esophagus so that it can be highlighted on X-ray.
- Fluoroscopy, where a certain type of barium is used that enables videotaping of the swallowing process.
- Esophagoscopy, which uses a thin tube called an endoscope that is passed down the throat to examine the esophagus, as well as the stomach and duodenum. During this procedure, a biopsy, which is a tissue sample, is sometimes also taken for analysis.
- Laryngoscopy, where a mirror or endoscope is used to examine the back of the throat
- pH monitoring, which is used to find out how regularly stomach acid is getting into the esophagus, as well as how long it is staying there.
- Manometry, where an endoscope attached to a computer is placed in the esophagus to measure the pressure as a patient swallows.
Treatment
The treatment approach to dysphagia depends on the underlying cause of the condition and the type of dysphagia the patient is suffering from. The various different aspects to treatment can include speech and language therapy, placement of a feeding tube, surgery to open up any narrowing of the esophagus or remove an obstruction, adjusting the consistency of food so that it can be swallowed more safely and easily, as well as performing exercises to help train the muscles involved in swallowing to work properly.
People can also learn how to position their bodies in such a way that may make swallowing easier. With treatment, many cases of dysphagia improve, although a cure is not always achieved.
References
Further Reading
Last Updated: Jan 13, 2023