Blue nevi are a category of melanocytic tumors, which arise from the proliferation of dermal dendritic melanocytes to form an acquired pigmented mole. They are also called pigmented nevi, nevomelanocytic nevi of acquired origin, or melanocytic nevi.
These are typically innocuous tumors. The melanocytes are deep in the skin, unless with the brown or black moles. Dermoscopy shows an unchanging steel-blue pattern.
The most frequently observed variants include the common blue nevi and cellular blue nevi. A third of all oral nevi are blue nevi, and these occur most often on the scalp, the dorsal sides of the hands or feet, and the sacral area. Among these, the sacral area shows cellular blue nevi most frequently. The extremities are more likely to have common blue nevi.
They are present in about three percent of Japanese people, and their prevalence is usually higher in Asians; however, they also occur in 0.5-4 percent of Caucasians. Women are twice as often affected as men.
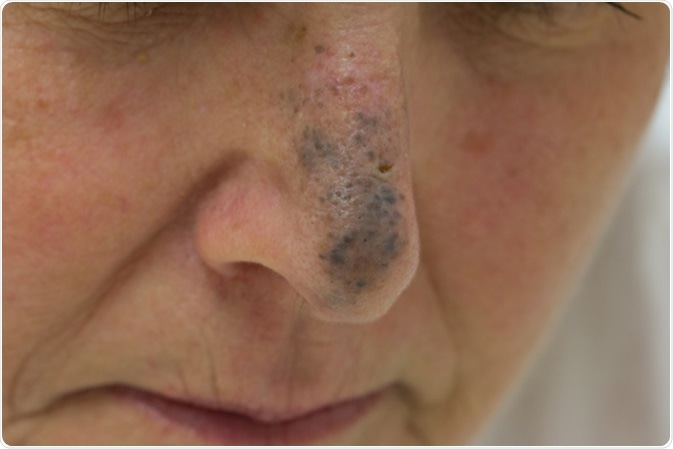
Blue Nevus on the Nose of a Female - Image Credit: Anthony Ricci / Shutterstock
Origin
Blue nevi arise from active dermal melanocytes present at birth, which occurs in these sites. In most other sites, these cells disappear from the dermis during fetal life. Common blue nevi contain spindled dendritic melanocytes, while cellular blue nevi show ovoid melanocytes. Junctional cells are rarely present.
Genetics of Blue Nevi
Most acquired melanocytic nevi have somatic activating mutations in MAPK signaling pathway genes, especially BRAF and NRAS genes. These are uncommonly found in blue nevi, which supports their independent origin, together with their clinical and histopathological features. However, blue nevi do exhibit somatic mutations of one of the genes which code for the G protein α-subunits, namely, GNAQ or GNA11 genes, mostly in codon 209.
These lead to a loss of GTPase activity and upregulates the MAPK pathway signaling. This is the same effect as occurs with BRAF and NRAS mutations. These mutations are oncogenic but their effect is not sufficient in isolation to cause cancerous changes, which correlates with the low risk of malignancy with blue nevi. Tumors which become malignant show a rapid increase in size.
Common Blue Nevi
These may occur in any age group, or even be present at birth. The most common age of occurrence is in adolescence. They are usually small smooth single papules colored dark blue to black. They are usually less than one centimeter in size. The color is due to the reflection of blue light, which has a shorter wavelength than light of other colors – the Tyndall scattering.
Cellular Blue Nevi
These may also be seen at any age. However, they usually arise below the age of 40 years. They are dark-colored, being bluish-black, and appear as plaques or nodules. They may be from one to several centimeters in size. Some larger cellular blue nevi on the trunk may appear histologically identical to a melanoma, but metastatic spread almost never occurs. FISH analysis is sometimes useful in distinguishing between such tumors and melanomas.
Other Variants
Rare variants and related dermal melanocytic proliferations have not been well studied, but the characteristic mutations are much less frequent in these than with the more common subtypes.
Diagnosis and Management
Blue nevi are diagnosed by their peculiar color, but if any suspicion of melanoma exists, the lesion is excised and sent for histopathological examination.
Blue nevi may be ignored if they are of typical size and appearance, and have a normal rate of growth. However, in most cases excision biopsy would be preferred to rule out more deadly conditions such as melanomas.
Excision under local anesthesia is preferred If the nevi have recently appeared or are fast growing, or if a melanoma or other skin cancer is to be ruled out based on the clinical appearance, or if they are very unsightly. Recurrence is uncommon but satellite lesions do occasionally occur following excision, and must be evaluated by biopsy to rule out malignant transformation.
References
Further Reading
Last Updated: Feb 26, 2019