Leptin is a peptide hormone produced by adipocytes. It is a key part of the regulatory mechanism for appetite and energy stores, acting via central and peripheral actions. This hormone shows effects on metabolism, endocrine system, immunity and energy balance.
The main function of leptin is to regulate the amount of body fat by central inhibition of appetite and food intake. Its effects on adipogenesis and energy expenditure are mediated via the hypothalamus, which is responsible for feelings of satiety. High leptin levels are correlated with body mass index (BMI), as well as body fat percentage.
Leptin is a cytokine of the long-chain helical cytokine family, containing interleukin-6, granulocyte colony-stimulating factor and growth hormone. It is coded for by the obese (OB or LEP) gene which is on chromosome 7q31.3, and which comprises three exons and two introns.
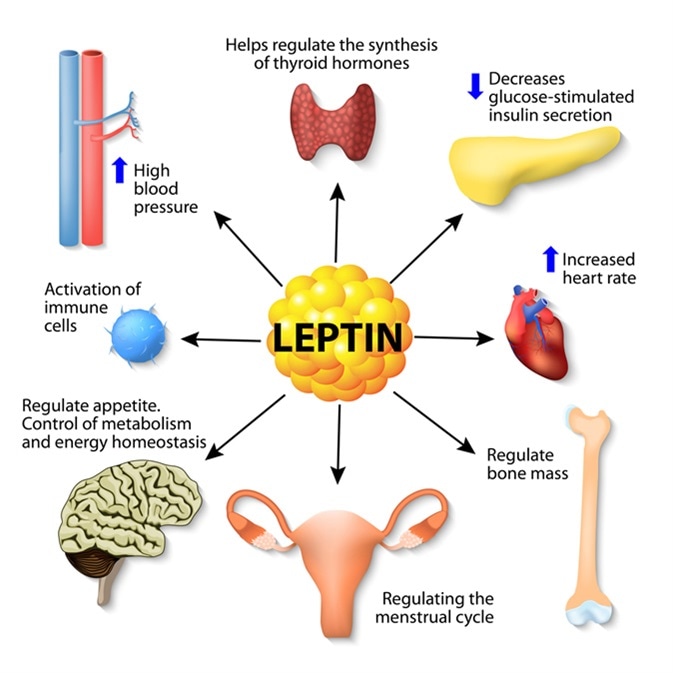
Image Credit: Designua / Shutterstock - Leptin is a hormone made by adipose cells that helps regulate appetite, control of metabolism, energy homeostasis, activation of immune cells, and other function.
Leptin Mutations
Leptin effects are through the leptin receptor which is part of the cytokine receptor family. Mutations in the genes that code for leptin or for the receptor can cause morbid obesity early in life, as was shown in rodents.
The other signs of homozygous mutations of this sort in rodents include:
- Hyperphagia (i.e. excessive eating)
- Lower energy expenditure
- High cortisol levels
- Abnormal glucose and lipid metabolism
- Infertility of the hypogonadotropic type
Leptin mutations in humans can also cause leptinopenia and early-onset obesity. It also causes:
- Reduced growth hormone and thyroid-Stimulating Hormone (TSH) levels
- Hyperinsulinemia with insulin resistance
- Dyslipidemia
- Severe degrees of hepatic steatosis
- Absence of secondary sexual development with hypogonadotropic hypogonadism
- Occasionally, immune deficiency resulting in severe and repeated bacterial infections that may be fatal early in life
There are eight different homozygous leptin gene mutations which can lead to leptinopenia. Mutations in the leptin gene leading to congenital leptin deficiency are most often seen in offspring of consanguineous marriages.
Leptin gene mutations are now treated by administration of the recombinant form of human leptin, metreleptin, in subcutaneous form. This is followed by weight loss, normalization or significant reduction in body fat, as well as of other systemic disturbances.
Gene sequencing is recommended at present only in cases of very severe obesity in childhood, especially if leptin levels are very low. It is possible that leptin mutations might occur which alter its biological activity, but not its synthesis or secretion, leaving the leptin levels unchanged. Thus new recommendations may be necessary to pick up such mutations due to the possibility of offering treatment.
Leptin Receptor Mutations
Leptin receptor mutations can also occur in the LEPR gene. The leptin receptor is found on many cells (including the hypothalamus) and mediates leptin actions in fat-energy balance, sleep, thirst, and body temperature - especially in relation to the body’s Circadian rhythms. It also affects endocrine function by regulating the secretion of many hormones.
The leptin receptor is activated by leptin binding, which occurs when fat cells become larger, indicating adequate or excessive body fat stores. This binding signals to the brain that there is no need to eat, which triggers the feeling of satiety.
Leptin receptor deficiency occurs as a result of receptor mutations, and this produces clinical signs of leptinopenia. LEPR mutations are inherited via autosomal recessive inheritance, so that the parents may not show any sign of the disorder but act as carriers, while the offspring may show the clinical spectrum of this condition.
References
Further Reading
Last Updated: Feb 26, 2019