Microcephaly is a condition in which a newborn baby has a much smaller head circumference than expected for the average infant at the same stage of development. Sometimes a child is born with no sign of microcephaly but develops symptoms later on due to other external factors. In order to take necessary steps to find out what is causing the condition and perhaps prevent it from getting any worse, timely diagnosis is very crucial.
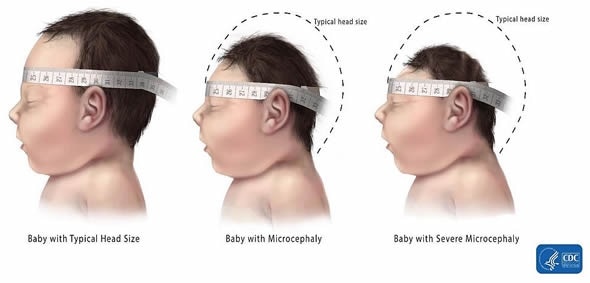
Image Credit: Centers for Disease Control and Prevention, National Center on Birth Defects and Developmental Disabilities)
Children with microcephaly usually have brain development issues which can result in hindered intelligence and physical challenges for the child. However, not all children born with microcephaly experience these additional complications. The condition can have a severe impact on the growing child leading to learning difficulties, speech issues, mobility issues due to challenges in using their arms and legs, and shortened stature. The patients also runs the risk of a reduced lifespan.
There are several ways by which doctors can identify microcephaly in an infant. Here are a few which cover diagnosis during pregnancy and afterwards:
Ultrasound
Microcephaly can be detected in the womb using an ultrasound scan, a technique that combines both high frequency sound waves and computer technology to produce diagnostic images of the growing baby’s blood vessels, organs, and tissues. However, microcephaly is not usually visible with this technique until the third trimester. The doctor usually looks for evidence of an abnormally small head in the ultrasound images.
Physical measurement of head circumference
Once the child is born, the medical staff can physically measure the circumference of the head. If there is evidence of a smaller size, the medical team may investigate further about the background of the parents to find out if microcephaly runs in the family. The team may also measure the parents’ heads to see if a smaller-sized head is just normal for either one of them. The head size of the baby is continuously monitored to see if it grows to become a size that is normally expected. However, the size of head in children affected by microcephaly differs across nations. Head size measurements take into account the sex, race, and age of the infant.
X-rays
X-rays can also be used as a diagnostic tool to confirm microcephaly. X-ray is not recommended for use during pregnancy as it is a form of radiation. Electromagnetic rays help the doctor view what is happening inside the child’s body and whether there are any abnormalities in the brain.
Computed tomography (CT or CAT)
This technology employs X-rays along with a computer to create more detailed horizontal or axial 3D slices of a body part. This is useful for revealing information about the organs, bones, muscles, and fat. CT scans are particularly good for studying bone injuries. CT scans are not advised during pregnancy.
Magnetic Resonance Imaging (MRI)
MRI uses large magnets to help create images of the body. This is best for viewing soft tissues such as in brain tumors, ligament and muscle injuries, and spinal cord injuries. MRI can be safely used on both pregnant women and babies.
Blood and Urine tests
Blood and urine tests are a good way of further determining any other health issues such as infections in the child. Medical teams also investigate genetic links to the development of microcephaly.
References
Further Reading
Last Updated: Dec 30, 2022