Introduction
Immune System and Psoriasis
Genetic Susceptibility to Psoriasis
Environmental Triggers for Psoriasis
HIV and Psoriasis
Medications for Psoriasis
References
The exact cause of psoriasis is not well understood, but it is generally accepted that several factors may contribute to an individual’s susceptibility to the condition and trigger symptoms. It is not a communicable condition and cannot be passed on from an infected patient to another person.
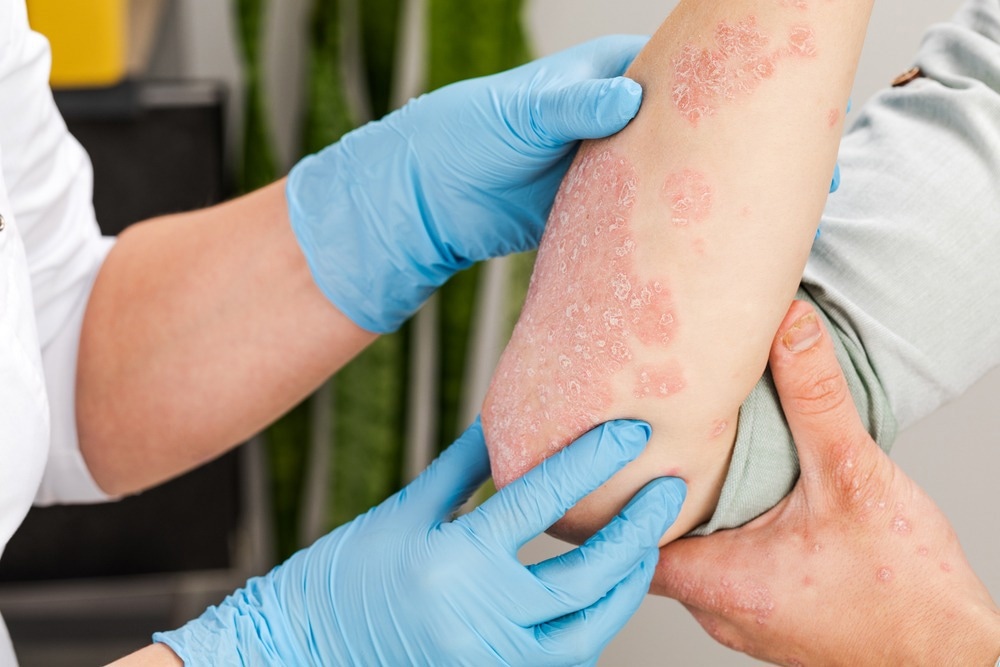
Image Credit: Fuss Sergey/Shutterstock.com
Immune System and Psoriasis
An abnormality in the immune system is thought to be the primary reason for the symptoms of psoriasis. The T-cells are usually responsible for detecting and destroying bacteria and other infections in the body but direct their action towards the healthy skin cells in patients with psoriasis.
This leads to the overproduction of new skin cells in the deep skin layers, triggering the release of more T-cells and continuing the cycle, eventually leading to psoriatic symptoms. The cause of this effect is thought to be a result of a combination of genetic susceptibility and environmental triggers.
Genetic Susceptibility to Psoriasis
Approximately 1 in 3 patients with psoriasis have a family history of the condition; if one identical twin is affected, the other has a 70% chance of developing the condition. These findings suggest a genetic link to the pathogenesis of psoriasis, and genetic loci associated with the condition have been identified.
Many genes are thought to be involved in the genetic susceptibility to psoriasis, many of which play a role in the immune system, specifically the major histocompatibility complex (MHC) and T cells. The most common genetic determinant of the condition is PSORS1, which is responsible for up to half of all genetically inherited cases.
Gene mutations that notably affect the immune system, such as IL12B and IL23R, are also being investigated for their role in causing psoriasis.
Environmental Triggers for Psoriasis
Certain triggers for psoriasis are known to induce or worsen symptoms of the condition following exposure. These triggers may include:
- Injury to the skin (e.g., cut, insect bite, sunburn)
- Excessive alcohol consumption
- Smoking
- Stress
- Hormonal changes at puberty or menopause
- Sickness (e.g., streptococcal throat infection)
- Seasonal or climate changes
- Dry skin
- Obesity
People with psoriasis should be encouraged to reduce their exposure to these triggers to help improve their symptoms and avoid a flare-up of the condition.
Image Credit: RAJ CREATIONZS/Shutterstock.com
HIV and Psoriasis
Individuals with HIV are equally likely to suffer from psoriasis than members of the general population, but those who are often affected experience more severe symptoms.
For this reason, there is a considerably higher incidence of psoriatic arthritis among patients with psoriasis that are HIV-positive compared to other patients. The overall symptoms tend to be more severe, and many patients require treatments beyond the standard therapy used for psoriasis.
Medications for Psoriasis
Some medications may trigger symptoms of psoriasis in some patients, such as:
- ACE inhibitors
- Antimalarial medicine
- Beta-blockers
- Calcium channel blockers
- Interleukins
- Interferons
- Lithium
- Non-steroidal anti-inflammatory drugs
- Terbinafine
- TNF inhibitors (e.g., infliximab or adalimumab)
Additionally, the withdrawal of topical corticosteroid cream may aggravate symptoms due to a rebound effect.
References:
- nhs.uk. (2018). Psoriasis - Causes. [online] Available at: https://www.nhs.uk/conditions/psoriasis/causes/.
- www.psoriasis.org. (n.d.). Psoriasis Causes & Triggers. [online] Available at: https://www.psoriasis.org/causes/.
- Mayo Clinic (2018). Psoriasis - Symptoms and causes. [online] Mayo Clinic. Available at: https://www.mayoclinic.org/diseases-conditions/psoriasis/symptoms-causes/syc-20355840.
- Healthline. (2018). Psoriasis Causes, Triggers, and Prevention. [online] Available at: https://www.healthline.com/health/psoriasis/causes#2 [Accessed 1 Aug. 2022].
Further Reading
Last Updated: Sep 11, 2023