Psoriasis represents a chronic inflammatory skin condition with a complex pathophysiology and significant genetic background. This disease is characterized by erythematous, scaling lesions that exhibit variable patterns and distribution, as well as different clinical phenotypes. Psoriasis can significantly influence the quality of life and usually requires lifetime control.
What Is Psoriasis?
Although Hippocrates described scaling diseases of the skin under the heading ‘lopoi,’ the first clinical description of psoriasis is attributed to Aurelius Celsus who mentioned this disease in his work De re medica. Still, the term ‘psoriasis’ was first used by a well-known Greek physician Galen, who derived it from the Greek word ‘psora’ which means itch.
According to recent estimates, psoriasis affects 2-3% of the world’s population, which is approximately 125 million people. Despite these staggering numbers, the incidence rate of psoriasis remains low, with a rate of roughly 92.3 new cases per 100,000 people per year worldwide.
Pathogenesis of the disease
A complex interplay between genetic factors and immunology culminates in the specific clinical and histological features of psoriasis. In predisposed individuals, thus-far unknown antigens trigger an insidious, self-perpetuating cycle of inflammation and subsequent epidermal hyperproliferation. Constituents of both innate and adaptive immune systems instigate and coordinate this process.
The time required for psoriatic epidermal cells to travel from the basal cell layer to the surface to be cast-off is 3-4 days, compared to a normal period of 26-28 days. The exact mechanism underlying this rapid increase in epidermal transit time is still a matter of debate, although it is often attributed to a shortened cell cycle time or recruitment of the resting cells in the active cycle.
A release of signaling proteins or cytokines stimulates an assembly of inflammatory gene products within the keratinocytes, inviting more immune cells into the skin and perpetuating the inflammatory milieu even more. This often results in unspecific histology of psoriasis, which can mimic a plethora of other dermatoses, as well as fungal infections.
Clinical and diagnostic features
Psoriasis is characterized by well-circumscribed, sharply demarcated erythematous papules and plaques. These papules and plaques are covered with brittle, dry, silvery, or greyish white and loosely adherent scales. Occasionally, a white blanching ring can be seen around psoriatic lesions, which is also known as Woronoff’s ring. The most commonly affected locations are the elbows, knees, umbilicus, scalp, and lumbar area.
Chronic plaque psoriasis represents the main type of psoriasis and is found in approximately 90% of cases. Other characteristic forms comprise erythrodermic psoriasis, guttate psoriasis, palmoplantar psoriasis, inverse psoriasis, and both localized and generalized pustular psoriasis. Psoriatic arthritis is a special type of arthritis associated with psoriatic skin lesions that involve peripheral and sacroiliac joints, the axial skeleton, entheses, and nails.
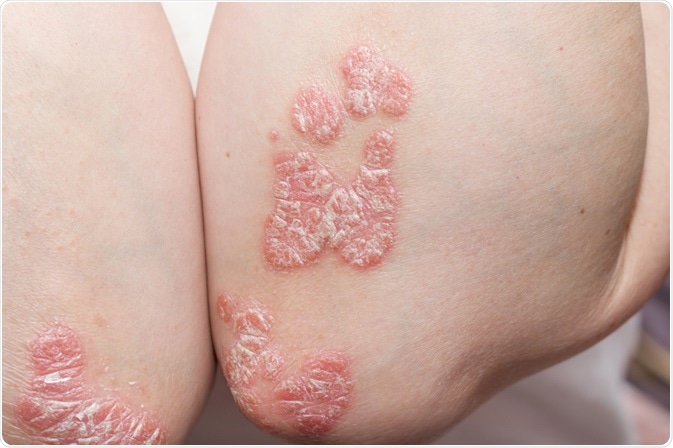
Image Credit: Millana / Shutterstock.com
Two phenomena are described which are highly specific for psoriasis. Removal of scales leads to pinpoint hemorrhages throughout the lesions, which is known as the Auspitz sign and corresponds to damage of dilated vessels in the superficial dermis. On the other hand, the Koebner phenomenon represents the development of skin lesions in areas of trauma.
Treatment options
There is a wide variety of different treatment options available for psoriasis; therefore, it is integral for patients and physicians to work together in building the appropriate approach. As patient adherence to treatment can influence the efficiency of a particular therapy, every patient should be involved in decision-making from the start. The specific treatment varies according to the location, severity, clinical variants, and duration of the disease.
Topical agents such as vitamin D analogs, corticosteroids, tacrolimus, pimecrolimus, tazarotene, anthralin, coal tar, and salicylic acid have all demonstrated efficacy in the treatment of psoriasis. Special attention should be given to the duration and dose of topical corticosteroids due to the risk of local and systemic side effects.
The most cost-effective approach for the extensive generalized disease is ultraviolet (UV) phototherapy. Systemic agents that include methotrexate, acitretin, and cyclosporine can also be used in such cases, whereas biologic agents such as infliximab, adalimumab, alefacept, and etanercept hold promise for the management of refractive disease.
References
- http://www.aafp.org/afp/2013/0501/p626.html
- http://www.nejm.org/doi/full/10.1056/NEJMra041320
- http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0068977/
- https://www.emjreviews.com/
- Menter A, Stoff B. Psoriasis. Manson Publishing Ltd, 2010; pp. 7-56.
- Pugashetti R, De Luca J, Feldman SR. Treatment of Psoriasis. In: Maibach H, Gorouhi F, editors. Evidence Based Dermatology, Second Edition. People's Medical Publishing House (USA), Shelton, Connecticut, 2011; pp. 213-234.
Further Reading
Last Updated: Dec 21, 2022