The diagnosis of sarcoidosis can be difficult due to the variable presentation of patients and the varied location of the causative nodules.
In most cases, diagnosis is made based on a comprehensive medical and family history, followed by a physical examination and various tests. As there are some other health conditions with similar symptoms, a differential diagnosis to confirm it is sarcoidosis is often necessary.
 The lungs and the lymph nodes are the most common placces for nodules to form in sarcoidosis. Image Credit: Magic mine / Shutterstock.com
The lungs and the lymph nodes are the most common placces for nodules to form in sarcoidosis. Image Credit: Magic mine / Shutterstock.com
Medical and family history
As the condition is likely to be linked to genetic factors that can be inherited, it is essential to establish if there is a family history of sarcoidosis. In addition to this, specific factors about the lifestyle of the individual may increase their risk of the condition. These include:
- Occupational factors that may have led to exposure to triggers
- Inhalation of beryllium metal (used in aircraft and weapons) throughout lifespan.
- Exposure to dust from birds or hay that may lead to inflammation
This information is important to determine the cause of the symptoms. Both beryllium metal and dust can cause inflammation in the lungs and symptoms similar to that of sarcoidosis, but are indicative of other health conditions in reality.
Physical examination
Following the medical history, a physical examination is required to check for evidence of nodules. Any evident lesions should be examined directly and signs of sarcoidosis should be sought, such as:
- Shortness of breath
- Red bumps on skin
- Swollen lymph nodes
- Enlarged liver or spleen
- Red eyes
- Abnormal or slow heartbeat
X-Ray imaging
A chest X-ray can be very useful to visualize the heart and the lungs and any nodules granulomas that may be affecting these organs. It can also help to detect enlarged lymph nodes.
As the vast majority of patients with sarcoidosis (more than 90%) have abnormal chest X-rays, this test is particularly useful in the diagnosis of the condition.
Biopsy
When sarcoidosis is suspected, the diagnosis should be confirmed by way of a biopsy. This involves the collection of a small tissue sample from an affected organ. Depending on the individual patient, the location of the biopsy tissue can vary, although it is most often from the skin or lymph nodes.
For a lung biopsy, a bronchoscopy utilizes a thin tube with a camera is threaded down the throat and into the respiratory organs. A small tissue sample can then also be taken with the same instrument for testing, known as a biopsy.
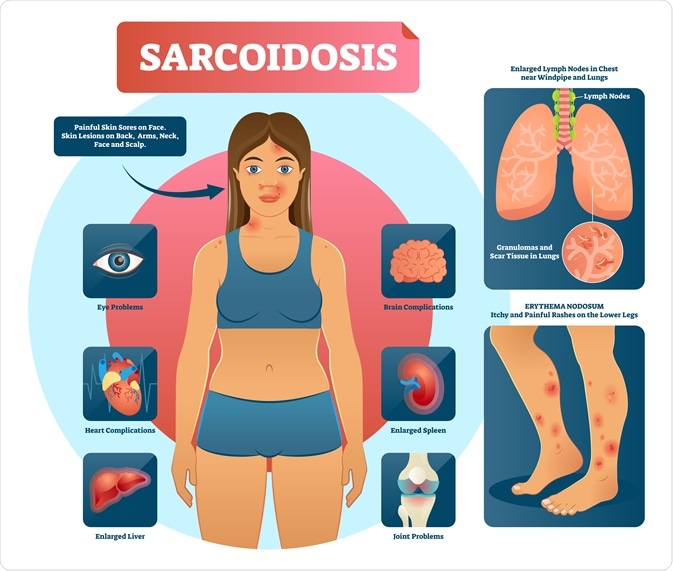 Infographic of sarcoidosis. Image Credit: VectorMine / Shutterstock.com
Infographic of sarcoidosis. Image Credit: VectorMine / Shutterstock.com
Other tests
There are several other tests that may then be called for to further categorize the condition and determine which organs are most affected. These tests are particularly beneficial in understanding the extent of the nodule growth and the appropriate management plan.
- Lung function tests – to measure the rate, volume and efficiency of breathing and ability to deliver oxygen to the circulation system
- Blood tests – to assess general health, as well as kidney and liver function
- Electrocardiogram – to investigate abnormal activity or size of heart tissue
- Positron emission tomography (PET) – to pinpoint affected areas to help in the selection of tissue for biopsy
- Magnetic resonance imaging (MRI) – to investigate the involvement of the heart and central nervous system tissue
- Computed tomography (CT) scan – to investigate involvement of lung tissue
- Eye examination – to detect eye involvement and evade serious vision deterioration
- Urine dipstick test – to investigate signs of abnormalities in the kidneys
Understanding Sarcoidosis: A Visual Guide for Students
References
Further Reading
Last Updated: Nov 28, 2022