Listeria is a bacterial genus responsible for listeriosis, a significant foodborne disease that can be difficult to control and that frequently results in severe clinical outcomes. The most important species for humans is Listeria monocytogenes, often labeled as a leading cause of death due to contaminated foods.
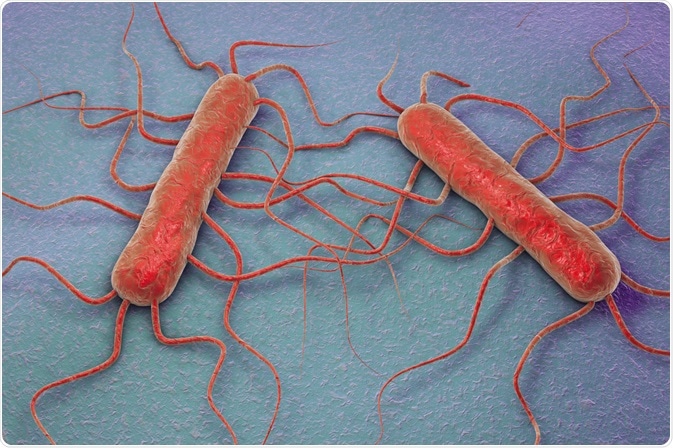 Image Credit: Kateryna Kon/Shutterstock.com
Image Credit: Kateryna Kon/Shutterstock.com
Besides Listeria monocytogenes, six more currently recognized species are found in this genus: Listeria innocua, Listeria ivanovii, Listeria seeligeri, Listeria welshimeri, Listeria martii, and Listeria grayi. Listeria ivanovii is sporadically associated with abortions in animals, but there have been some reports of this species (alongside Listeria seeligeri) causing illness in humans.
Listeria may have been recognized as early as 1891 in tissue samples from German patients. It was isolated from the liver of rabbits in 1911 in Sweden, and the disease’s syndrome was recognized in sheep in Germany in 1925. The genus was named after Sir Joseph Lister, the father of modern antiseptic surgery.
Characteristics of Listeria species
All Listeria species are gram-positive, facultatively anaerobic bacteria with both psychrotrophic (thriving in a cold environment) and mesophilic (growing in moderate temperature) features. Based upon the low guanine-cytosine content of its genome, the genus is placed in the Clostridium sub-branch of gram-positive bacteria.
Morphologically, they are short rods measuring 0.4-0.5 µm by 0.5-2.0 µm with rounded ends. They can be curved in single or short chains, often in a “V” shape. Listeria monocytogenes is motile due to one to five peritrichous flagella, and filaments up to 20 µm in length may develop in older cultures.
Listeria species strains are stereotyped based on the cellular (“O”) and flagellar (“H”) antigens, and full serological description is given by Seeglier and Donker (based on 15 “O” and 5 “H” antigens). More than 95% of human infections caused by strains of Listeria monocytogenes belong to serotypes 1/2a, 1/2b, and 4b.
The decomposing plant matter is considered to be the natural habitat of these bacteria, as they can live there as saprophytes. In addition, domesticated ruminants possibly play a pivotal role in the maintenance of Listeria in the rural environment through a continuous fecal-oral enrichment cycle.
Epidemiology of listeriosis
Changes in food production and the demands of a growing society have increased the burden of foodborne illnesses. Listeria monocytogenes is especially challenging to handle during food processing, as it can multiply over a wide range of temperatures, especially at refrigerator temperatures.
This serious invasive disease primarily afflicts vulnerable populations such as pregnant women, neonates, the elderly, and immunocompromised adults. The disease is mainly caused by the consumption of contaminated ready-to-eat food, with soft cheeses made from raw milk and ready-to-eat meats posing the highest threat to susceptible individuals.
Listeria monocytogenes is estimated to cause approximately 1600 illnesses each year in the United States with more than 250 related deaths. Since 2001, an increase in the number of listeriosis cases has been observed in several European Union countries, predominantly in the population older than 60.
The incidence of infection increases with age, thus the mean age of adult infections is higher than 55 years of age. Immunosuppression is considered a major factor in this shift for both the epidemic and sporadic forms of listeriosis. Furthermore, infections with this pathogen usually occur in urban populations.
Albeit person-to-person transmission outside the hospital setting has never been persuasively demonstrated, the nosocomial spread of Listeria monocytogenes is well recognized, particularly on neonatal units. Routes of transmission include rectal thermometers, contaminated resuscitation equipment, as well as mineral oil applied to the skin of newborns. Nosocomial listeriosis may also be foodborne in origin.
What is Listeria monocytogenes and how does it cause food poisoning?
References
- Listeria (Listeriosis) | Listeria | CDC (2021). Available at: https://www.cdc.gov/listeria/ (Accessed: 28 September 2021).
- (2021) Journals.asm.org. Available at: https://journals.asm.org/doi/pdf/10.1128/cmr.14.3.584-640.2001 (Accessed: 28 September 2021).
- Silk, B. et al. (2014) "Foodborne Listeriosis Acquired in Hospitals", Clinical Infectious Diseases, 59(4), pp. 532-540. doi: 10.1093/cid/ciu365.
- Guillet, C. et al. (2010) "Human Listeriosis Caused byListeria ivanovii", Emerging Infectious Diseases, 16(1), pp. 136-138. doi: 10.3201/eid1601.091155.
- de Noordhout, C. et al. (2014) "The global burden of listeriosis: a systematic review and meta-analysis", The Lancet Infectious Diseases, 14(11), pp. 1073-1082. doi: 10.1016/s1473-3099(14)70870-9.
- https://sochinf.cl/
- Wagner M, McLauchlin J. Biology. In: Liu D. Handbook of Listeria Monocytogenes. CRC Press, 2008; pp. 1-26.
Further Reading
Last Updated: Apr 8, 2023