Infections with Salmonella species represent a significant public health problem due to their large and varied animal reservoir, presence of human and animal carrier states, and the lack of coordinated programs for control. Although cases of human salmonellosis have been steadily declining since 1995, it remains one of the most important human food-borne diseases.
Salmonella has evolved to live in the gastrointestinal tracts of animals. Thus the primary sources of contamination are animals and their feces. In recent years, the significance of foods of vegetable origin as likely vehicles of gastrointestinal infection has been highlighted.
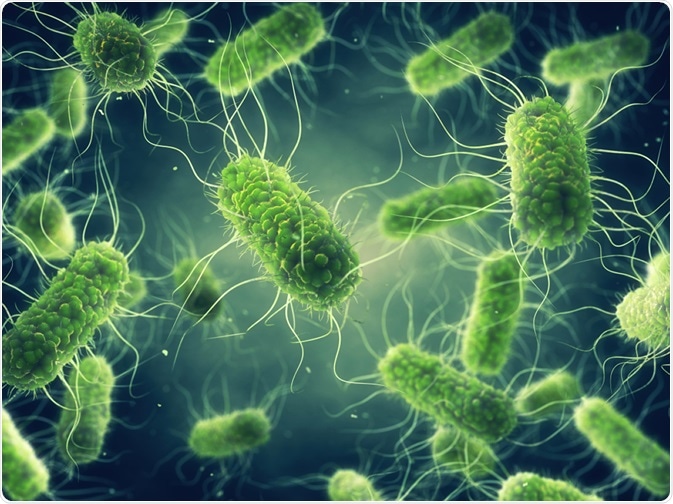
Pathogenic Salmonella bacteria. Image Credit: nobeastsofierce / Shutterstock
Principal sources of infection
Different animals can be infected with Salmonella, most often without any obvious clinical symptoms. The most common animal reservoirs are chickens, pigs, turkeys, and cows, although various wild animals such as birds, reptiles, frogs, and fish can carry the bacteria. As salmonellae are able to survive in meats and animal products that are not thoroughly cooked, animal products still represent a main vehicle of transmission.
Consequently, raw meats and unpasteurized milk are regarded as especially important sources of infection. Other high-risk products are raw or partly cooked eggs, homemade mayonnaise, and ice cream, unpasteurized fruit juices, and lightly cooked or raw seed sprouts.
Despite strong evidence between the food of animal origin and human salmonellosis, other modes of infection are also important – some examples are cross-contamination at home and commercial kitchens, exposure to pets (namely dogs, cats, pet tortoises, and snakes), through contact with other people, and ingestion of vegetables and fruits.
Certain Salmonella serotypes are species-specific, but many are able to cross between species and cause disease in humans. They can be subsequently shed in the feces of infected individuals after symptoms have subsided, and some patients can also become chronic carriers. Nevertheless, a foodborne disease caused by an infected food handler is rarely observed and typically arises as a result of poor personal hygiene.
The incidence of salmonellosis among infants is approximately eight times greater than the incidence among other age groups. Several large outbreaks of Salmonella infection can be traced back to contaminated powdered infant formula, resulting in diarrhea and (in some infants) bacteremia and meningitis.
Preventive measures
Hazard Analysis & Critical Control Points (HACCP) represents a systematic preventive approach to food safety, which is also pivotal for the effective control of Salmonella. Prevention should start on the farm, therefore policies that encourage measures to reduce the levels of Salmonella in poultry houses, units for egg production, during the growing of fresh produce, and during transport were developed.
Food manufacturers should take keep track of the source of their ingredients and insist that producers implement effective controls, or exclusively purchase pasteurized products to reduce the risk of Salmonella contamination. In short, risk reduction strategies should be employed throughout the food chain.
Salmonella can be adequately controlled by relatively mild heat treatments, but effective measures should be in place in order to avoid cross-contamination between raw and cooked foods. HACCP should be used to identify and implement adequate controls in all foods that will be supplied to the consumer as ready-to-eat.
Attentive handling and storage should be encouraged at the retail stage and in the consumer’s home to ensure that ready-to-eat foods remain Salmonella-free. Careful labeling for raw products is of uttermost importance as well, and consumers should be repeatedly reminded to thoroughly wash fresh produce, even when it appears safe.
European Union regulations cover Salmonella in a wide range of products, with specific requirements for Salmonella testing of cattle, poultry, goats, sheep, horses, and pig carcasses. Likewise, US food law requires Salmonella to be completely absent from ready-to-eat food products that are not intended to be heated before eating.
Infectious Diseases A-Z: Salmonella safety
Sources
- japr.oxfordjournals.org/content/20/1/102.full
- www.ijern.com/images/January-2013/c-02.pdf
- http://cid.oxfordjournals.org/content/46/2/268.full
- drum.lib.umd.edu/bitstream/1903/2072/1/umi-umd-2037.pdf
- www.scielo.br/scielo.php
- Humphrey T. Public health aspects of Salmonella enterica in food production. In: Mastroeni P, Maskell D. Salmonella Infections: Clinical, Immunological and Molecular Aspects. Cambridge University Press, 2006; pp. 89-116.
Further Reading
Last Updated: Feb 17, 2021