Research published this week estimates that the risk of dying from early stage breast cancer within 20 years of diagnosis is very low (3.3%).
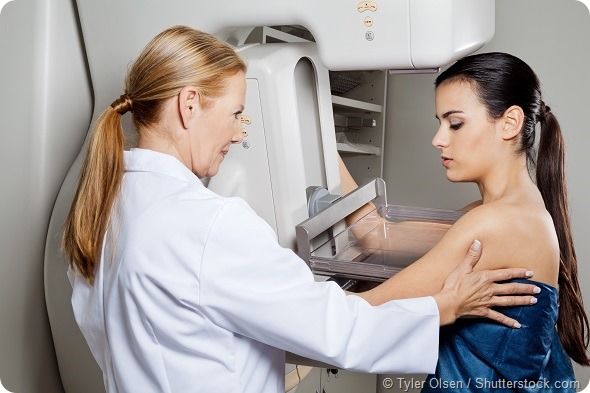
About one fifth of breast cancers detected through routine mammograms are at an early stage; some cells in ducts within the breast have become cancerous, but have not yet started spreading into the surrounding tissue.
This is known as ductal carcinoma in situ breast (DCIS) or stage zero cancer. Such cancers can be easily removed surgically. However, some women can subsequently develop a second breast cancer after having a DCIS breast cancer removed and this may (in a low proportion of patients) be invasive and ultimately fatal.
Steven Narod MD and colleagues analysed data in the Surveillance, Epidemiology and End Results (SEER) 18 registries database to see if they could identify factors predictive of mortality after a DCIS diagnosis.
The study included data from 108,196 women diagnosed with DCIS between 1988 and 2011. The average age at diagnosis was 54 years and the women had follow-up data covering an average of 7.5 years.
The analysis found the risk of dying from breast cancer within 10 years of DCIS diagnosis to be 1.1%. Although low, this is still 1.8 times higher than the breast cancer mortality rate in the general population.
At 20 years after a DCIS diagnosis, the overall mortality rate was 3.3%. This rate more than doubled among women who developed DCIS before the age of 35 years and for black women.
Although, it is generally considered that an invasive recurrence on the same side (ipsilateral) as the DCIS is associated with a greater risk of dying from breast cancer, this study showed that preventing an ipsilateral invasive recurrence did not prevent death from breast cancer.
Although radiotherapy reduced the risk of ipsilateral invasive recurrence, it did not reduce the risk of dying from breast cancer within 10 years of DCIS diagnosis.
Interestingly, patients undergoing single mastectomy had a higher breast cancer 10-year mortality rate than those undergoing radiotherapy, despite having a lower risk of ipsilateral invasive recurrence. Thus, more aggressive treatment of DCIS does not necessarily reduce breast cancer mortality.
The authors concluded:
Some cases of DCIS have an inherent potential for distant metastatic spread. It is therefore appropriate to consider these as de facto breast cancers and not as pre-invasive markers predictive of a subsequent invasive cancer"
In a related editorial, Laura Esserman, and Christina Yaud commented "If we want the future to be better for women with DCIS, we have to be committed to testing new approaches to care."