Sleep Apnea
Sleep apnea is a serious sleep disorder that occurs when a person’s breathing is interrupted during sleep. Untreated, those with sleep apnea stop breathing repeatedly during their sleep. This can happen hundreds of times over a 6 to 8 hours sleep cycle.
When a person stops breathing, the brain – and the rest of the body – may not be getting enough oxygen.
Potentially life-threatening, sleep apnea is far more common than previously thought. It happens in both genders and all age groups. It is estimated that about 25% of men and nearly 10% of women suffer from sleep apnea.
It can affect people of all ages, including infants, but it is more common in those over 40 and overweight.
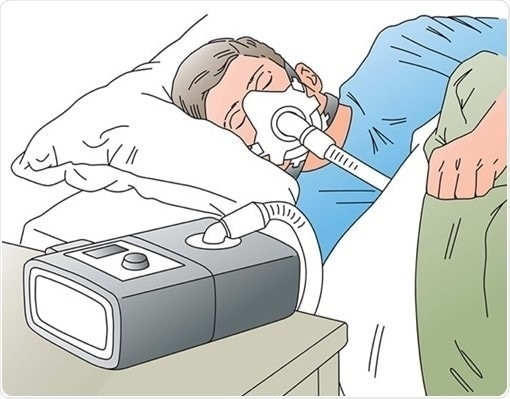
Image Credit: Superior Sensor Technology
According to the Cleveland Clinic, there are two types of sleep apnea: obstructive and central.
- Obstructive sleep apnea is more common and occurs as repetitive episodes of complete or partial upper airway blockage during sleep. During an apneic episode, the diaphragm and chest muscles work harder as the pressure increases to open the airway. Breathing usually resumes with a loud gasp or body jerk. These episodes can interfere with sound sleep, reduce the flow of oxygen to vital organs and cause heart rhythm irregularities.
- In central sleep apnea, the airway is not blocked but the brain fails to signal the muscles to breathe due to instability in the respiratory control center. Central apnea is related to the function of the central nervous system.
If it’s not treated, sleep apnea can cause several health problems, including hypertension (high blood pressure), stroke, cardiomyopathy (enlargement of the muscle tissue of the heart), heart failure, diabetes and heart attacks.
Untreated sleep apnea can also be responsible for job impairment, work-related accidents, motor vehicle crashes, as well as underachievement in school in children and adolescents.
Most common devices to treat sleep apnea
Positive Airway Pressure therapy, or PAP therapy, is the most common and recommended treatment for obstructive sleep apnea.
With PAP therapy, patients wear a mask over their nose and/or mouth and an air blower gently forces air through the mask. The air pressure is adjusted so that it is just enough to prevent the upper airway tissues from collapsing during sleep.
PAP therapy prevents airway closure while in use, but apnea episodes can return if PAP is stopped or if it is used improperly. Properly used, PAP helps patients breathe and maintain good blood oxygen levels throughout the night.
There are three main types of positive airway pressure devices depending on the specific needs of the patient:
CPAP (Continuous Positive Airway Pressure)
CPAP is the most common type of machine. This device is programmed to produce pressurized air at one steady air pressure level. To change the air pressure, you have to reset the device’s settings. If the patient needs more or less pressure during the night, the CPAP is not able to adjust.
BiPAP (Bi-Level Positive Airway Pressure)
BiPAP machines have two pressure settings, one pressure for inhaling and a lower pressure for exhaling.
It is used for individuals who can’t tolerate CPAP machines or have elevated carbon dioxide levels in their blood. BiPAP devices can also come with a backup respiratory rate for patients who have central sleep apnea.
The backup respiratory rate ensures the person breathes, as the main problem with central sleep apnea is initiating breath.
BiPAP is also helpful for other conditions affecting the lungs, such as COPD.
APAP (Automatic Positive Airway Pressure)
APAP machines check a patient’s breathing throughout the night and automatically adjust the air pressure to compensate for changes in sleep position or the effects of medications that may have changed breathing patterns.
Unlike CPAP machines, APAP machines can automatically choose the right pressure setting based on a patient’s breathing needs. This allows for much greater flexibility.
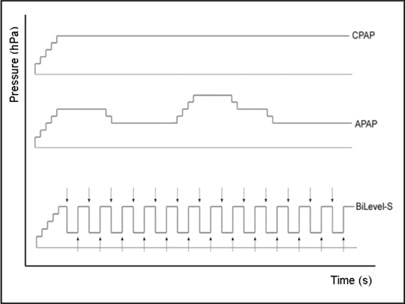
Figure 1. Example of pressure patterns of CPAP vs. APAP vs. BiPAP. Image Credit: NIH
The role of pressure sensors in PAP machines
PAP machines include several types of sensors to monitor and/or regulate different functions, including airflow, air pressure, temperature and humidity.
While adjusting temperature and humidity is important for the patient experience, this article will focus on the two functions that are served by pressure sensors: airflow and air pressure.
As seen in the following use cases, the most effective pressure sensors have a very fast feedback loop (to tell the system to adjust the fan more quickly when a patient is inhaling/exhaling), are able to effectively block out noise from fans and motors (to reduce error rates), can support multiple pressures without any degradation in performance (to support all patient requirements) and have a high-resolution to ensure a very strong signal-to-noise (SNR) ratio.
CPAP
With a CPAP machine, the pressure is set to one fixed value that is constantly applied throughout the treatment. In this implementation, a gage pressure sensor is used to measure the air pressure that is being applied to the patient from the machine.
In some implementations, a second gage sensor is used to monitor the air pressure coming back from the patient to ensure there is no leakage due to an improperly placed mask.
An alternate solution to dual gage sensors is the addition of a differential pressure sensor for measuring flow, which also enables the CPAP device to be configurable for BiPAP and APAP modalities.
BiPAP
As BiPAP machines need to monitor both patient breathing inflows and outflows, they require two pressure sensors: a gage pressure sensor to control the patient’s pressure and a differential pressure sensor for system flow measurement.
Specifically, pressure sensors monitor the patient’s breathing and send a signal to the machine to reduce the applied pressure when a patient exhales and then increase it again when the patient inhales.
Adjusting the applied pressure when inhaling and exhaling results in the patient being much more comfortable, and no longer ‘fighting’ against the sleep apnea machine when exhaling.
APAP
Similar to BiPAP, APAP machines will adjust the applied patient pressure throughout the night. But unlike BiPAP which adjusts between two settings, APAP machines are not limited to only two predefined settings.
APAP machines automatically adjust patient pressure according to the resistance present in the patient’s breathing. While pressure sensors monitor the patient’s breathing and send a signal to the machine, an APAP machine varies the applied pressure based on precise requirements coming from the patient.
Typically, an APAP machine is prescribed when neither a CPAP or BiPAP machine achieves the desired results.
Superior Sensor’s technology advantage
Having an extremely low noise floor, the NimbleSenseTM architecture is ideal for the precise, low-pressure measurements that PAP equipment requires to maximize their accuracy and performance.
In addition, Superior Sensors has gone a step further with its CP Series by integrating the two pressure sensors (gage and differential) in one device. This highly integrated dual sensor solution eliminates the need for a second pressure sensor.
Finally, several application-specific building blocks provide additional capabilities to further improve the sleep apnea solution. These include Multi-Range TechnologyTM, an advanced multi-order filter and integrated closed loop control.
Figure 2. NimbleSense Building Blocks that Benefit PAP Machines. Image Credit: Superior Sensor Technology
About Superior Sensor Technology
Superior Sensor Technology is an innovative, high technology company revolutionizing the high performance, cost driven pressure sensor market by developing integrative, highly intelligent solutions for industrial, HVAC and medical applications.
Our proprietary pressure sensor technology with advanced programmable software features enables customers to develop higher performing, more reliable equipment.
Sponsored Content Policy: News-Medical.net publishes articles and related content that may be derived from sources where we have existing commercial relationships, provided such content adds value to the core editorial ethos of News-Medical.Net which is to educate and inform site visitors interested in medical research, science, medical devices and treatments.