Introduction
Collecting the Cervical Cell Sample
Laboratory Tests
What are Normal Pap Smear Results?
What are Unclear Pap Smear Results?
What are Abnormal Pap Smear Results?
Follow-Up after a Pap Smear
References
The Pap smear test is a helpful screening tool to detect changes in the cells of the cervix that may have the potential to lead to cervical cancer. This aids in recognizing changes earlier and allows treatment to help prevent cervical cancer progression.
Image Credit: Iryna Inshyna/Shutterstock.com
Collecting the Cervical Cell Sample
It is recommended for all women over the age of 18 that have ever been sexually active to have regular Pap smears every two years.
The test involves a cell sample being taken from the cervical wall. This smear is then sent away to a laboratory to be tested for abnormalities associated with HPV and cervical cancer.
Laboratory Tests
A glass slide is used to collect the cells, and the Papanicolaou technique is used in the laboratory to detect abnormal cells. This involves staining the sample cells with tinctorial dyes, which leads selective cells to retain the acides.
Observing how the cells react to the dye allows medical analysts to detect if the cells are normal or abnormal.
What are Normal Pap Smear Results?
If normal results are detected, the woman should be advised that the cells in her cervix are normal at the current time, but she should return for another test in two years to continue monitoring the cervical cells.
What are Unclear Pap Smear Results?
It is also possible for the results to be unclear whether the cell sample is normal or abnormal. In most cases, this will lead to another Pap test after a shorter period of time than the standard recommendation to monitor further changes. Further tests can also be undertaken immediately in some cases to examine the possibility of more serious outcomes.
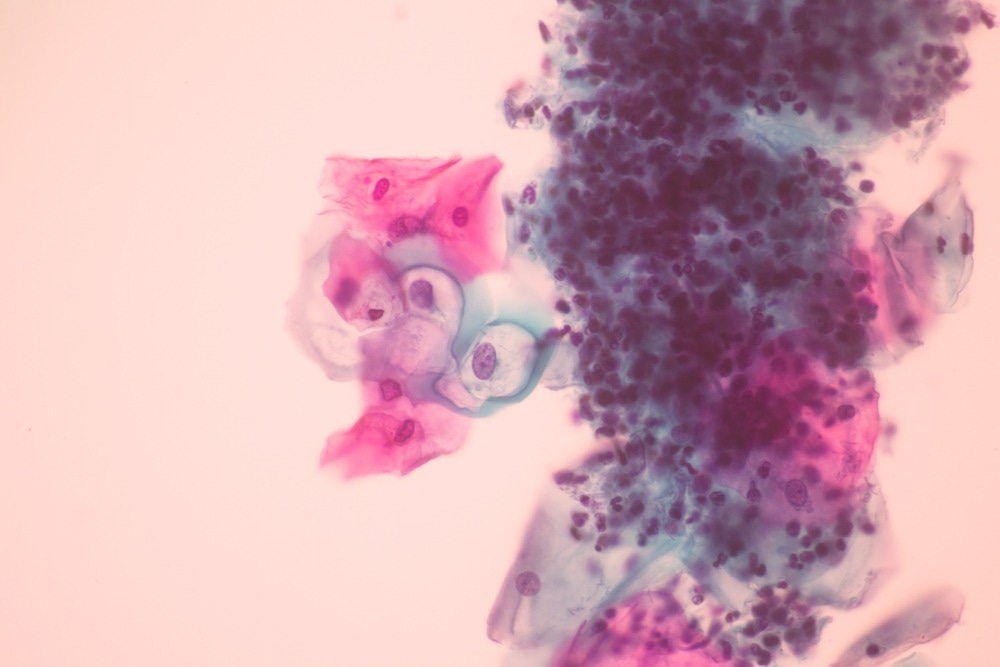
Image Credit: Komsan Loonprom/Shutterstock.com
What are Abnormal Pap Smear Results?
There are several different classes of abnormal Pap smear results.
ASCUS or AGUS refers to abnormal cells without a clear explanation of what the changes signify. They may be due to HPV but may also indicate changes leading to cancer.
Low or high-grade dysplasia (LSIL or HSIL) suggests that there are changes present that have the potential to lead to cancer. This risk is more prominent with HSIL.
Carcinoma in situ (CIS) usually means that there are abnormal changes present that are likely to require treatment to avoid progression to cervical cancer.
Atypical squamous or glandular cells (ASC or AGC) signify abnormal cell changes that may be high-grade dysplasia and require further testing and medical attention.
When any abnormal change is found as a result of a Pap smear, further testing is required to investigate the cell changes and the implications this may have.
Follow-Up after a Pap Smear
The course of action in regards to follow-up depends on the cell abnormality, as well as the previous history of Pap smears and the family history or other individual risk factors for cervical cancer.
If minor changes are evident, another Pap smear is usually recommended in 6 to 12 months to monitor any further cell changes.
A colposcopy-directed biopsy may also be indicated to investigate the current situation further, particularly if more severe changes are present. A HPV test is also used to investigate the presence of the HPV viruses commonly associated with causing cervical cancer.
It is essential that the woman is involved in the follow-up process and understands the implications of each of the tests. Empowering women with information about the follow-up process helps ensure they are on board with successive treatment decisions.
What do my Pap test results mean and how can my partner and I know if we are infected with HPV?
References:
- Healthline. (2015). Pap Smear (Pap Test): Reasons, Procedure & Results. [online] Available at: https://www.healthline.com/health/pap-smear-pap-test-what-to-expect#Candidates3 [Accessed 2 Aug. 2022].
- www.cdc.gov. (2021). What Should I Know About Cervical Cancer Screening? | CDC. [online] Available at: https://www.cdc.gov/cancer/cervical/basic_info/screening.htm?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fstd%2Fhpv%2Fpap%2Fdefault.htm [Accessed 2 Aug. 2022].
- medlineplus.gov. (n.d.). Pap test: MedlinePlus Medical Encyclopedia. [online] Available at: https://medlineplus.gov/ency/article/003911.htm.
- Saraiya, M., Martinez, G., Glaser, K. and Kulasingam, S. (2009). Pap Testing and Sexual Activity Among Young Women in the United States. Obstetrics & Gynecology, [online] 114(6), pp.1213–1219. doi:10.1097/aog.0b013e3181be3db4.
Further Reading
Last Updated: Aug 10, 2022