Edema occurs when the capillaries leak fluid into the surrounding tissues of the body, which causes the fluid to accumulate in the area, ultimately leading to swelling. Chronic edema involves the continuation of this effect over several weeks or months; therefore, there is a need to understand the possible causes and the appropriate management of the condition.
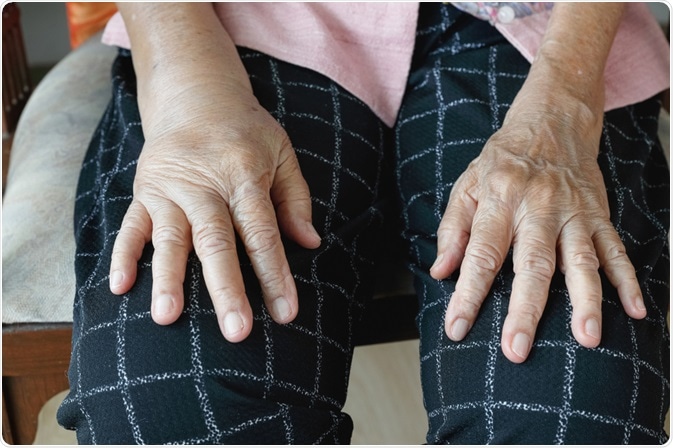
Image Credit: Toa55 / Shutterstock.com
Causes
Some people may experience temporary symptoms of edema due to sitting or staying in one position without moving for too long. A poor diet with a high intake of salty foods is another possible cause of acute edema. Women may experience edema due to hormonal changes as a feature of premenstrual syndrome or pregnancy.
Some medications are also linked to causing edema and can persist for as long as the drug continues to be used. Examples of these may include:
- Antihypertensive medications
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Steroidal drugs
- Estrogen medications
- Thiazolidinedione drugs
However, chronic edema can also be a symptom of an underlying medical condition that should be addressed.
For example, congestive heart failure is a condition that involves the loss of the heart’s ability to pump blood effectively. Blood can pool in the legs, ankles, and feet of the affected patients as a result. In some patients, edema may also affect the abdomen and lungs of patients, leading to symptoms of dyspnea.
Cirrhosis, or damage to the liver, can also lead to the accumulation of fluid in the abdominal cavity and the legs. Chronic venous insufficiency is a condition that involves the weakening of the valves in the veins in the legs, which can lead to the pooling of blood in the legs and, subsequently, the development of edema.
Patients with kidney disease may be affected by the retention of sodium and fluid in the circulatory system, which can result in chronic edema. This usually causes swelling in the legs and around the eyes. Likewise, damage to the kidneys linked to nephrotic syndrome can also cause edema.
Damage to the lymphatic system can also contribute to the development of chronic edema due to the ineffective clearing of fluid from the tissues, which is otherwise normally carried out by the lymph nodes and vessels.
What is Edema or swollen feet and legs?
Management
In most cases of mild edema, the symptoms resolve spontaneously. However, there may be a need for medical treatment, particularly in cases of severe or chronic edema.
Diuretic medications such as furosemide are commonly recommended to increase elimination of fluid from the body via the urinary tract. This is particularly useful to elicit a fast response and reduce symptoms quickly.
For the management of chronic edema, which can include patients who repeatedly experience edema symptoms, it is essential to establish the underlying cause of the condition so that it can be addressed. This usually involves a comprehensive medical history, including the nature of symptoms and any relation to concurrent health conditions or medications. It may be necessary to change treatment options for health conditions to reduce edema.
Several non-pharmaceutical management techniques can help to reduce edema symptoms. Changes in the diet, such as reducing the consumption of salt can reduce retention of fluid. Increasing daily activity levels can allow patients to move the affected area, which can encourage blood blow that can help to reduce swelling.
Gently massaging the swollen area can also encourage the excess fluid to move away from the affected area. Additionally, wearing compression stockings or gloves can help to prevent the accumulation of fluid. Holding the affected area above the level of the heart several times a day can also contribute to a reduction in pressure in the edematous area.
Finally, it is important for the patient affected by chronic edema to protect the area and keep it from being injured. It is important to keep the area clean and well moisturized, which will help to strengthen the skin so that it does not crack as easily.
References
Further Reading
Last Updated: Apr 26, 2021