Endoscopic retrograde cholangiopancreatography (ERCP) is a medical technique that is used primarily to investigate and treat pathologies involving the biliary tree and pancreatic ducts.
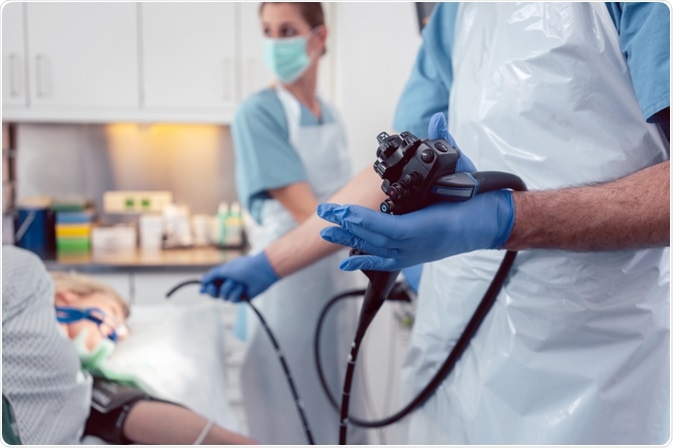
Image Credit: Kzenon / Shutterstock.com
Indications that could warrant the need for ERCP include gallstones, tumors, defective sphincters, sclerosis of ducts, and pseudocysts, the latter of which are accumulations of fluid and tissue components.
ERCP has traditionally been used for diagnostic purposes. However, with the advent of safer and less invasive advances in imaging technologies such as ultrasound and magnetic resonance cholangiopancreatography (MRCP), ERCP is now mainly used for therapeutic interventions.
Preparation for the ERCP procedure
Patients are required to fast for at least 6 hours prior to undergoing the ERCP procedure. This ensures that the stomach is empty, which is an essential requirement for ERCP.
Patient-specific preparation with regards to any medications that may have to be taken, drug allergies, or co-existing medical conditions is taken into account prior to the procedure. Cardiovascular, neurological, and/or cardiopulmonary disorders should be reported to the physician as these, if unstable, are detrimental to the procedure. Furthermore, any jewelry should be removed to avoid X-ray interference.
ERCP : What to Expect | IU Health
The procedure
The ERCP procedure typically takes about an hour and intravenous (IV) sedation may be administered to help the patient relax. The throat is locally anesthetized and the patient is placed in a prone or semi-prone position before the insertion of the duodenoscope through the mouth. Caution is taken when passing the endoscope through the esophagus and stomach since there is limited visibility. If at any point there is resistance to the passage of the scope, the procedure is abandoned and this resistance is investigated with the help of gastroscopy.
Once the duodenoscope has successfully passed through the stomach and entered the duodenum, its tip is manipulated to view the major duodenal papilla, which can be visualized as a pinkish protuberance at the junction of the horizontal-vertical duodenal folds. Appropriate positioning of the duodenoscope is critical if proper cannulation of the biliary or pancreatic ductal system is to be achieved.
Traditional cannulation has been achieved with the help of injecting contrast material to confirm proper positioning. However, there is now data to support the use of wire guidance, which uses a wire under fluoroscopy, as it is associated with lower incidences of post-ERCP pancreatitis and other ERCP complications. Taking this into account, wire guidance has become the preferred cannulation method.
Once the wire is confirmed to be in the proper position, the cannulation device is advanced into position and a radiopaque contrast agent is injected. At this point, a cholangiogram or pancreatogram may be obtained to assess abnormalities and allow for the appropriate therapeutic interventions to be introduced. For instance, a biliary sphincterotomy may be performed in cases of gallstones to ease the passage of stones through the bile duct. In cases of biliary stricture, a stent may be introduced to alleviate the secondary obstruction.
After the procedure
After the ERCP procedure has been completed, patients are typically monitored for 1 to 2 hours or until the effects of the sedatives wear off. The throat may feel a bit sore for a couple of days; however, patients may resume their normal diets and continue any other existing medications unless otherwise specified. Complications that may arise include infections, pancreatitis, and hemorrhage. Should a patient develop fever, vomiting, or worsening abdominal, chest or throat pain, medical care should be urgently sought.
References
Further Reading
Last Updated: Mar 13, 2023