Genital mycoplasmas are a group comprising the smallest self-replicating organisms that have the capability for cell-free existence. They are characterized by the lack of a rigid cell which confers pleomorphic features upon their cells, but also makes them extremely susceptible to dehydration.
Although some species can be present in the female genital tract as commensal microbial flora, Ureaplasma urealyticum, Mycoplasma hominis and Mycoplasma genitalium have been shown to cause several distinct clinical entities. These may range from bacterial vaginosis and cervicitis, to adverse effects on female fertility.
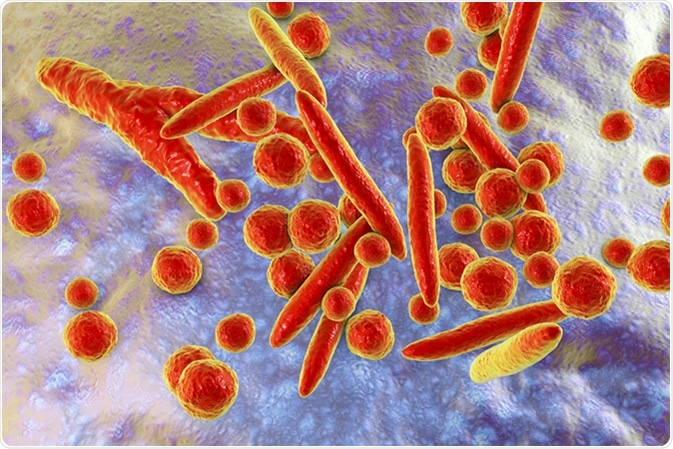
Mycoplasma bacteria, 3D illustration showing small polymorphic bacteria which cause pneumonia, genital and urinary infections. Image Credit: Kateryna Kon / Shutterstock
Common Clinical Syndromes in Women
Bacterial vaginosis is a vaginal inflammation caused by a synergistic overgrowth of various microorganisms, with genital mycoplasmas playing a major role in its development in association with Gardnerella vaginalis and anaerobic bacteria. Both Ureaplasma urealyticum and Mycoplasma hominis have been linked to bacterial vaginosis, causing 62-92% and 58-76% of cases, respectively.
Also, the association between Mycoplasma genitalium and cervicitis (i.e. the inflammation or irritation of the lining of the uterine cervix) has been suggested, although the exact mechanism is still controversial. Women with such cervicitis more often report bleeding after vaginal intercourse when compared to women who do not harbor Mycoplasma genitalium.
Cervicitis usually precedes pelvic inflammatory disease (PID), which is a serious infection of the upper genital tract with potential consequences for reproductive health. Microorganisms ascend from the lower genital region to the uterus, fallopian tubes and ovaries. A large study of women with clinically suspected PID has shown that Mycoplasma genitalium was as prevalent as Chlamydia trachomatis and Neisseria gonorrhoeae in this disease.
The adverse effect of Mycoplasma hominis on the epithelial lining of the Fallopian tubes in a laboratory environment was established more than four decades ago, and this pathogen has been isolated from the endometrium (the lining of the uterus) and the fallopian tubes of about 10% of women with salpingitis (i.e. an acute inflammation of the fallopian tubes). Moreover, the symbiotic relationship of Mycoplasma hominis with the protozoan parasite Trichomonas vaginalis may lead to co-infection and, in turn, worsen the clinical presentation.
The Influence on Female Fertility
Infertility associated with Ureaplasma urealyticum was initially reported in 1970 and subsequently corroborated by several other studies that demonstrated a high frequency of infection in infertile women. But although Ureaplasma urealyticum has been isolated from the affected fallopian tubes, it was chiefly as a part of a polymicrobial infection. Hence we still do not have all the answers as to whether this genital mycoplasma is responsible for a small proportion of infertility cases, or whether it is merely a coincidental finding.
On the other hand, research on Mycoplasma genitalium as a cause of infertility in women has shown a significant relationship. Studies have demonstrated a high correlation of laparoscopically proven tubal infertility and the presence of specific antibodies to this mollicute in the serum.
Moreover, in one study on Polish women Mycoplasma genitalium was detected by polymerase chain reaction (PCR) more commonly in cervical swabs from infertile patients than in healthy and fertile women, indicating that even the results of cervical swab analysis may forecast the infection of the upper genital tract.
References
- http://www.antimicrobe.org/m06.asp
- http://cmr.asm.org/content/18/4/757.full
- https://www.hindawi.com/journals/idog/2016/4513089/
- https://www.hindawi.com/journals/jpath/2014/183167/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2564705/
- http://journals.sagepub.com/doi/abs/10.1258/0956462021924695?journalCode=stda
- Blanchard A, Bébéar CM. Mycoplasmas of Humans. In: Razin S, Herrmann R, editors. Molecular Biology and Pathogenicity of Mycoplasmas. Springer Science & Business Media, 2007; pp. 45-72.
- Mendoza N, Ravanfar P, Shetty AK, Pellicane BL, Creed R, Goel S, Tyring SK. Genital Mycoplasma Infection. In: Gross G, Tyring SK, editors. Sexually Transmitted Infections and Sexually Transmitted Diseases. Springer Science & Business Media, 2011; pp. 197-202.
Further Reading
Last Updated: Feb 26, 2019