Written by Keynote Contributor, Dr. Praveen Bhatia, MBBS, FRCP
An introduction to COLDOSA
In the medical sphere, we love acronyms. You might visit your GP, who manages your chronic obstructive pulmonary disease (COPD), to decide whether you need continuous positive airway pressure (CPAP) or long-term oxygen therapy (LTOT). By using acronyms, we can save precious seconds during our busy workload. Unfortunately, this can lead to much confusion when the medical jargon gets in the way of a patient's understanding of their condition.
Introducing the mother of all medical acronyms – COLDOSA (Chronic Obstructive Lung Disease and Obstructive Sleep Apnoea). Luckily for our baffled patients, we can simplify this by calling it Overlap Syndrome – or OS for short.
Overlap syndrome, or COLDOSA, is the name given when a patient is suffering from both chronic obstructive pulmonary disease and obstructive sleep apnoea. Combined, these conditions cause a significant drop in oxygen during sleep, leading to an increased risk of disability and death.

Image Credit: Kateryna Mostova/Shutterstock.com
What is the overlap between COPD and OSA?
The word overlap might suggest that COPD have shared characteristics – but in this case, the "overlap" is a misnomer. Instead, these are two common and separate conditions, both of which affect your airways in different ways. When someone suffers from both conditions, the "overlap" refers to how the conditions interact to increase the risks beyond what would be expected from each condition.
COPD is a condition usually caused by smoking, in which you develop progressive obstruction of airflow to the alveoli in your lungs due to chronic inflammation. Put simply, regularly inhaling smoke, or noxious fumes irritates the lungs, leading to irreversible narrowing of your airways, making it harder to breathe. COPD has a high morbidity rate and mortality.
Obstructive Sleep Apnoea (OSA) is another common condition in which the walls of the throat relax during your sleep, leading to the intermittent collapse of your airway. This is associated with heavy snoring and gradually dropping oxygen levels during sleep, eventually resulting in a sudden awakening. This leads to interrupted sleep and excessive daytime sleepiness and increases the risk of high blood pressure, heart disease, and stroke.
COPD and OSA are both very common conditions – in the UK, approximately 1.17 million people have been diagnosed with COPD and 1.5 million with OSA. This is just the number of patients who have reached a diagnosis – the true prevalence of both COPD and OSA in adults over 40 is thought to be between 5 and 10%.
Even if we ignore the shared risk factors, such as smoking and advancing age, the chance of a patient suffering from both conditions is relatively high – roughly 1 in 200 adults over 40.
How these conditions work together to damage your health
During sleep, particularly in the rapid eye movement (REM) phase, the muscles of our upper airway, diaphragm and chest wall relax. Normally, this doesn't cause a significant problem, and we can still get a long and restful sleep.
In patients with OSA, this restful sleep becomes nearly impossible as the relaxed upper airway collapses completely during REM sleep. This is due to additional pressure around the throat, such as obesity and peripheral oedema, or narrowed airways resulting from nasal congestion or enlarged tonsils. When the airway collapses, you cannot breathe, causing hypoxia (low oxygen levels) until the brain's sensors kick in and wake you up. This results in arousals, interrupted sleep, and repeated periods of low oxygen levels during the night. This is thought to cause a surge of catecholamine release, leading to increased pulmonary arterial pressure and hypertension and right-sided heart failure.
Patients with COPD also have similar problems with poor sleep. As the lungs are scarred and the airways narrow, the lungs cannot compensate for the reduced movement of the chest wall during REM sleep, so breathing becomes ineffective during this stage of sleep. Almost half of patients with COPD report difficulties getting to or staying asleep, and 70% of patients are reported to have a drop in their oxygen levels overnight.

Image Credit: Dai Yim/Shutterstock.com
When combined, the effects of OSA and COPD lead to even more fragmented sleep and frequent episodes of nocturnal hypoxaemia – low oxygen levels during the night. For reasons still not fully understood, these effects are synergistic, and the combined risks are greater than the sum of their parts.
In the short term, nocturnal hypoxaemia results in fatigue, poor concentration, and daytime somnolence (sleepiness). The real risk, however, is in the long-term effects of prolonged nocturnal hypoxaemia. A sustained drop in oxygen level promotes inflammation in the body, which is repeated multiple times on a nightly basis and leads to a chronic state of inflammation. This state of inflammation can cause several conditions, including:
- Hypertension
- Stroke
- Pulmonary Hypertension
- Right-sided heart failure
- Arrhythmias such as atrial fibrillation
- Cognitive impairment due to its effect on mammillary bodies
- Increased risk of type 2 diabetes mellitus
This can also become a vicious cycle if improperly treated. Right-sided heart failure causes a build-up of fluid in the body, which can put additional pressure around the throat and increase the likelihood and severity of OSA. This can then exacerbate the state of chronic inflammation and lead to worsening heart failure.
There are also long-term impacts of poor-quality sleep. Those who suffer from problems sleeping are more likely to have feelings of anxiety and depression, and poor sleep is associated with an increased risk of:
- Mania
- Psychosis
- Road traffic and workplace accidents
- An underproductive workforce
- Suicide
Patients with COPD are already at risk of depression and anxiety, so worsening sleep quality adds to the mental health burden that these patients face.
Diagnosing overlap syndrome
A major factor we need to consider when approaching overlap syndrome is that both COPD and OSA are significantly underdiagnosed. Studies have suggested that up to 70% of those with COPD do not have a formal diagnosis and that up to 1 billion people suffer from OSA – up to 50% of adults in some countries.
As both conditions require specialist equipment for diagnosis, a solution to identifying those with overlap syndrome could be to screen patients who currently have a diagnosis of COPD or OSA. Using specialist diagnostic equipment for this purpose would take up significant resources, so we can incorporate a pre-screening questionnaire into routine care to direct our resources more appropriately.
For patients with OSA, those who could go on to have formal screening tests for COPD include:
- Patients with a significant history of smoking or exposure to noxious fumes
- Those who have evidence of wheeze, pursed-lip breathing, and breathlessness on examination.
- Patients with symptoms suggestive of COPD including:
- Breathlessness
- Wheezing
- Persistent cough with phlegm
- Frequent chest infections
For patients with COPD, screening for OSA is more difficult. In severe COPD, it is much harder to discern whether sleep symptoms are due to COPD or overlap syndrome. For this reason, screening all patients with severe COPD for OSA might be appropriate. For those with mild-moderate COPD, patients who might qualify for formal screening tests include those who suffer sleep symptoms which are inconsistent with the severity of their COPD, including:
- Loud snoring
- Daytime sleepiness and difficulty concentrating
- Frequently waking during sleep
- Suddenly waking from sleep, gasping for air
- Dry mouth and sore throat after waking
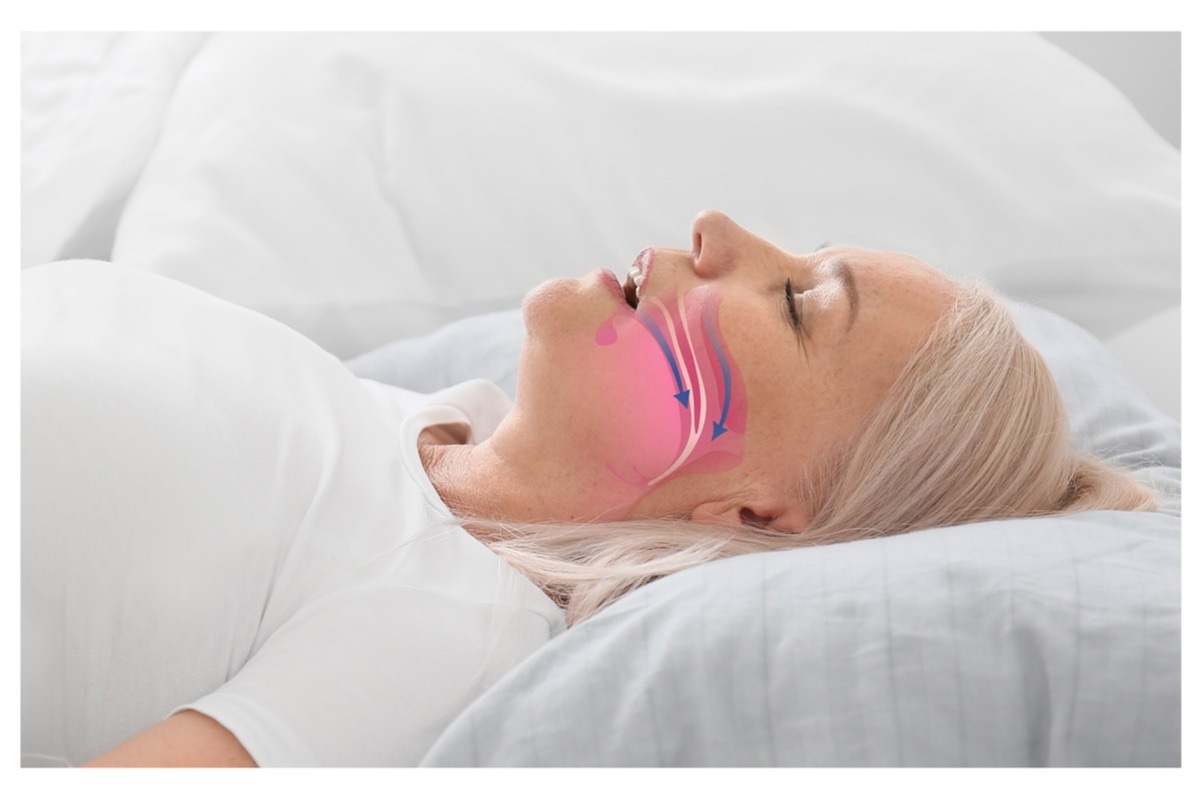
Image Credit: Pixel-Shot/Shutterstock.com
The Epworth sleepiness scale might be an appropriate questionnaire to pre-screen for OSA, though this must be read in the context of COPD, which can cause similar sleep symptoms. Overnight pulse oximetry is a simple screening test that can rule out OSA. Those with a positive test can then be referred for a more detailed assessment with polysomnography.
Treatment of overlap syndrome
If overlap syndrome is confirmed, it is vital that the parent specialities of each condition – respiratory medicine and sleep medicine – work together to create a plan to reduce the risks of this deadly combination. The world of medicine can sometimes move slowly, so we must educate the new generation of doctors on this novel syndrome through continuous professional development.
The mainstay of treatment for overlap syndrome is ensuring that COPD treatment is optimised and Continuous Positive Airway Pressure Ventilation (CPAP) – a device the patient uses every night to prevent a drop in their oxygen level while asleep. CPAP works by providing a constant stream of air at high pressure via a face mask or nasal prongs. These machines help the airways to remain open and the lungs better cope when the patient's muscles relax during REM sleep. CPAP, often used as a treatment for OSA and severe COPD, has significantly reduced mortality for patients with overlap syndrome.
Recently, there has been debate around whether Non-Invasive Ventilation (NIV) – air pressure delivered via a mask that changes between high and low pressure to assist breathing – has an additional mortality benefit over CPAP. While some authors suggest that it is time to make this the first-line treatment, there is some reluctance to change guidelines as the evidence base for this is currently lacking.
In addition to treatment with CPAP or NIV, both conditions benefit from lifestyle modification such as structured exercise programmes and pulmonary rehabilitation. These activities build fitness levels and strengthen chest wall muscles to help the patient's lungs to compensate during sleep. COPD must also be treated as usual with bronchodilators, corticosteroids, smoking cessation, and sometimes supplemental oxygen.
Finally, both OSA and COPD can be associated with and worsened by gastro-oesophageal reflux disease (GORD), which should be actively looked for and managed by the treating provider. This combination introduces a new potential acronym – COLDOSAGORD.
Summary
The number of patients suffering from overlap syndrome – a combination of chronic obstructive pulmonary disease (COPD) and obstructive sleep apnoea (OSA) – is likely to be greatly underestimated, which is worrying given the significant risk to life this syndrome presents.
Not only do patients with overlap syndrome face risks to their health and life, but the lack of good sleep can lead to poor quality of life and increases the risk of mental health conditions. To overcome this often-unrecognised challenge, we must incorporate screening tools into our standard care for COPD and OSA to ensure that these patients receive the proper care.
References
- Singh S, Kaur H, Singh S, Khawaja I. The Overlap Syndrome. Cureus. 2018;10(10):e3453. Published 2018 Oct 15. doi:10.7759/cureus.3453
- Owens RL, Malhotra A. Sleep-disordered breathing and COPD: the overlap syndrome. Respir Care. 2010;55(10):1333-1346.
- (OHID), O. (2022). Inhale - INteractive Health Atlas of Lung conditions in England - Data - OHID. Retrieved 2 July 2022, from https://fingertips.phe.org.uk/profile/inhale/data#page/3/gid/8000008/pat/15/par/E92000001/ati/167/are/E38000006/iid/253/age/1/sex/4/cat/-1/ctp/-1/yrr/1/cid/4/tbm/1/page-options/car-do-0
- Benjafield, A., Ayas, N., Eastwood, P., Heinzer, R., Ip, M., & Morrell, M. et al. (2019). Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. The Lancet Respiratory Medicine, 7(8), 687-698. doi: 10.1016/s2213-2600(19)30198-5
- Diab, N., Gershon, A., Sin, D., Tan, W., Bourbeau, J., Boulet, L., & Aaron, S. (2018). Underdiagnosis and Overdiagnosis of Chronic Obstructive Pulmonary Disease. American Journal Of Respiratory And Critical Care Medicine, 198(9), 1130-1139. doi: 10.1164/rccm.201804-0621ci
- Ioachimescu OC, Janocko NJ, Ciavatta MM, Howard M, Warnock MV. Obstructive Lung Disease and Obstructive Sleep Apnea (OLDOSA) cohort study: 10-year assessment. J Clin Sleep Med. 2020;16(2):267-277. doi:10.5664/jcsm.8180
- Freeman, D., Sheaves, B., Goodwin, G. M. (2017). The effects of improving sleep on mental health (OASIS): a randomised controlled trial with mediation analysis. The Lancet. Psychiatry, 4(10), 749–758. https://doi.org/10.1016/S2215-0366(17)30328-0
- Pumar MI, Gray CR, Walsh JR, Yang IA, Rolls TA, Ward DL. Anxiety and depression-Important psychological comorbidities of COPD. J Thorac Dis. 2014;6(11):1615-1631. doi:10.3978/j.issn.2072-1439.2014.09.28
- Suri TM, Suri JC. A review of therapies for the overlap syndrome of obstructive sleep apnea and chronic obstructive pulmonary disease. FASEB Bioadv. 2021;3(9):683-693. Published 2021 Jun 11. doi:10.1096/fba.2021-00024
About Dr Praveen Bhatia, MBBS, FRCP
Dr Praveen Bhatia is a Consultant Physician in Respiratory and General Medicine in Stockport, United Kingdom. He has a background in sleep medicine, including sleep-disordered breathing conditions such as obstructive sleep apnoea.
Dr Bhatia graduated from Indira Gandhi Medical College, India, in 1985, migrating to the United Kingdom to pursue his passion for respiratory medicine in 1992. He has held a consultant post in respiratory medicine since 2007 and currently works full-time in the NHS. Dr Bhatia worked tirelessly through the COVID-19 pandemic, providing specialist care for patients with COVID across the hospital.
In addition to his work in the NHS, Dr. Bhatia is an Honorary Senior Lecturer for Manchester Medical School and is a Specialist Clinical Advisor for Medical Education start-up MedCourse.
Disclaimer: This article has not been subjected to peer review and is presented as the personal views of a qualified expert in the subject in accordance with the general terms and conditions of use of the News-Medical.Net website. Dr. Bhatia does not have any conflicts of interest to declare.
Last Updated: Jul 11, 2022