Warts, which are also known as verrucae when appearing on hands and feet, are benign epidermal proliferations caused by the human papillomavirus (HPV). Warts, which are common in the general population at some point in life, can vary in size, appearance, shape, and treatment response, depending on the type of epithelium affected.
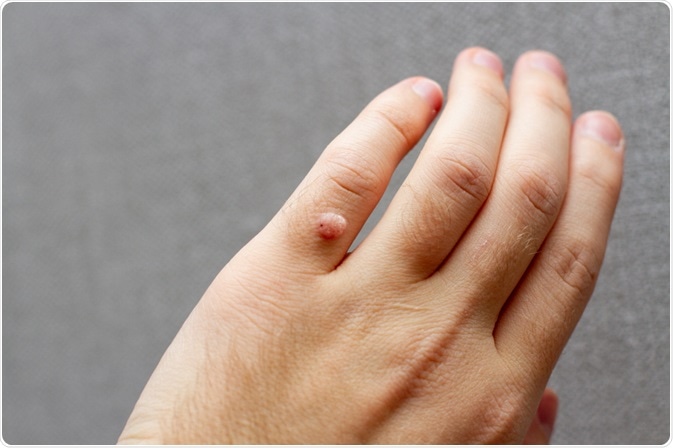
Image Credit: Epov Dmitry / Shutterstock.com
Warts can be categorized into different types. For example, common warts represent individualized nodules or papules with a rough surface and are most commonly observed on the back of hands and fingers. On the other hand, genital warts are soft growths on the skin and mucus membranes of the genital region.
Epidemiology and transmission
HPV infection and the subsequent development of warts that are very commonly observed represent the most common viral infection of the skin, affecting 7% to 10% of the general population. These numbers can be 50 to 100 times higher in immunocompromised individuals, such as kidney-transplant recipients or those on chemotherapy, where it affects more than 90% of patients.
Warts may occur throughout an individual's lifetime; however, there is an increased incidence during school age, reaching a peak in adolescence and early adulthood. Cross-sectional studies conducted in schools have shown that the prevalence of warts in children varies between 2% and 20%. If the workplace is considered a risk factor, handlers of meat, poultry, and fish have a higher prevalence in comparison to other workers.
The virus is transmitted via direct or indirect contact with someone who has the lesion. It is released along with shedding skin cells in a nonlytic manner. Genital warts can be spread during vaginal or anal sex, as well as by sharing sex toys, with condoms not provide complete protection against this condition.
Minor injuries, trauma, or maceration can cause dysfunctions in the epithelial barrier and subsequent loss of continuity in the skin, hence allowing viral infection and the formation of warts. The incubation period ranges from 3 weeks to 8 months after contact, and spontaneous regression is seen in a majority of cases.
Pathogenesis of viral warts
HPV is a small double-stranded DNA virus with a genome of approximately 8,000 base pairs. All types of the virus show tropism for cells of the stratified squamous epithelium; however, the difference in affinity can be observed for various anatomical sites. For example, HPV 1 is a typical representative of skin HPV type that shows a high rate of replication in the keratinized epithelium. Conversely, HPV 16 is a mucosal HPV type with a preference for genital regions.
The life cycle of HPV is linked to the cell differentiation program of the host cell. Initial infection requires access of infectious particles to cells in the basal layer. Note that there is no viral replication at this site and that the virus instead just keeps its genome by amplification of low copy numbers. Replication and the synthesis of proteins occur in the differentiated keratinocytes of the suprabasal layer.
GENITAL WARTS, Causes, Signs and Symptoms, Diagnosis and Treatment.
The development of lesions and their type both correlate with the quantity of detected viral particles. In younger particles, there is a higher amount of viruses in comparison to old ones. Furthermore, plantar warts contain a higher viral load as compared to common warts. It must be noted that in benign lesions, the replication of the HPV genome is extrachromosomal.
The histopathological characteristics of viral warts are acanthosis, papillomatosis, and hyperkeratosis, with the confluence of the epidermal ridges in the center of the lesion and koilocytes. Some authors have also suggested that certain histological features are specific to each type of HPV; thus, a histopathological examination would help in identifying different viral types.
References
Last Updated: Dec 22, 2022