A tracheotomy is a surgical procedure that creates an opening into the trachea from an incision in the back of the neck for the installation of a breathing tube. This enables the patient to breathe without the use of the nose or mouth, which is useful when the upper respiratory tract is obstructed.
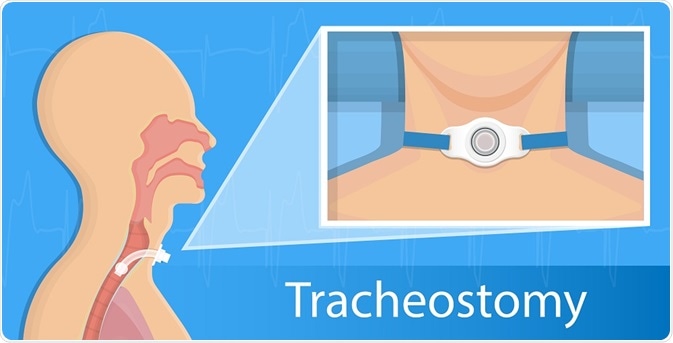
rumrua | Shutterstock
History
Tracheotomy has a long history of use with pictorial evidence on ancient Egyptian artifacts from 3000BC and written records at various points in time from 2000BC and more recently.
However, until the early in the twentieth century tracheotomy was widely regarded as futile and was not widely practiced, despite several isolated successful cases.
In the early 1900s, Chevalier Jackson created a standardized method of surgery that included appropriate post-operative care, which greatly reduced mortality rates associated with the procedure.
The technique has been further developed since this time and is now more commonly used with the introduction of new technology and significantly reduced risk of complications.
When should a tracheostomy be carried out?
A tracheostomy is a very useful surgical procedure that is used in a number of circumstances. This includes an emergency situation to bypass an obstruction of the upper airway and a planned surgical procedure to clean secretions from the airway or deliver oxygen to the lungs.
Some specific situations that may require a tracheotomy include:
- Obstruction of upper airway by foreign body
- Injury to the larynx, neck or mouth
- Severe infection of the upper respiratory tract, such as epiglottis or croup
- Tumor that obstructs the upper airway
- Obstructive sleep apnea
- Chronic pulmonary disease
- Dysfunction of the diaphragm
- Anaphylaxis
- Coma
Surgical procedure
A tracheotomy is usually performed in an operating room of a controlled hospital setting with the patient under general anesthesia.
The most widely used technique usually involves the extension of the neck over a shoulder roll and the endotracheal tube is positioned so that the cuff is level with the middle of the vocal cord.
An incision about 3-4cm in length is made into the inferior border of the cricoid cartilage. The thyroid isthmus should then be pushed down with unobtrusive dissection of the pretracheal tissue. The larynx then needs to be stabilized, a bronchoscopy should be performed and a needle placed at the edge of the light reflex, without touching the posterior tracheal wall.
The needle is then withdrawn but the cannula should remain in the tracheal lumen. A dilator is loaded and used to dilate the tissue between the skin and the tracheal lumen, which prepares the area for the placement of the tracheostomy tube.
Postoperative care is essential to promote the smooth recovery following the procedure and reduce the risk of complications
What are the potential complications?
The modern technique used to perform a tracheotomy is associated with a much lower risk of complication than previous methods, but some complications may arise. These may include
- Bleeding of the trachea or the tracheostomy
- Pneumothorax or trapping of air causing the lungs to collapse
- Collection of air can cause pneumomediastinum or subcutaneous emphysema
- Damage to esophagus or larynx may result in speaking and swallowing difficulties
- Blockage of tracheostomy tube caused by blood clots, mucus or pressure from surrounding airways
- Accidental decannulation or removal of the tracheostomy tube
- Bacterial infection of the trachea
- Damage to the esophagus due to pressure or infection
- Tracheomalacia or erosion of the trachea due to friction
- Development of tracheo-esophageal fistula
- Granulation development that require surgical removal
- Narrowed or collapsed esophagus may lead to difficulty breathing
- Failure to heal following decannulation
Further Reading
Last Updated: Dec 5, 2018