The huge number of specialist terms in medical science can be confusing. One such example is the difference between the established therapeutic technique of focused ultrasound (FUS) and Iconeus’ functional ultrasound (fUS) imaging technology.
This article clearly demonstrates their distinct history, features, and applications. Here, we highlight how both effective ultrasound technologies can complement each other and provide insights into the impact of therapeutic ultrasound on the brain.
History and applications of FUS and fUS
The first FUS device was developed in the 1940s by researchers at the University of Illinois, USA, making it the older of these two technologies. It was observed that the focused ultrasound beams generated by these devices produced tissue lesions, highlighting their potential for tumor treatment and other therapeutic applications.
Several years of investigations were conducted into these high-intensity focused ultrasound (HIFU) technologies, but it was not possible to implement them in clinical applications until the development of imaging-based guiding techniques in the 1990s.
Recent applications have taken this field further, expanding into low-intensity focused ultrasound (LIFU) treatments. LIFU is designed to stimulate or modulate specific tissue functions rather than simply destroying cells.
Its long clinical history means people often think of focused ultrasound therapy rather than functional ultrasound imaging when considering ultrasound in the brain, leading to misunderstandings due to the use of similar abbreviations.
fUS is a relatively new concept that uses very high frame rates to improve the sensitivity of Doppler-based imaging.
This technology was initially developed in the early 2010s by researchers at ESPCI Paris. A few of those founders went on to establish Iconeus in 2016, following further research and proof-of-concept studies.
The potential of fUS for brain imaging has rapidly grown since its initial conception, with the technique now used to study the brain's responses to sensory stimulation or drugs, investigate resting-state functional connectivity, and generate detailed maps of the neurovascular network.
All this work is currently at the preclinical stage, though clinical applications are currently being developed.

Although the concept of fUS was only proposed in 2011, it has rapidly evolved into a fully fledged, user-friendly imaging technology widely adopted in labs worldwide for preclinical brain imaging. Using the Iconeus One imaging station (left) and the scanning platform (center), it’s possible to visualize the brain vasculature (right). Image Credit: Iconeus
Key differences between FUS and fUS
Both FUS and fUS use ultrasound, but each application differs in its hardware and operating mode.
FUS utilizes multiple beams of relatively low-frequency ultrasound (generally within 0.2–3 MHz, depending on the application and target). Mechanical or phased-signal ‘acoustic lenses’ (also known as ‘transmit focusing’) are used to focus these beams on the target.
All this energy is delivered very quickly to prevent heat from dissipating. This also means that the effect remains localized to the target region.
FUS is used to target interventions across the body, including soft tissues, blood vessels, major organs, and the central and peripheral nervous systems.
In contrast, fUS employs a sequence of discrete high-frequency ultrasound pulses (generally 15 MHz in small-animal imaging). These pulses are typically delivered using a linear transducer array to produce a set of unfocused low-energy ‘plane-waves’ across the region of interest. This process is referred to as ‘distributed insonification.’
The same transducer array captures echoes from these pulses, delivering a crisp 2D or 3D image of blood volume distribution.
Unlike FUS, almost all fUS applications involve the brain, where the technique’s high sensitivity offers the most significant advantage over other imaging modalities.
Red blood cells are the principal reflectors in the brain, meaning that fUS provides information on both the vasculature and neuron activity, thanks to neurovascular coupling.
It’s these distinctions that highlight why FUS therapy equipment cannot be used to perform fUS imaging, and vice versa.
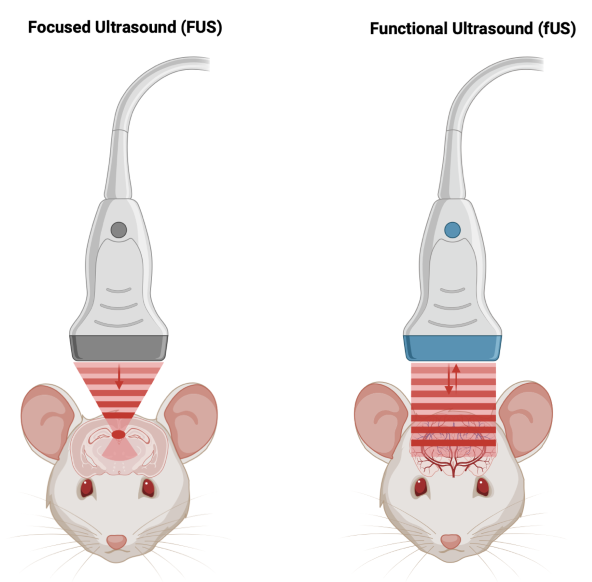
Comparison of focused ultrasound (FUS, left) and functional ultrasound (fUS, right), showing how the energy in FUS is focused on a single spot, in contrast to the unfocused plane-wave used in fUS (and the resulting reflections that are used to create an image). The lower-case ‘f’ in fUS is used by analogy to functional magnetic resonance imaging (fMRI). Image Credit: Iconeus
Comparing FUS and fUS
The table below provides an at-a-glance comparison of FUS and fUS.
Source: Iconeus
| Category |
Focused ultrasound (FUS) |
Functional ultrasound (fUS) |
| Main purpose |
Tumor therapy and neuromodulation |
Neurovascular/neurofunctional imaging |
| Ultrasound frequency |
About 0.2–3 MHz |
Typically 15 MHz |
| Energy focusing? |
Yes (‘transmit focusing’ used) |
No (‘transmit focusing’ not used) |
Energy concentration
at target |
High |
Low |
| Reflections detected? |
No |
Yes |
Typical volumes
involved |
A cylinder, a few mm wide × a few cm long |
Usually up to about 2 × 2 × 2 cm, larger volumes with specialized probes |
Applicable body
regions |
Body-wide, including the brain |
Brain, rarely the spinal cord |
| Clinical? |
Clinical therapies are well-established or under investigation |
Currently preclinical, but clinical applications are being advanced |
Combining FUS and fUS: Improving understanding of therapeutic effects
Despite its long history, the use of FUS at low intensities to modulate brain function has been hindered by a lack of in vivo studies providing detailed insights into its cellular effects and the capacity to induce microscopic displacement of neuronal tissue.
These challenges are largely due to the limitations in current brain imaging systems. fMRI is expensive and difficult, while conventional (B-mode) ultrasound imaging faces limitations in contrast resolution in soft tissues like the brain. Imaging is generally performed after the FUS pulse has completed. As a result, only information on transient effects can be obtained.
fUS provides a more information-rich imaging approach in preclinical models. However, due to its capacity to image blood flow at high resolution and in real time. It also offers much greater operational convenience.
fUS can also be used alongside FUS. A 2024 study published in Nature Communications generated fUS data showing correlations between FUS in the mouse brain and acoustic pressure, sonication duration, and pulse duration.1,2
The paper’s authors highlighted the importance of this link: “We anticipate that the insights developed in this study will provide more guided and effective FUS neuromodulation.”
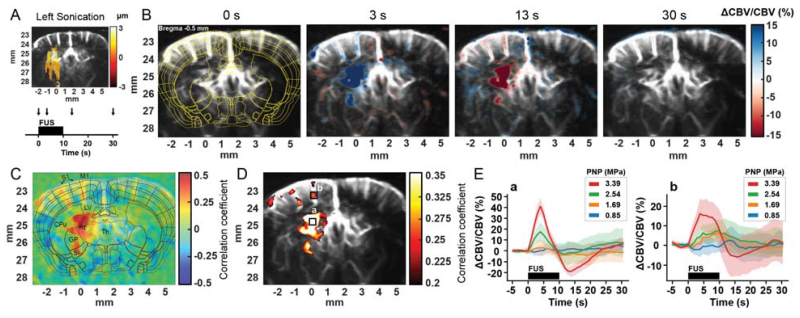
Functional responses to focused ultrasound stimulation. Functional ultrasound (fUS) imaging reveals that focused ultrasound (FUS) induces measurable hemodynamic responses in the brain. (A) Experimental setup showing targeting and stimulation timeline. (B) Representative blood volume changes at different time points following stimulation. (C–D) Activation maps highlighting regions responding to the stimulus. (E) Quantification of the response amplitude under different stimulation intensities, shown as mean ± standard deviation. Figure reproduced without modification. Image Credit: Kim, S., et al. (2024)2
Conclusion
Functional ultrasound has been widely and historically referred to as ‘fUS’ by both its developers and users. It should ideally be referred to as ‘fUS imaging’ or ‘fUSI’ in the future to clarify its differences from FUS therapy.
This distinction will be increasingly important as the different roles of ultrasound in medical science become better understood by clinical practitioners and researchers.
This work will also be essential as the simultaneous use of FUS and fUS becomes more widely studied.
References and further reading
- Kim, S., et al. (2024). Functional ultrasound (fUS) imaging of displacement-guided focused ultrasound (FUS) neuromodulation in mice. NeuroImage, 298, pp.120768–120768. DOI: 10.1016/j.neuroimage.2024.120768. https://www.sciencedirect.com/science/article/pii/S1053811924002659?via%3Dihub.
- Kim, S., et al. (2024). Functional ultrasound (fUS) imaging of displacement-guided focused ultrasound (FUS) neuromodulation in mice. bioRxiv (Cold Spring Harbor Laboratory). (online) DOI: 10.1101/2024.03.29.587355. https://www.biorxiv.org/content/10.1101/2024.03.29.587355v1.
Acknowledgments
Produced from materials originally authored by Iconeus.
About Iconeus
Iconeus is a Paris-based company, founded by the inventors of functional ultrasound, who have invented an easy-to-use functional ultrasound system for imaging cerebral blood flow and microvasculature. Its unique combination of sensitivity, speed, and high resolution has enabled it to lead the field in preclinical studies on awake animals, and it is now being proposed for applications in clinical research too.
Iconeus is introducing functional ultrasound neuroimaging: a breakthrough imaging modality for brain activity monitoring based on blood flow imaging with ultra-high sensitivity.
For preclinical research, the portability and high versatility of their technology enable the study of brain activity at unprecedented scales and in a large variety of subject states: awake, behaving, freely-moving, resting-state, and asleep conditions.
Iconeus' technology can be easily combined with other complementary modalities, such as EEG headstage or optogenetics, which are inherently difficult to combine with FMRI. Iconeus also offers key applications such as functional connectivity assessment between brain structures (connectomics) or stroke 4D monitoring. Building on years of preclinical expertise and research, they're now investing and supporting exciting new clinical applications.
Sponsored Content Policy: News-Medical.net publishes articles and related content that may be derived from sources where we have existing commercial relationships, provided such content adds value to the core editorial ethos of News-Medical.net, which is to educate and inform site visitors interested in medical research, science, medical devices, and treatments.