Acne is a common skin condition that occurs when the hair follicles on the skin become clogged with oil and dead skin cells. It typically appears as pimples, blackheads, or whiteheads on the face, neck, chest, and back. Acne can range in severity from a few mild blemishes to a more severe and persistent condition that can cause scarring.
It is most common during puberty and can be triggered by various factors, including hormonal changes, genetics, certain medications, and stress. While acne is not a serious health condition, it can be emotionally distressing and may affect a person's self-esteem. Various treatments are available to help control and manage acne, including topical creams, oral medications, and procedures such as chemical peels and laser therapy.
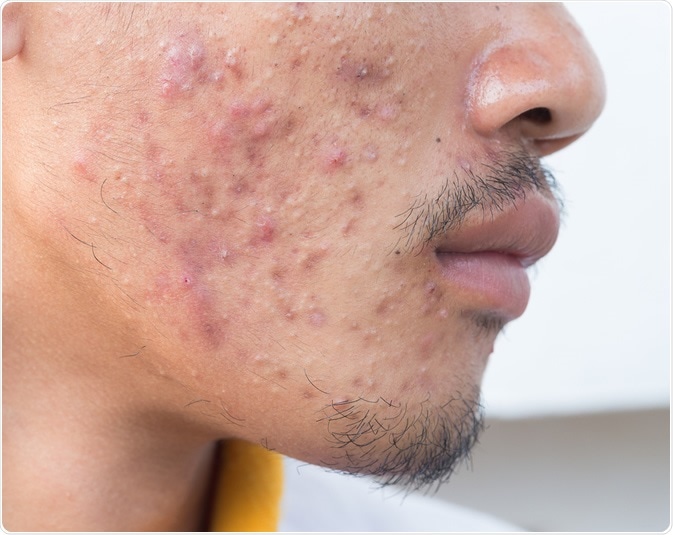
Man with problematic skin and scars from acne. Image Credit: frank60 / Shutterstock
Risk Factors
Several factors can increase a person's risk of developing acne:
-
Hormones: Hormonal changes, such as those that occur during puberty, pregnancy, and menopause, can stimulate the production of oil in the skin and increase the risk of acne.
-
Genetics: If someone in your family has had acne, you may be more likely to develop it as well.
-
Medications: Certain medications, such as corticosteroids and lithium, can increase the risk of acne.
-
Cosmetics: Using heavy or greasy cosmetics or not properly removing makeup can contribute to the development of acne.
-
Diet: Some research suggests that a diet high in refined sugars, dairy products, and processed foods may be linked to an increased risk of acne.
-
Stress: Stress can disrupt the balance of hormones in the body and may contribute to the development of acne.
-
Environment: Pollution and other environmental factors may contribute to the development of acne.
It's important to note that while these factors can increase the risk of acne, they do not necessarily cause acne in every person.
In keeping with this, the following indicators have been found to be associated with acne in males:
-
A higher body mass index (BMI) and waist-hip ratio (WHR) correlate with greater body fat
-
Higher levels of blood pressure, both systolic and diastolic
-
Higher basal glucose concentrations
-
Higher insulin levels when challenged with an oral glucose tolerance test (OGTT)
Insulin Resistance and Acne
In some patients with acne, there is the existence of a metabolic derangement that revolves around the presence of insulin resistance. Treating insulin resistance would, therefore, be a key target in preventing acne exacerbations in young males.
Reducing the glycemic load in food has been suggested and proven in many patients to help decrease the incidence of acne. This may be because of the following factors:
-
Increased glycemic load increases the insulin requirement, is associated with hyperphagia (i.e., extreme drive to consume food) and obesity, as well as increased levels of free fatty acids in the blood
-
Insulin production may cause increased androgen secretion and potentiate androgenic effects by inducing the enzymes in steroidogenic pathways and by stimulating the secretion of gonadotropin-releasing hormone and increased sex hormone binding globulin
-
Insulin decreases the level of insulin-like growth factor 1 (IGF-1) binding protein, leading to increased activity of IGF-1, which stimulates cell proliferation
These effects of insulin produce the following changes:
-
Basal keratinocytes within the duct of the hair follicle proliferate
-
Superficial keratinocytes in the follicle are shed excessively
-
Increased androgen activity stimulates sebum secretion
-
The blocked follicle is colonized by Propionibacterium acnes with resulting inflammation
This is further supported by the well-known finding that females with polycystic ovarian syndrome (PCOS) have a higher prevalence of acne. The earliest metabolic disturbance here is insulin resistance, and it is associated with hyperinsulinemia and high androgen levels, with high IGF-1 and low sex hormone-binding globulin (SHBG) levels. When oral hypoglycemic agents are used to treat PCOS, it helps increase tissue sensitivity to insulin and thereby reduce acne.
Low-Glycemic Diet in Acne
Some research suggests that following a low-glycemic diet may benefit people with acne. The glycemic index (GI) is a measure of how quickly a food raises blood sugar levels. Foods with a high GI raise blood sugar levels quickly, while those with a low GI have a slower, more gradual effect on blood sugar.
A low-glycemic diet is rich in whole, unprocessed foods and limits foods high in refined sugars and carbohydrates, which have a high GI. Some studies have found that a low-glycemic diet may help to improve acne by reducing insulin and androgen levels, which are thought to be involved in the development of acne.
It's important to note that while a low-glycemic diet may be beneficial for some people with acne, it is not a cure-all and may not work for everyone. Other factors, such as genetics, hormonal changes, and skincare habits, may also play a role in the development of acne. Additionally, while some foods may be more likely to trigger acne in some people, there is no one-size-fits-all list of "good" and "bad" foods for acne. Speaking with a healthcare provider or registered dietitian for personalized dietary recommendations is important.
Other Hormones in Acne
Assessing the levels of testosterone, as well as other androgenic hormones, and the sex hormone binding globulin showed that individuals with and without acne had no major differences in these hormones, but serum estradiol levels were higher in acne patients. This might trigger other thymic hormones which cause acne outbreaks as an inflammatory response to sebum production or infection with Propionibacterium acnes.
Another hormone that might play a role in the pathogenesis of acne is luteinizing hormone (LH) which seems to have a more sustained period of action in a subsection of male patients than in unaffected males. In most males, LH falls steadily over time as growth occurs. Another study suggested that LH levels determine serum testosterone levels in acne patients and therefore correlate with acne outbreaks. This subgroup of men with chronic acne is either hyperresponsive to LH or has a greater total mass of androgen-secreting glandular tissue.
Management
Oral contraceptives have proven to benefit some girls because they reduce androgen production due to suppressing pituitary gonadotropin secretion. Danazol may play the same role in males without the associated estrogenic effects because it also inhibits gonadotropin production. It is currently used to treat refractory male acne when topical agents and systemic antibiotics have not proven successful. However, the effect is limited to when the patient is on the drug, as acne promptly rebounds when it is stopped. Side effects are usually mild in males, though the drug can cause androgenization in females.
Another useful drug is antiandrogen cyproterone acetate. It inhibits sebum production and thus prevents acne outbreaks. However, it is not used as a first-line treatment. Furthermore, it may cause breast lumps, which resolve when treatment is stopped. Its effects are not permanent, however, and relapse is extremely common.
A cautionary note regarding the use of tetracycline in severe acne is in order. Though effective in clearing comedones, some research has exposed an unexpectedly higher risk of prostate cancer in treated men. The contribution of tetracycline to the pathogenesis of this condition in men with acne is yet to be fully elucidated.
Several steps can be taken to manage acne:
-
Use a gentle cleanser: Choose a mild, non-abrasive cleanser to wash your face twice daily. Avoid using harsh scrubs or overly hot water, as these can irritate the skin and make acne worse.
-
Keep your skin moisturized: Acne-prone skin can be dry and sensitive, so it's important to use a moisturizer to keep the skin hydrated. Look for products that are oil-free and non-comedogenic, which means they won't clog pores.
-
Use non-comedogenic makeup and skincare products: Choose makeup and skincare products labeled as non-comedogenic, which means they won't clog pores.
-
Avoid picking or squeezing pimples: Picking or squeezing pimples can cause inflammation and lead to scarring. It's best to leave pimples alone and let them heal independently.
-
Use acne-specific treatments: There are several over-the-counter and prescription treatments available to help manage acne, including topical creams, gels, and lotions that contain ingredients such as benzoyl peroxide, salicylic acid, and retinoids. These treatments can help to unclog pores and reduce inflammation.
-
Seek medical treatment: If self-care measures are ineffective in managing acne, a dermatologist or other healthcare provider can provide additional treatment options, such as oral medications or procedures such as chemical peels or laser therapy.
It's important to be patient when managing acne, as it can take time to see results. It's also important to follow a consistent skincare routine and avoid triggers that may worsen acne, such as wearing heavy makeup and not properly removing it.
References
Further Reading
Last Updated: Dec 19, 2022