Amniocentesis is a prenatal diagnostic procedure in which a minute amount of amniotic fluid is extracted and tested for chromosomal anomalies in the fetus. The amniotic fluid is the fluid that surrounds the fetus in the uterus, within the amniotic sac. It is secreted by the amniotic membrane and has several nutritive and protective functions. It is generally carried out between 15 and 20 weeks of pregnancy, as doing it earlier would cause a higher risk of miscarriage.
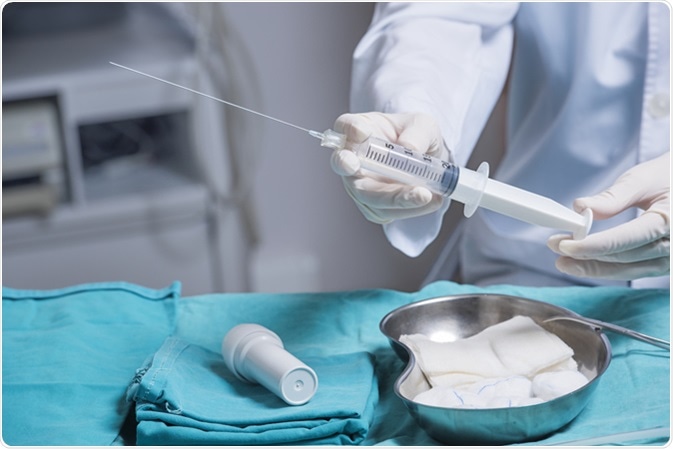
Preparing an amniocentesis needle for amniotic fluid extraction. Image Credit: Thomas Andreas / Shutterstock
The Procedure
In amniocentesis, the procedure is explained first and then the patient must give informed consent by signing a form after reading it through. No special precautions are necessary before the start of the procedure, but any medical or other allergies must be communicated to the doctor beforehand, as well as details of all current medications (prescribed or otherwise) and supplements. A history of bleeding disorders should also be made known.
An important step is to tell the doctor if the patient is Rh negative, to enable prophylactic immunoglobulin to be given before the procedure and thus prevent Rh sensitization, which may be disastrous in its effects, sometimes in the current pregnancy and often in succeeding pregnancies. The urinary bladder should be full in most cases to help elevate the uterus and increase the success rate of the procedure.
Once the patient is prepared for the procedure, the vital signs are checked, and an ultrasound examination done to confirm fetal heart rate, placental position, fetal positioning and umbilical cord location. It is also helpful in locating an amniotic fluid pocket that is not occupied by any fetal part, reducing the risk of fetal injury. After cleansing the surface of the abdomen, local anesthetic may be injected followed by the introduction of the ultrasound-guided amniocentesis needle through the anterior abdominal wall, the uterus and the amniotic sac. The uterus may cramp a little at this point. About an ounce of amniotic fluid is extracted using a syringe attached to the needle, and this is sent for testing. In 80% of women two attempts are required to get enough fluid for testing.
The needlestick site is bandaged lightly after the needle is removed, the patient and the fetus are monitored to ensure they are stable, and if the mother is Rh negative, Rhogam is administered to take care of any possible Rh sensitization.
After monitoring is completed for an hour, the patient is usually sent home. The fluid is tested for alpha-fetoprotein (AFP) to rule out some congenital defects, as well as for other metabolic disorders if indicated.
Amniocentesis
Precautions
If the patient complains of nausea, dizziness or cramping, she should be evaluated and treated accordingly. Rest is advised for 24 hours at least, but the following symptoms must be reported at once:
- Bleeding from the needlestick site
- Fluid leaking from the amniocentesis site or the vagina
- Fever with or without chills
- Abdominal pain worsens
- The fetus feels less or markedly more active especially if the procedure is carried out after the 20th week of gestation
Further Reading
Last Updated: Feb 26, 2019