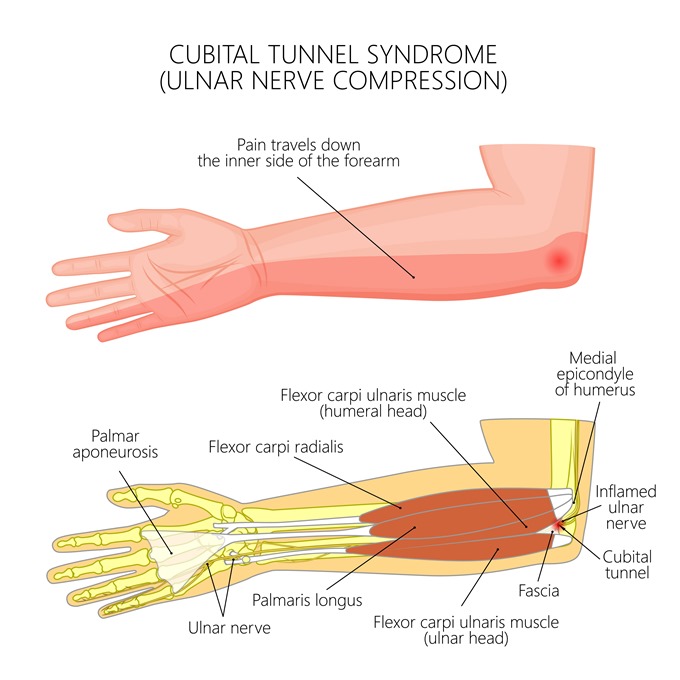
Compression of the ulnar nerve causes ulnar nerve entrapment syndrome to occur. The ulnar nerve is one of the principal nerves of the upper limb. It has a long course from the neck down into the hand, passing through the elbow, and the wrist. It is most often entrapped within the cubital tunnel, which passes beneath the medial epicondyle of the ulna.
This spot is the famous ‘funny bone,’ where even a light bump produces intense tingling or a feeling like an electric shock. Compression here leads to the cubital tunnel syndrome, the second most common entrapment neuropathy in humans. After this, the nerve is buried in forearm musculature, and emerges on the medial side of the palm, passing through Guyon’s canal. This is another less common site of entrapment.
The ulnar nerve innervates the medial side of the hand, and almost all of the intrinsic hand muscles. It also supplies some long flexors in the forearm. It is thus responsible for a great deal of wrist flexion and almost all fine hand movements.
Causes
The following are some identified causes;
- Prolonged bending of the elbow which stretches the ulnar nerve.
- In a few cases the ulnar nerve slides out from under the epicondyle when the elbow is bent. Gliding to and fro over the bone can lead to nerve irritation.
- Prolonged leaning on the bent elbow puts pressure on the ulnar nerve.
- Elbow edema may compress the nerve.
- Direct trauma to the funny bone produces temporary paresthesia.
Risk factors
Factors which increase the risk of cubital tunnel syndrome include:
- History of elbow trauma or arthritis
- Cysts of the elbow
- Occupations which demand bending of the elbow for a long time
Mechanism
Ulnar damage may be due to the direct effects of pressure against the tough retinaculum roofing the cubital tunnel, or by interference with the blood supply to the nerve.
Symptoms
Ulnar nerve compression causes numbness and tingling, or ‘pins and needles’ of the hand, specifically of the little finger. Burning and pain have also been reported. While this may occur when the elbow is bent, in some people it may occur during sleep, with the individual waking to find that the affected finger is numb. A weak grip and difficulty in performing precise hand movements may be another symptom. Muscular wasting of the hand is a late symptom and indicates irreversible damage. In advanced cases the hand becomes clawed.
Diagnosis and management
The condition is diagnosed based upon the symptoms and physical examination, including that of the cubital area. Tests may be done to detect the position in which the nerve is symptomatic, and to check for muscular weakness or sensory loss. Imaging may be required if the presence of osteophytes is suspected, as well as to rule out arthritis. Nerve conduction studies and electromyography may also be employed in some cases.
In most cases, stopping the activity which puts pressure on the nerve, preventing elbow flexion at night with a reversed elbow brace, and the use of non-steroidal anti-inflammatory drugs, will lead to improvement in symptoms.
Surgical management is advised only when muscular weakness has set in, severe compression is present, or medical measures fail to relieve the symptoms. This includes procedures such as:
- Cubital tunnel release
- Anterior transposition of the ulnar nerve
- Medial epicondylectomy
Recovery may take a few weeks to months, and physical therapy is useful to restore strength and flexibility.
References
- http://orthoinfo.aaos.org/topic.cfm?topic=a00069
- https://medlineplus.gov/ency/article/000789.htm
- https://www.betterhealth.vic.gov.au
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2599973/
- https://www.ncbi.nlm.nih.gov/pubmed/10829185
Further Reading
Last Updated: Dec 29, 2022