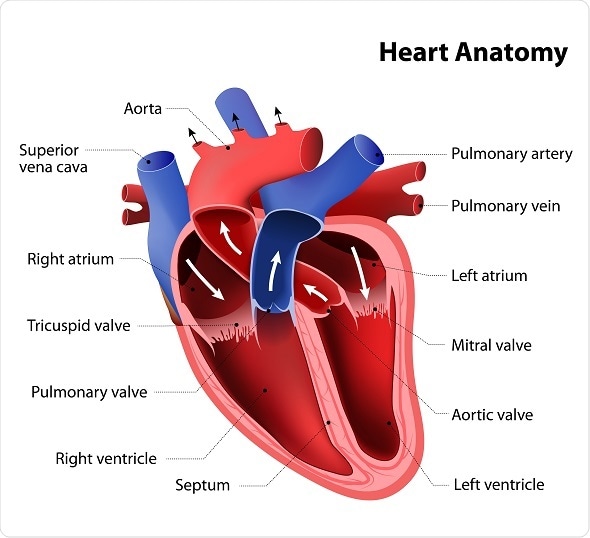
Double outlet right ventricle (DORV) is a rare congenital disorder that has a yet to be identified cause and/ or predictive factor. Infants with DORV have great arteries (i.e. the aorta and pulmonary artery), which both arise from the right ventricle. This is in stark contrast to the normal anatomical left and right ventricular origin of the aorta and pulmonary artery, respectively.
©Designua / Shutterstock.com
Infants may present in the first few weeks of life with bluish discoloration of the skin (cyanosis) due to poor oxygenation of the blood. Other complications such as difficulty breathing, poor feeding, and generally a failure to thrive are not uncommon. A common accompanying structural cardiac pathology with DORV is ventricular septal defects (VSD). In addition to this, patients may have pulmonary artery stenosis and transposition of the great vessels.
Workup
There are several approaches that may be used to diagnose DORV, which in some cases can be done even before the baby is born, prenatally. After birth, a physical examination is conducted on the infant and with the help of a stethoscope, cardiac murmurs (i.e. extra or unusual sounds) can be heard, which indicate an underlying pathology. In order to determine the nature of the pathology, imaging studies such as a chest X-ray, cardiac magnetic resonance imaging (MRI), and echocardiograms may be done. Electrocardiograms are also of diagnostic value.
The imaging technique most often used to diagnose DORV is echocardiography. This technique uses sound waves to create an image of the heart, which shows both great arteries predominantly committed to the right ventricle. This technique can also be used to determine the VSD in relation to the great vessels as well as the spatial relationship between the aorta and the pulmonary artery. Moreover, the presence of associated cardiac anomalies may also be identified. Prenatal fetal echocardiograms can be done to diagnose DORV.
Chest x-rays can also be done and typically tend to correlate with the clinical picture. However, they are not able to distinguish between DORV and other congenital heart defects. If there are any residual ambiguities after conducting an echocardiogram, then MRI may be used. However, MRI is particularly challenging due to the need for possible sedation and a more prolonged diagnostic process. Electrocardiograms are useful in that they produce results that indicate ventricular hypertrophy and atrial enlargement.
Management
The initial treatment of DORV depends on how severe the symptoms of the infant are at the time of presentation and also on the anatomy of the lesion. Moreover, the child’s age and the type of DORV the child presents with must also be taken into consideration. Children who are experiencing congestive heart failure will need to be hospitalized and managed aggressively with physical stress reduction, a reduction in fluid intake, and where applicable oxygen and diuretic therapy.
Ultimately, surgery, with the aim of connecting the aorta to its intended left ventricle and the pulmonary artery to the right ventricle, will be the treatment of choice for most cases of DORV. One particular type of surgery conducted is known as intraventricular repair, where a baffle (i.e., a tunnel) is created through the VSD to join the aorta to the left ventricle. This is done with the help of a patch of synthetic fiber called Darcon.
In another surgical approach, which is known as an arterial switch, the great vessels are repositioned into their normal anatomical places and the VSD is surgically closed. In cases where the left or right ventricle has a defect too severe to function normally (e.g., too small), 3 open heart surgeries will be conducted to enable a reconfiguration of the circulatory system and the heart called Fontan circulation. This requires what is called a staged reconstruction with the end result being the heart functioning with one ventricle as opposed to two.
Further Reading
Last Updated: Feb 26, 2019