Human ehrlichiosis is an acute febrile tick-borne disease that is caused by various species belonging to the genera Ehrlichia and Anaplasma. The infection is known to cause protracted fever and generalized body aches, and is characterized by leukopenia, thrombocytopenia, pancytopenia, and elevated liver transaminases.
Since this condition may be life-threatening in certain instances, early institution of treatment is pivotal. Most patients with human monocytic ehrlichiosis and human granulocytic anaplasmosis respond well to tetracycline antibiotics. Conversely, preventive antibiotic administration for ehrlichial infection is not warranted for individuals with recent tick bites/tick exposure who are not ill.
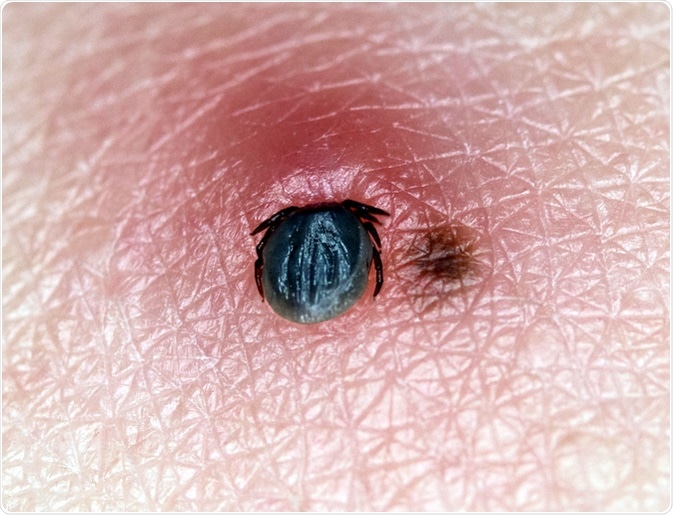
A very small tick (Ixodes ricinus) sucks blood on human skin with a birthmark. Image Credit: KPixMining / Shutterstock
Treatment Options for Ehrlichiosis
Ehrlichia chaffeensis and Ehrlichia canis, the causative agents of human monocytic ehrlichiosis, are susceptible to all tetracycline antibiotics and their derivatives. These drugs exhibit broad spectrum activity by binding to bacterial ribosomes and inhibiting protein synthesis by interrupting peptide chain formation. A plethora of other human pathogens (such as rickettsiae, borreliae, chlamydiae, as well as some mycobacterial and protozoal species) are susceptible to tetracyclines as well.
Treatment considerations for human granulocytic anaplasmosis are similar to those for human monocytic ehrlichiosis, with tetracyclines being very effective against Anaplasma phagocytophilum and Ehrlichia ewingii. The possibility of Babesia co-infection often has to be considered, which means monotherapy is sometimes not sufficient.
In both groups of diseases treatment response is usually rapid. Therefore, an alternative diagnosis should be considered if fever persists for more than 72 hours after the initiation of appropriate antibiotics. Even though research studies did not specifically address recommended treatment duration, many experts advocate continued antibiotics for 3-5 days after fever abates, and perhaps even longer (up to 14 days) if there were signs of central nervous system involvement.
A particular challenge for clinicians is ehrlichiosis in pregnancy, as tetracyclines are contraindicated in this population. Antibiotic sensitivity studies show that certain anti-tuberculous drugs have bactericidal activity in vitro against Ehrlichia and Anaplasma. This is also a viable and appropriate alternative approach in pregnant women.
Since clinical experience with other drugs that show activity in vitro is lacking, there are no fixed treatment recommendations for children younger than eight years of age, as well as for individuals who are hypersensitive to tetracycline drugs. Furthermore, there is no clinical data on the potential usefulness of adjunctive corticosteroid application to suppress the inflammatory manifestations of the disease.
Pertinent Prevention Strategies
Avoiding tick bites and removing any adherent tick immediately are the first steps in disease prevention. Individuals who reside in endemic areas are advised to wear long sleeves and light colored clothing during outdoor activities, since the latter permits easier visualization of crawling ticks. Adults at high risk of tick bites should apply repellents such as N,N-diethyl-meta-toluamide (commonly known as DEET) or permethrin to prevent this.
After visiting tick-infested regions, a careful inspection of body, hair and clothes should always be done with immediate removal of attached ticks. Research studies have demonstrated that a period lasting from 4 to 24 hours after infected ticks attach to the host is possibly essential for the successful transmission of Ehrlichia and Anaplasma. Hence, swift and thorough removal of attached ticks is of the utmost importance for preventing transmission and subsequent disease.
At the moment there are no commercially available or experimental vaccines for prevention of either human or veterinary ehrlichiosis. In conclusion, it has to be emphasized that the diagnosis of ehrlichiosis necessitates a high level of suspicion, which is why it is often made retrospectively, with potentially dire consequences for the affected individuals in rare cases.
Further Reading
Last Updated: Nov 26, 2018