The term "epidermal nevus syndrome" (ENS) is used for any of the various clinical entities which are distinctive in terms of their signs and symptoms, histopathology, and genetic composition. In most cases, they include epidermal nevi which occur along the lines of Blaschko. Other manifestations occur in the skeletal system, but more commonly in the brain and the eye.
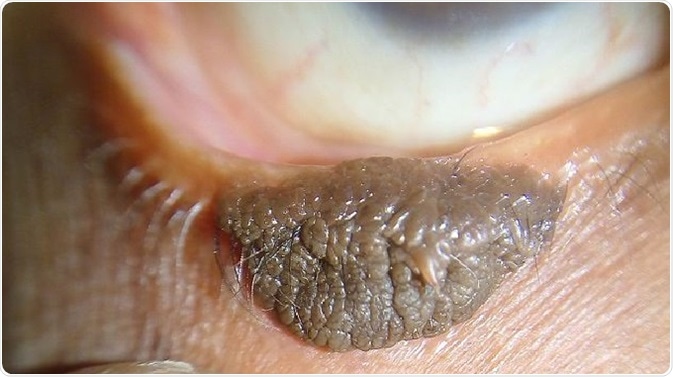
Epidermal nevus in lower eyelid margin. ©Imrankabirhossain/ en.wikipedia.org.
Nevus sebaceous syndrome (Schimmelpenning syndrome)
Also known as Schimmelpenning-Feuerstein-Mims syndrome or SFM syndrome, this consists of a sebaceous nevus with anomalies of the brain, the iris (forming a coloboma), and conjunctival lipodermoid. It does not appear to be hereditary in origin. In addition to sebaceous nevi, it includes:
- Skeletal deformities involving the trunk, face, or limbs
- Eye defects involving the cornea or conjunctiva, or resulting in a coloboma
- Brain defects which cause mental retardation, epilepsy, and shrinkage or enlargement of the brain
- Hypophosphatemic rickets resulting in bone disease due to vitamin D deficiency
Proteus syndrome
This syndrome is usually associated with a flat velvety type of epidermal nevus. It involves overgrowth of the skin, the blood vessels, fibrous connective tissue, the kidneys and lungs. Tumors may emerge later on, both malignant and benign. Both males and females are affected. The defect is probably one of the genes that regulate cell growth.
CHILD syndrome
This is confined almost always to females, because of its X-linked dominant inheritance which is lethal to males before birth. It appears in childhood. It comprises diffuse lateralization, ptychotropism, and microscopic verruciform xanthoma.
Phakomatosis pigmentokeratotica
This is apparently caused by the occurrence of two overlapping syndromes in the same individual, causing ‘twin spots; to appear. The two distinctive spots here are the sebaceous nevus and popular nevus spilus, or speckled lentiginous nevus. The nevus spilus refers to a congenital melanocytic nevus which is flat and brown in the newborn but becomes speckled with darker brown, the speckles finally becoming popular.
The syndrome overlaps with some features of Schimmelpenning syndrome as well as with the popular nevus spilus syndrome, namely, hyperhidrosis, muscle weakness, and dysesthesias.
Another variant is didymosis aplasticosebacea, which has nevus sebaceous in association with congenital aplasia of the skin. Furthermore, didymosis aplasticosebacea may occur as part of the SCALP (Sebaceous nevus, Central nervous system anomalies, Aplasia cutis, Limbal dermoid, Pigmented nevus) syndrome. Giant melanocytic nevus may also occur in this syndrome.
Nevus comedonicus syndrome
This involves cataract formation. It is non-hereditary. The comedone nevus consists of a clump of obstructed hair follicles leading to blackheads, often with pits. Other defects have been reported, such as:
- Ipsilateral cataracts
- Ipsi- or contralateral skeletal defects
- Ipsi- or contralateral neurological defects
- Pigmented hairy epidermal nevus syndrome
This includes the Becker nevus, ipsilateral mammary hypoplasia, and scoliosis or other skeletal abnormalities. The Becker nevus is a patch of dark skin, rather like a map. Dark hair grows in the mole at puberty. It is mostly found on the shoulders or upper part of the back. In addition, the individual may have poor breast/nipple development ipsilaterally, lack of subcutaneous fatty layer, and defects of muscle and skeletal symmetry.
The angora hair nevus refers to an epidermal nevus with long white soft hair, often with skeletal (facial) defects and neurological problems.
Epidermal nevus with bone cysts and hypophosphatemic rickets
This describes a condition in which there is a large extent of epidermal nevus in the body, usually to one side only, along with tumors of the bone, lungs, and skin. The bones may rupture, or form cysts. Bone fractures are common, causing deformity, due to the presence of bone cysts. Hypophosphatemic rickets can occur due to vitamin D deficiency and low phosphate.
Tumors
In addition, both benign and malignant tumors have been known to occur with epidermal nevi. It is therefore clear that the epidermal nevus syndromes are caused by the modified functioning of several genes which are defective due to the occurrence of somatic mutations in mosaic form. It is important to distinguish between the different epidermal nevus syndromes so that complications may be looked for and treated appropriately, and genetic counseling may be offered as well.
References
- http://jamanetwork.com/journals/jamadermatology/article-abstract/530551
- https://ghr.nlm.nih.gov/condition/epidermal-nevus#diagnosis
- http://www.dermnetnz.org/topics/epidermal-naevus-syndromes/
- https://www.ncbi.nlm.nih.gov/pubmed/18395670
- https://www.ncbi.nlm.nih.gov/pubmed/23622186
- https://www.ncbi.nlm.nih.gov/pubmed/7640190
Further Reading
Last Updated: Feb 26, 2019