Worldwide chronic knee, hip and back pain are the commonest causes of pain. It impairs people’s mobility, physical, mental and emotional health and wellbeing, independence, quality of life, and increases the risk of comorbidity. Care of joint pain is responsible for enormous health and social care expenditure.
Background
Despite its prevalence, joint pain is managed poorly. Guidelines recommend that people receive advice about self-management and pain-coping strategies, particularly regarding the role of exercise/physical activity and maintaining a healthy body weight in reducing pain and improving physical and mental wellbeing.
Unfortunately, few people receive this advice; most are maintained on long-term analgesia, which is often ineffective, expensive and has the risk of serious side effects. Joint replacement is restricted to people with advanced disease (about 2% of people with joint pain), expensive and contra-indicated in many older people. Consequently, people endure many years of unnecessary pain and disability.
In addition, people usually associate physical activity, such as walking, with the onset and increase of pain. They assume pain signals activity may be doing more harm than good, causing joint “wear and tear” and exacerbating pain, and begin to avoid physical activity. Unfortunately, inactivity causes joints to become stiffer, muscles weaker, and people find they can do less and less over time. It is very difficult to change people’s entrenched health beliefs and behaviours and convince them to be more active.
ESCAPE-pain
To address these issues, we developed Enabling Self-management and Coping with Arthritic Pain using Exercise (ESCAPE-pain). This a rehabilitation programme that combines giving people information and advice to help them understand their condition with an exercise programme that allows participants to experience the benefits of exercise/physical activity and its role in controlling joint pain and its impact.
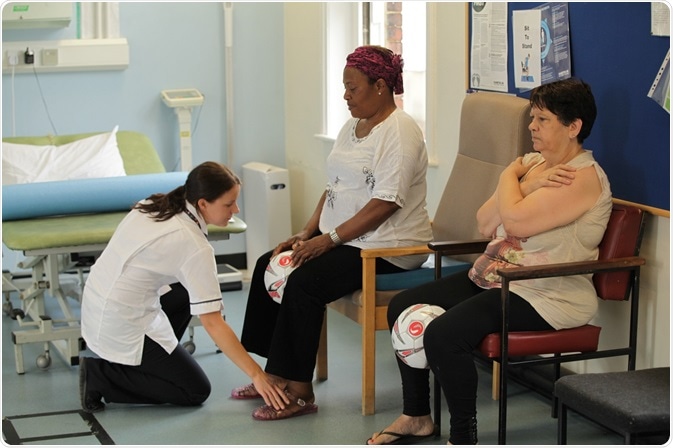
Led by a specially trained “facilitator” (physiotherapist or exercise instructor), groups of 8-12 people (45 years and over) with chronic knee and/or hip pain attend 12 sessions twice a week for six weeks. Each session comprises:
- a 20-minute education component - themed discussions and shared learning about the causes of joint pain, prognosis, advice, and pain self-management/coping strategies, such as heat/ice, rest-activity cycling, relaxation
- a 40 minute supervised exercise component where participants undertake a personalized, progressive exercise regimen to increase strength, endurance and function
Threaded into the education and exercise components are behavioural change techniques (motivational interviewing, goal-setting, action planning, positive reinforcement) to help people appreciate how physical activity can control symptoms, enabling people to regain control of their lives.
The blend of information-giving, shared-learning and experiential-learning challenge people’s beliefs about joint pain encourage them to be more active and lose weight if necessary. Clinical trials show ESCAPE-pain reduces pain, improves physical function, mental and emotional wellbeing for up to 2½ years. Participants describe improvements in pain, functional ability, walking, climbing stairs, general wellbeing, sleep quality, and socialization. They become more confident, optimistic, independent and self-reliant, rather than relying on medication, surgery and other people to help them.
Healthcare professionals in healthcare facilities usually deliver programmes like ESCAPE-pain. Given the logistic, financial, and workforce constraints on healthcare systems, this seriously limits the number of people accessing and benefiting from such programmes.
Moreover, healthcare systems cannot provide ongoing support to help people continue to be active to retain a programme’s benefits. Therefore we trained exercise professionals to deliver ESCAPE-pain in leisure and community venues. This negates the need for healthcare facilities and professionals and enables people to remain active and exercise after completing the programme.
The outcomes and positive feedback are comparable regardless of where ESCAPE-pain is delivered or who delivers it. Consequently, some healthcare commissioners are now forming partnerships with community/leisure organizations to deliver ESCAPE-pain outside clinical settings, freeing up clinical facilities, making better use of the workforce, reducing costs and providing ongoing support.

For people unable to attend a face-to-face programme (due to personal choice, rurality, etc.) we now developed a smartphone app, online and “virtual” version of ESCAPE-pain. Despite challenges with IT issues, the need for appropriate equipment, digital exclusion of deprived or disadvantaged ethnic or socioeconomic groups, ESCAPE-pain can be delivered “remotely” as a virtual programme. Whether these digital offers are as effective as the face-to-face programmes needs to be determined.
ESCAPE-pain is helping us rethink and redesign how we deliver effective care to the large and increasing number of people with joint pain. It increases the range of professional groups who can deliver evidence-based health programmes in local communities, taking care of people with joint pain more accessible, more effective and more efficient.
Where can readers find out more information?
For information about the ESCAPE-pain programme visit www.ESCAPE-pain.org, our twitter-feed @escape_pain and #LiveBetterDoMore.
References
- Vos T, Lim SS, Abbafati C, et al. Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 2020; 396: 1204–1222.
- National Institute for Health and Clinical Excellence. Osteoarthritis: the care and management of osteoarthritis in adults , http://www.nice.org.uk/guidance/cg177 (2014).
- Ganz DA, Chang JT, Roth CP, et al. quality of osteoarthritis care for community-dwelling older adults. Arthritis Rheum 2006; 55: 241–247.
- Hippisley-Cox J, Coupland C. Risk of myocardial infarction in patients taking cyclo-oxygenase-2 inhibitors or conventional non-steroidal anti-inflammatory drugs: population based nested case-control analysis. BMJ 2005; 330: 1366–1369.
- Hippisley-Cox J, Coupland C, Logan R. Risk of adverse gastrointestinal outcomes in patients taking cyclo-oxygenase-2 inhibitors or conventional non-steroidal anti-inflammatory drugs: population based nested case-control analysis. BMJ 2005; 331: 1310–1316.
- Hurley M, Walsh NE, Mitchell H, et al. Long-term outcomes and costs of an integrated rehabilitation program for chronic knee pain: A pragmatic, cluster randomized, controlled trial. Arthitis Care Res 2012; 64: 238–247.
- Hurley M, Walsh N, Bhavnani V, et al. Health beliefs before and after participation on an exercised-based rehabilitation programme for chronic knee pain: Doing is believing. BMC Musculoskelet Disord 2010; 11: 31.
- Pearson J, Walsh N, Carter D, et al. Developing a Web-Based Version of An Exercise-Based Rehabilitation Program for People With Chronic Knee and Hip Pain: A Mixed Methods Study. JMIR Res Protoc 2016; 5: e67.
About Professor Mike Hurley
Professor Mike Hurley qualified as a physiotherapist at Kings’ College Hospital in 1985. After completing his PhD at University College London he was Lecture, Reader and Professor at Kings College London between 1990-2010. Since 2010 he has been Professor of Rehabilitation Sciences at St George’s University of London and Kingston University..jpg)
He has authored over 100 research papers.
He has served as Clinical Advisor to Arthritis Research UK (2002-2008), Chair of Chartered Society of Physiotherapy’s Research and Clinical Effectiveness (2001-2004), has contributed to several national working groups, clinical guideline committee and conferences.
Between 2013-2021 he was seconded as Clinical Director for the Musculoskeletal Programme of the Health Innovation Network. In 2021 he was appointed Clinical Director of the ESCAPE-pain programme at Orthopaedic Research UK.
A major part of his work was the development of ESCAPE-pain – a rehabilitation programme to help people with knee, hip and back pain that is delivered in clinical and community venues across the UK. ESCAPE-pain has won many accolades, endorsements and awards including 2020 Health Service Journal’s Musculoskeletal Condition Initiative of the Year, and the 2021 Self Care Forum Innovation of the Year in 2021
Last Updated: Dec 14, 2021