Hepatitis is a condition caused by many different agents, both living and nonliving. The most common infective causes include the hepatitis viruses, such as hepatitis A, hepatitis B, and hepatitis C. The hepatitis C virus causes inflammation of the liver. There are a variety of substances and conditions that can render the liver vulnerable to hepatitis C, including extensive drinking, other infections, certain diseases, and even certain therapeutic agents.
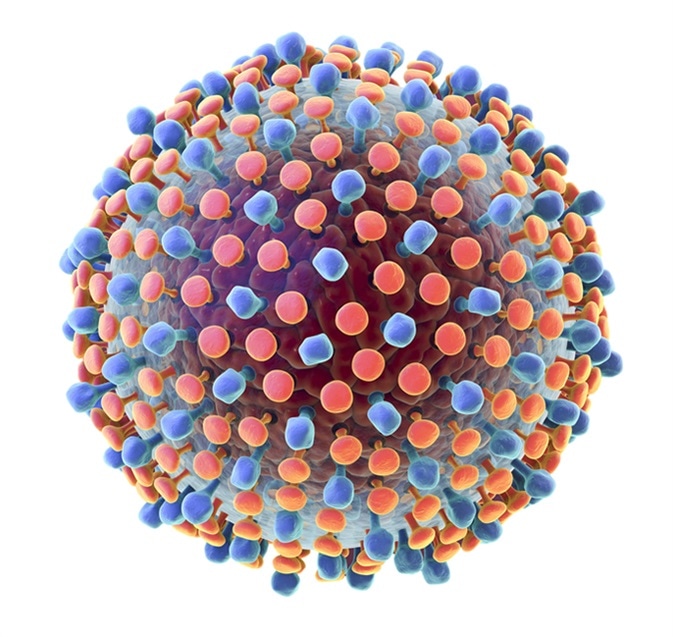
Hepatitis C virus model, 3D illustration. A virus consists of a protein coat (capsid) surrounding RNA and outer lipoprotein envelope with two types of glycoprotein spikes, E1 and E2. Image Credit: Kateryna Kon / Shutterstock
The virus that brings on hepatitis C can cause both acute and chronic hepatitis. Acute hepatitis is may be a mild illness lasting a few weeks. It may resolve or evolve into a serious, lifelong condition that must be dealt with. It has been estimated that in 2015, there were more than 1.7 million new infections with hepatitis C. More than 70 million people have the chronic form of hepatitis C. Eventually many of these chronic cases will develop liver cancer or cirrhosis. Cirrhosis of the liver occurs when scar tissue replaces normal, healthy tissue in the organ.
Nearly 400,000 people die annually from hepatitis C, most often from cirrhosis or primary malignancy of the liver. Antiviral drugs have the potential to cure more than 95% of those who have hepatitis C, lessening the risk of death from liver cancer and cirrhosis. Unfortunately those who have the condition may not know it, and the rate of diagnosis and treatment is low. There is no vaccine for this condition.
Hepatitis C (HCV) Lifecycle - Medical Animation
Transmission
The virus that brings the hepatitis C infection is found in blood or bodily fluids, making hepatitis C a blood-borne virus. There are a number of ways in which transmission of the virus occurs, including:
- Sharing drug-injecting systems, including syringes or needles
- The reuse of syringes or needles
- The use of poorly sterilized syringes or needles
- Intercourse with an infected individual, although this is a less common route of infection
- The use of poorly screened or unscreened blood components – red blood cells, plasma -- during a transfusion
Any infected blood spills, even if they are dry, must be cleaned with a bleach-based solution. This is because the virus can survive on surfaces at room temperature for nearly a month.
Moreover, it is possible that hepatitis C can be transmitted from an infected woman to her fetus. In addition, the chances of contracting hepatitis C increase if a person has had more than one sex partner in the previous six months, has a history of sexually transmitted disease, or is a male homosexual, among other risk factors.
The virus is not transmitted through casual contact, such as kissing or sharing food with an infected individual. It is not transmitted through breast milk. It cannot spread by sharing drinking cups and utensils with an infected person, or by hugging or shaking hands.
The current and growing interest in body tattooing and piercing, also called body art, has raised concerns about the spread of this virus through these means. Some research has shown that hepatitis C is not spread by instruments at properly licensed commercial tattoo parlors. But transmission could occur in unlicensed establishments where there may be poor sanitation management. Informal tattooing already occurs in prisons or other informal settings. Additional research could help determine if these types of informal tattooing environments may be sites for transmitting hepatitis C.
25 Years From Discovery To Cure: The Hepatitis C Story | Nezam Afdhal | TEDxOxford
References
Further Reading
Last Updated: Dec 29, 2022