Kyphosis represents an abnormal curvature of the upper spinal region that often leads to slouching in childhood and can worsen with age, especially during the pubertal growth spurt. Specific treatment for kyphosis is determined based on the age of a patient, overall medical history, the extent of the condition, tolerance for specific medications, therapies and procedures, as well as the expectation for the course of the disease.
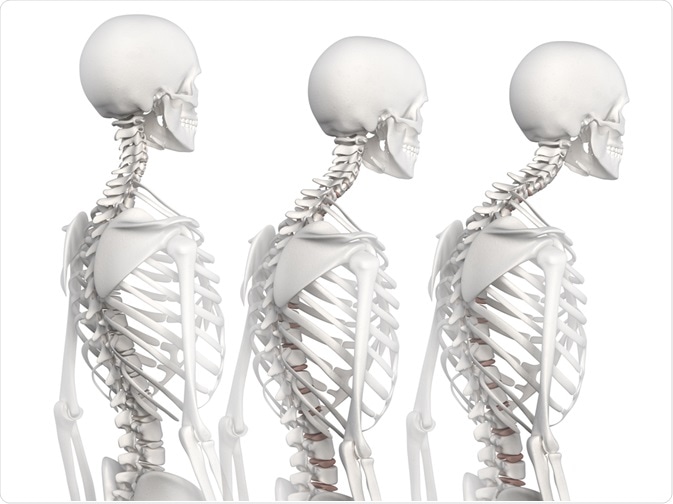
Image Credit: CLIPAREA Custom Media / Shutterstock.com
The end goal of all treatment protocols is to stop the progression of the curve and prevent deformity. A myriad of conventional orthopedic and surgical treatments are available; therefore, the strategy should be tailored to the needs of each individual patient. As early detection of kyphosis is pivotal for successful treatment of this condition, pediatricians or family physicians routinely look for signs of eventual kyphosis in children.
Conservative treatment of kyphosis
Physical therapy is often prescribed to improve posture by strengthening the trunk muscles and stretching the hamstring muscles. A well-designed exercise program may also serve to alleviate kyphosis-related pain in many patients. Learning correct body mechanics to preserve erect posture, retaining high levels of activity, sticking to regular non-jarring exercises such as swimming, and daily stretching exercises are customary initial steps in treating kyphosis.
Bracing is the cornerstone of the orthopedic treatment of kyphosis with the goal of correcting and stabilizing the deformity. The brace is worn while the bones are still growing and it should decrease the curvature of the spine by more than 15 degrees. In patients with kyphosis, the most widely used devices are the Milwaukee brace and the kyphosis bivalve brace.
Brace treatment is largely successful in patients with kyphosis between 55 and 80 degrees if the diagnosis is made prior to skeletal maturity. In order to improve the patients’ quality of life and compliance while wearing the brace, attempts have been made to reduce material burden without the loss of desired in-brace correction.
Before any kind of bracing is prescribed, in some cases, there is a need for a cast in order to correct a marked and rigid kyphotic deformity. When there is no risk of spinal cord compression or instability, the preferable approach in patients with severe and rigid kyphosis is a gradual correction of the deformity in order to decrease the risks of surgery, facilitate the surgical treatment itself, and ameliorate post-surgical outcomes.
Surgical approach
When kyphosis is so severe that it necessitates surgery, many different procedures are considered. As each case of kyphosis is somewhat different, a very specialized approach is required for optimal results. In addition, surgery should not just aim to straighten the spine but to also solve the problems brought on by kyphosis.
A common surgical choice for a progressive kyphotic distortion is a solid fusion or arthrodesis of the deformed vertebrae. Such fusion may also include one normal vertebra above and one normal vertebra below the affected area. On the back of the spine and along the area of the abnormality, a bone graft is placed posteriorly, although the anterior placement of an additional graft is sometimes pursued in severely angulated curves.
Surgery can also include instrumentation in the form of hooks, rods, and screws, which helps to correct the deformity in progressive kyphotic cases of older children. If the spinal cord is deemed unable to tolerate certain manipulative techniques that aim to straighten the spine, the removal of the misshapen vertebrae to realign the spine can be considered.
In addition, an osteotomy, which is a bone-cutting procedure that re-aligns the spine, is often recommended. The Smith-Peterson osteotomy is performed at multiple levels to allow secure implementation of additional corrective forces. In this procedure, the facets are removed and the spine is bent backward further than normal. Although there is only a little bit of correction that can occur over one level (up to 15 degrees), multiple levels of large amounts of correction can be achieved.
As with any other surgery, there is a risk of ensuing complications which can be very serious. The most common complications include pulmonary impairments, nerve injuries, as well as infectious and mechanical complications. Delayed complications consist of loss of correction, implant fractures, junctional kyphosis, and late osteoarthritis under the fused segment. Complications could also involve subsequent pain and the need for additional surgery.
Further Reading
Last Updated: Apr 7, 2023