Rheumatic heart disease (RHD) is a major cause of chronic and serious ill-health in developing countries. It is responsible for a leading share of heart disease in children and young adults, accounting for a quarter of a million deaths a year. It is actually an autoimmune disease, caused by the body’s abnormal reaction to an ordinary streptococcal Group A infection of the throat.
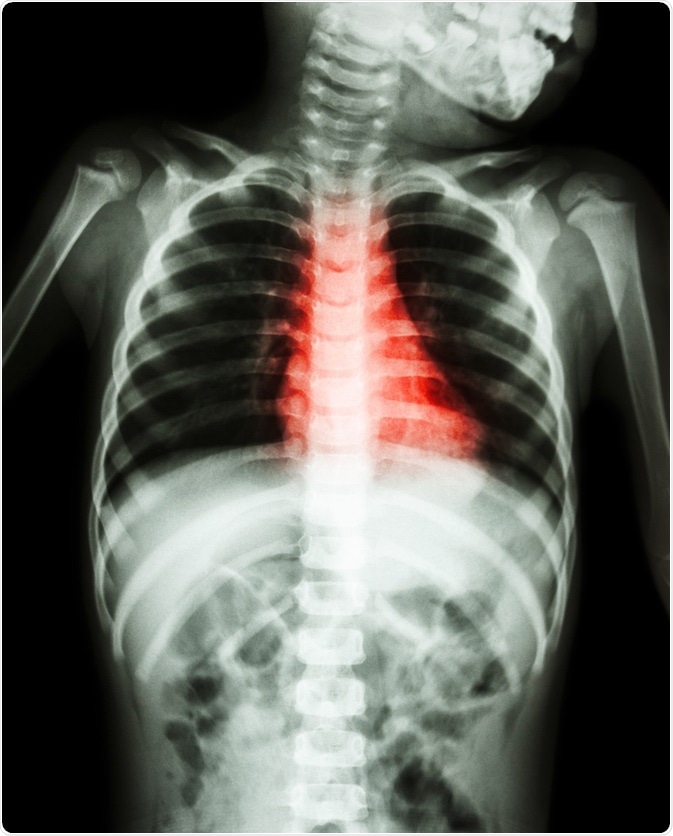 Credit: Puwadol Jaturawutthichai/ Shutterstock.com
Credit: Puwadol Jaturawutthichai/ Shutterstock.com
This occurs in certain individuals much more readily, due to their genetic make-up. The throat infection leads to the development of a generalized autoimmune disorder called acute rheumatic fever (ARF).
The autoimmune antibodies latch on to and progressively destroy the tissue forming the heart valves, leading to RHD. This is usually asymptomatic for 10-20 years because the heart compensates in various ways to pump enough blood to the body, despite the valve damage. Eventually, however, progressive damage leads to heart failure.
Incidence
RHD affects mostly poor populations, with overcrowding and undernutrition being associated risk factors. Those affected by the initial ARF are children between the ages of 5 and 14 years, though it may strike even younger children. Recurrences of ARF may continue into young adult life. ARF occurs equally often in males and females, but RHD is much more common in females.
The reason is not known, but may be because of generally reduced female access to health care and food, as well as the increased likelihood of RHD becoming symptomatic during pregnancy when greater demands are placed on the heart.
RHD generally becomes symptomatic in the twenties and thirties, with most of the remaining RHD burden falling on children and adolescents.
Progressive disease
Even after the acute infection has been controlled, persistent inflammation continues to wreak havoc on the valves. RHD complicates ARF in about 30-45% of patients, with damage involving the pericardium, endocardium and sometimes the myocardium – all three layers of the heart.
The only permanent damage is to the endocardium of the valves, which become scarred and thickened. This interferes with the normal pumping function of the heart leading to the onset of breathlessness with exertion, rapid feelings of tiredness, chest pain in some cases and eventual heart failure.
Clinical features
Multiple valves are affected by RHD, mostly the mitral, aortic and tricuspid valves. The involvement of the mitral valve is almost 100%, while the aortic valve is damaged in a third of cases. Thickening of the valve occurs, which may lead to either restricted outflow or abnormal backflow through the valve opening.
This puts extra strain on the chambers on either side of the opening, reduces cardiac output of blood to the body circulation, and hinders proper exchange of oxygen and carbon dioxide through the lungs.
Mitral regurgitation is a condition in which the mitral valve allows blood to flow back into the left atrium when the left ventricle starts to pump blood. This eventually leads to left heart failure with dilation of the left sided chambers of the heart.
This is the lesion most commonly observed in RHD, usually in combination with other valve diseases. Mitral stenosis, aortic regurgitation and less commonly, aortic stenosis, are other components of the RDH spectrum.
Prevention of RHD
The prevention of RHD is a prime concern for medical professionals based with this huge burden of disease, and several levels of prevention have been described in detail. The most commonly adopted measure is antibiotic prophylaxis with penicillin, a drug highly active against group A streptococci, by which means the recurrence of ARF can be prevented.
Screening measures using echocardiography are also being discussed to allow early detection and treatment of high-risk populations before clinical disease sets in.
Management
Medical management for RHD is only effective to control cardiovascular symptoms in early cases. RHD may remain silent for years or decades because of compensatory changes in the heart. Secondary prevention with long-acting penicillin G or other effective antibiotics should be strictly enforced to reduce the risk of recurrence of ARF with resulting RHD complications.
Once heart failure sets in, surgery is the only option unless the patient has no access to surgery or is unfit for it. Lifestyle changes are relevant to allow the maximum freedom from symptoms.
Prevention of endocarditis is another important precaution to be observed in patients with RHD, when they are faced with invasive procedures, and especially after surgical treatment with prosthetic heart valve replacement, valve repair, or if they already have had one or more episodes of endocarditis.
The management of RHD is primarily surgical once signs of declining left ventricular function or symptoms relating to poor heart function set in. Both balloon procedures to dilate narrowed valves, or valve replacement for irreparably damaged valves, are commonly practiced.
Complications
Patients with mitral stenosis may develop clots in the stagnant blood within the left atrium. These may break off and travel within the blood vessels to block various important blood vessels within the body, resulting in stroke, heart attacks or pulmonary embolism. Anticoagulation is needed if an atrial clot is present.
Dilation of the left atrium can cause disruption of the heart’s pacemaker in the left atrial wall, causing an irregular heartbeat called atrial fibrillation. This is most often seen in mitral stenosis, especially in older patients with elevated right atrial pressure. It increases the risk of embolism, and of ventricular arrhythmia which can precipitate acute cardiac failure because of the poor reserve of pumping action in the diseased heart.
Further Reading
Last Updated: May 24, 2019