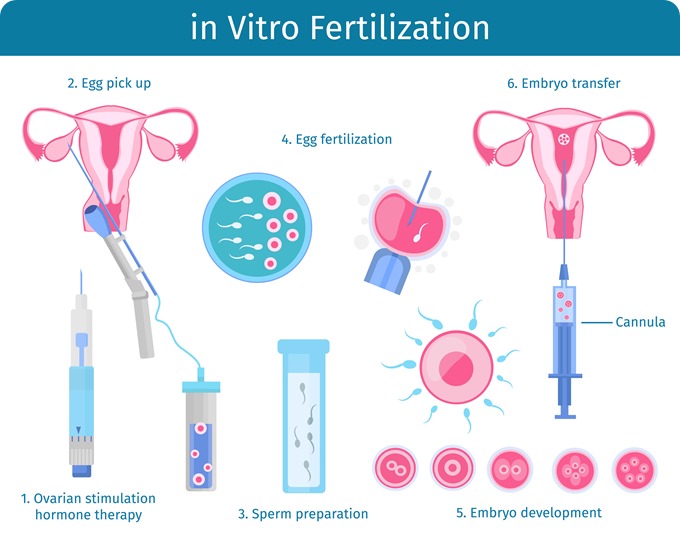
In vitro fertilization (IVF) is a multi-stage procedure which bypasses the mechanism of natural fertilization within the fallopian tubes of a woman. It attempts to achieve fusion of a sperm and an oocyte outside the body i.e. in a culture medium. It involves the following stages, each of which must necessarily be successful before the couple can hope to proceed to the next one.
©ectorPot / Shutterstock.com
Preparatory phase
Before beginning IVF, the medical center will take a careful medical history, perform a physical examination, and take informed consent from both partners. In addition, various blood tests may be ordered to exclude or detect various infections, especially those which are blood-borne or sexually transmitted.
Suppressing (downregulating) the natural hormone cycle
Women who are ovulating are treated with hormones at a suppressive dose, either in the form of a self-administered daily or nasal spray, for about two weeks.
Controlled ovarian hyperstimulation
Various protocols are used to stimulate multiple ovulations to help produce multiple embryos. In order to prevent premature ovulation due to the secondary oversecretion of gonadotropin hormones, pituitary suppression of these hormones is first achieved by pre-treatment with a long-acting gonadotropin-agonist (Lupron).
When measurements show that suppression has been optimally achieved, daily gonadotropins are injected daily to stimulate ovarian follicular development. The growth of the follicles is followed up carefully with ultrasound imaging and hormone level assays.
Once the lead follicle is big enough, which usually occurs after about 12 days, human chorionic gonadotropin (hCG) is administered to simulate the luteinizing hormone (LH) surge which triggers ovulation in the natural setting. The stage is now set for oocyte retrieval in about 36 hours.
Oocyte retrieval
Under ultrasound guidance, transvaginal follicular aspiration is performed to retrieve the oocytes from the follicles in both ovaries. The procedure is done under sedation. Side effects include mild cramping and soreness, with some vaginal bleeding. After oocyte retrieval, progesterone pessaries, injections, or gels, are prescribed to prepare the endometrium for implantation within 5 days of fertilization. The oocytes are cultured in a special media within an incubator until they are ready for insemination.
Fertilization
In this stage the oocytes and sperms are mixed and left alone for fertilization to occur, in a special medium. The method of fertilization used depends on the sperm used. Provided normal sperm is available from the partner, about 50,000 to 100,000 motile sperm are placed into the dish containing the oocytes. This is called standard insemination.
On the other hand, if normal motile sperm are not available, the intracytoplasmic sperm injection (ICSI) technique is preferred. Here, single sperm are picked out using microneedles, and directly injected into the cytoplasm of the oocyte under a high-power microscope.
This allows fertilization to proceed even in the presence of oligospermia or azoospermia, asthenospermia, or teratozoospermia. Sperm may be aspirated directly from the testicular tissue if they are absent in the sperm sample. Such sperm are always used via ICSI for fertilization in IVF because they are immature when retrieved.
intracytoplasmic sperm injection of human egg
After 16-20 hours the oocytes are examined for the success of fertilization. All the embryos formed at this stage are allowed to grow in a laboratory incubator for up to five days. At this stage they have become blastocysts.
Blastocysts are a ball of cells, much larger than the zygote, and which contain fluid. The better they expand, the higher their quality and the more chance there is that implantation will succeed.
Embryo transfer
Blastocyst transfer is carried out to increase the chances of successful implantation, since natural implantation occurs at the blastocyst stage (day 5 following fertilization). This also makes it possible to transfer one or two embryos rather than three or more, since implantation is more likely at this stage.
In contrast, if the embryos are of low quality or the level of fertilization is low, transfer is done on the second or third day itself, which is called the cleavage stage. The embryo has between four and eight cells. Embryo quality is assessed based on the number of cells, their distribution, and the presence of fragmentation.
5-Day Blastocyst Transfer
The healthiest embryos are then selected for embryo transfer. Any remaining healthy embryos may be frozen and stored for use in later cycles, if required.
The number of embryos used for transfer depends upon the age of the woman. For those over 40 years, up to three embryos may be transferred into the uterus. For women younger than this, only up to two embryos are used per cycle to reduce the risk of multiple pregnancy. Single embryo transfer is the recommended procedure in many cases.
During this procedure, the vagina is visualized with a speculum and the embryos passed down a fine catheter into the uterus, through the cervix, under ultrasound guidance. The urinary bladder is kept full in order to achieve a clear ultrasound picture. While no pain is expected during embryo transfer, the distended bladder may cause some discomfort.
Progesterone supplementation is continued until the pregnancy is confirmed, typically by testing within 12-14 days of embryo transfer.
Freezing and storage of any unused embryos is then performed after the best ones have been transferred.
IVF - male component
In men, the following steps are required:
A sample of sperm is asked for, and the sperm are washed and prepared for separation. During this process, the active or motile sperm are separated for use from the poor-quality sluggish ones.
At this time, if samples had already previously been given for freezing and storage, they are thawed and prepared for separation of the best quality sperm from the specimen.
References
- https://www.urmc.rochester.edu/
- https://medlineplus.gov/ency/article/007279.htm
- http://www.hfea.gov.uk
- http://www.nhs.uk/Conditions/IVF/Pages/How-is-it-performed.aspx
Further Reading
Last Updated: Jan 2, 2023