A pyogenic granuloma is an abnormal vascular growth, with an inflammatory component, which arises mostly over the skin of the head, arms, or neck. It may also occur at various spots inside the oral cavity.
It is painless and its main importance lies in the fact that it may give rise to sudden bleeding with quite insignificant trauma to the surface. This is because it is composed of small friable blood vessels.
In some cases, it regresses spontaneously, shrinking and losing its color within a few days as the blood vessels close. Especially with respect to oral pyogenic granulomas appearing in pregnancy, active surveillance may work well as they often resolve on their own. Pyogenic granulomas due to a specific medication are known to subside once the offending drug is removed.
However, in the majority of patients, these lesions are removed because of the trouble caused by the ready bleeding from them.
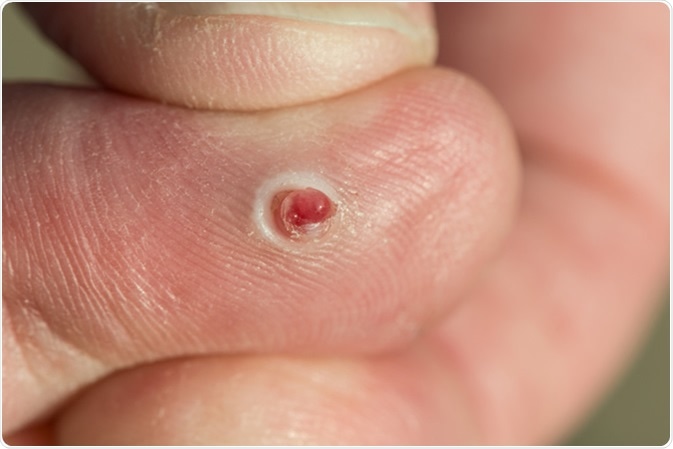
Pyogenic granuloma - Image Credit: CLS Digital Arts / Shutterstock
Modes of Treatment
Various treatment modalities exist, including:
Curettage and Cauterization
This is usually done under local anesthesia. It involves removing the lesion by sharply curetting it off the skin, followed by cauterization of the bleeding vessels left behind, which feed the hemangioma. This achieves hemostasis and also reduces the chances of the lesion re-appearing. It has the disadvantage of leaving a scar after healing.
If the granuloma is incompletely removed, it may lead to recurrence. The high rate of recurrence, which is up to 16 percent for gingival pyogenic granulomas, is because the feeding vessels extend down into the dermis in the shape of a cone, which is not always reached by the curettage.
Surgical Excision
When a pyogenic granuloma recurs after curettage, it is best excised with a deep dissection, applying sutures to approximate the skin edges. Surgical excision is the treatment of choice for gingival pyogenic granulomas, which have a higher rate of recurrence especially when arising in pregnancy. For this reason, a 2 mm margin should be preserved, and any causative agent such as a foreign body should be removed at the same time. Pyogenic granulomas in other sites rarely recur after excision. Shave excision is also practiced for this condition.
Electrocautery Excision
This method uses electric current to produce heating of the cautery tip which is used to remove the lesion. It produces good hemostasis, can be precisely controlled, but does not allow a histological diagnosis to be made.
Cryosurgery
This is a technique in which liquid nitrogen is used to freeze and destroy small pyogenic granulomas. Large ones are not suitable for removal by this method, as the amount of freezing cannot be precisely tailored or predicted, leading to inadequate removal or excessive tissue damage.
Laser Surgery
Small pyogenic granulomas may be shrunk using a carbon dioxide or Neodymium-Yttrium-Argon-Garnet (NdYAG) laser, while larger ones may be ablated and the base seared with laser energy. Laser treatment is associated with less postoperative pain, and is a less invasive procedure. It does not require sutures, as well. Other advantages include faster healing, satisfactory coagulation, the absence of the need for continued dressings, and producing marked reduction in the number of micro-organisms in the area, which prevents infection of the healing wound. A better cosmetic result may be predicted because of decreased edema, wound shrinkage, and less scarring.
These topical agents contain agents such as Imiquimod, which are also useful to treat warts and solar keratosis. They are immunomodulators. Along with a high rate of efficacy, they are particularly helpful in treating pediatric pyogenic granulomas.
- Silver nitrate is used as a chemical cautery to seal the blood vessels that comprise the lesion. It is non-invasive, and convenient to apply.
Sclerotherapy
Phenol for topical application acts as a sclerosant, closing off and coagulating the blood vessels in the hemangioma and allowing it to shrink and disappear over time. Other sclerotherapy agents include sodium tetradecyl sulfate, and monoethanolamine oleate.
Injections of Corticosteroids into the Lesion
This method of treatment avoids surgery but has not been shown to be uniformly successful.
Photodynamic Therapy (PDT)
This is another modality which depends on the action of certain light frequencies to activate photosensitizers injected into the lesion, to directly destroy the cells, both vascular and extra-vascular. It produces vascular spasm, thrombosis, and permanent occlusion, and its effects have been found to be long term.
References
Further Reading
Last Updated: Feb 27, 2019