Skip to:
What is Scarlet Fever?
Streptococcus pyogenes, which causes a disease known as ‘Scarlett Fever’, is a group A streptococci infection, and are found to be most commonly transmitted directly from person-to-person contact. Usually, transmission can occur via the nasal secretions or saliva of a person suffering from the infection.
Streptococcus pyogenes infection. Image Credit: Dragos Pop / Shutterstock
Patients with Scarlett Fever are also significantly more likely to spread the bacteria to others than carriers that are asymptomatic. Crowded places — such as day-care centres, schools, university accommodation, or military training facilities — can further facilitate the transmission of Scarlett Fever causative organisms. However rare, the transmission of these group A strep infections could also come about via food, such as an infected person coming into direct contact with ready-to-eat food just before serving – with foodborne outbreaks of group A strep having previously occurred after improper food handling procedure. Fomites, for example household items, have been found to be highly unlikely to facilitate spread this type of bacteria. There is also no evidence indicating that pets or animals can transmit this kind of bacteria to humans.
Scarlett fever can come about in all ages of people, with this condition occurring most commonly amongst children aged between 5 and 15 years old. It is a relatively rare condition to occur in children aged younger than 3 years old. Whether these kinds of group A streptococci infections will decrease, increase, or remain the same is unknown. History is awash with descriptions of outbreaks of group A streptococcal infections on a variety of scales. In the 17th century, outbreaks of scarlet fever were found to have spread from Italy and Spain all the way over to Northern Europe; and in the early 18th century, an epidemic occurred inside the American colonies, which ultimately killed over 4,000 people.
A majority of these outbreaks increased and decreased before the age of antibiotic treatments, which suggested that either variations in the expression of virulence factors by the bacteria, or changes in social/economic conditions were responsible for these changes in incidence. This concept can be best demonstrated by the extraordinary mortality rate of Scarlet Fever which were documented in the late 1880s in the US states: New York and Chicago, as well as over in Norway: 25% to 30% of children that contracted Scarlet Fever died in that time. By the 20th century, the mortality rate of this disease decreased to below 2% in all three of those locations. Seeing as the social/economic conditions were not likely to have changes significantly during that time, and since antibiotics were not an option, the drop in mortality rate was likely to have been induced by the reduced expression of one of the streptococcal virulence factors, or possibly via slow acquisition of overall herd immunity to that virulence factor.
How is Scarlet Fever Treated?
Scarlet Fever is typically treated using a 10-day course of select antibiotics. This is usually in the form of amoxicillin or penicillin tablets, whereas liquid antibiotics may be advised for younger children. For patients that have an allergy to penicillin, some alternative antibiotics such as erythromycin could be offered instead. Clinical and laboratory studies have concluded that penicillin is the most effective antibiotic treatment against haemolytic streptococci. Penicillin has previously been found to be more active against these bacteria than sulphonamides in defending mice against the lethal infections caused by this type of organism. There are a vast number of scientific reports discussing haemolytic streptococcus infections that can resisted therapy using sulphonamides, but that responded appropriately to penicillin treatments. This study, amongst many others, concluded that penicillin is one of the best antibiotics for treating patients suffering from group A streptococci infections such as Scarlet Fever.
In terms of the prevention of Scarlet Fever infection, appropriate hand hygiene measures and respiratory etiquette has been found to reduce the transmission of all types of these group A streptococci infections. Hand hygiene is particularly significant after sneezing and coughing, as well as before preparing and eating food. Typically, treating an infected patient with an antibiotic such as penicillin for around 24 hours generally eliminates the ability to the patient to spread the bacteria to others. Therefore, people suffering with Scarlet Fever should reduce person-to-person contact (e.g. stay home from work, school, or day-care) until they are both afebrile, and after at least 24 hours of starting any appropriate antibiotic treatments.
Scarlet fever is usually of mild intensity and goes away on its own in about a week without treatment. Scarlet fever is caused by Group A beta haemolytic Streptococci. In mild cases this might not cause complications but in severe infections there might be life threatening complications.
Thus, treatment of scarlet fever with antibiotics is important to prevent complications. Most people recover around four to five days after starting treatment with antibiotics. 1-8
Treatment of scarlet fever entails taking antibiotics, bed rest and so forth.
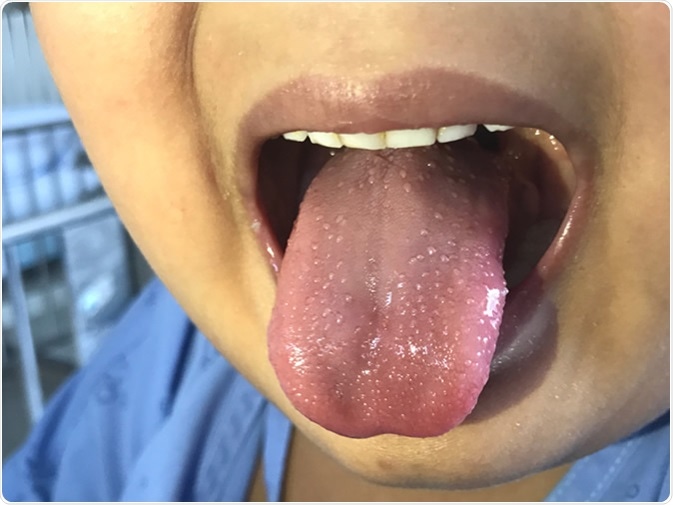
Strawberry tongue in case scarlet fever. (Strawberry tongue is the name given to a swollen, bumpy tongue. Most often, the enlarged tongue is very red, like a strawberry or raspberry.) Image Credit: Chalie Chulapornsiri / Shutterstock
Antibiotics
Usually a 10 day course of antibiotics are prescribed. Penicillin is the commonest drug of choice. Those who are allergic to penicillin may be prescribed alternatives like Erythromycin.
These days a culture and sensitivity test is done from the throat swab sample. This shows sensitivity of the stain of Streptococci to particular antibiotics. Those found effective are prescribed.
Symptoms usually go in a few days if the antibiotics are taken regularly. The fever will normally disappear within a day or two of starting antibiotics. However, all patients are advised to strictly complete their antibiotic regimen.
Scarlet Fever
Bed rest
Patient is advised to stay in bed and drinking plenty of cool (not cold) fluids like water. Warm liquids like soup or cold foods like popsicles or milkshakes also help relieve a sore throat. The room needs to be kept cool.
Relieving the fever and itching
Paracetamol/Acetaminophen is prescribed to relieve the fever and to ease the aches and pains.
A calamine lotion or other soothing lotions are prescribed to relieve itching of the rash
Complications of scarlet fever
Complications of scarlet fever include:
-
ear infections (otitis media)
-
adenitis or throat abscesses
-
inflammation and infections of the sinuses (sinusitis)
-
kidney infections (glomerulonephritis)
-
lung infections (pneumonia)
acute rheumatic fever that may cause joint pain and also affect the heart valves
These complications are usually seen if scarlet fever or streptococcal sore throat is not treated adequately with antibiotics. They need to be individually assessed and appropriately managed.
Rare complications include kidney failure, meningitis, severe toxic shock or blood poisoning or infection of the deeper tissues (necrotizing fasciitis) and bones (osteomyelitis).
Those with complications or with difficulty in swallowing may need hospitalization for intravenous antibiotics and fluids.
Prevention of scarlet fever
Prevention of scarlet fever entails:
-
Scarlet fever is highly contagious. It can spread through inhaled air borne tiny droplets with the bacteria or by touching. Children with scarlet fever need to be kept away from school and day care at least till their symptoms recede.
-
Tissues and handkerchiefs used by an infected person should be disposed or washed carefully.
-
Hand washing before and after touching infected tissues or material or after touching face or nose of an infected person is important. Toys and surfaces should be washed and disinfected daily.
-
Utensils, clothes, towels, baths etc. should not be shared with an infected person.
-
Throat cultures may be needed for the family. Usually the infection can spread to others in the family. Usually repeat throat cultures are not necessary after completion of a course of antibiotics.
Scarlet fever and pregnancy
Pregnant women usually do not carry a risk of passing on any harmful effects to their unborn babies if they get this infection. However, care must be taken to isolate pregnant women and the elderly from people and children with the infections.
Adults and children over 10 rarely get Streptococcal throat infections but may be carriers of the infection.
Further Reading
Last Updated: May 29, 2023